Effects of the ACA Medicaid Expansion on Racial Disparities in Health and Health Care
Executive Summary
The disparate impacts of the COVID-19 pandemic on people of color have exposed and compounded underlying racial/ethnic disparities in health and health care. These disparities include longstanding higher uninsured rates among people of color that contribute to barriers to care and, ultimately, worse health outcomes. The Affordable Care Act (ACA) coverage expansions, including the Medicaid expansion to low-income adults, provide an opportunity to reduce disparities in coverage, which research suggests may contribute to reductions in disparities access to care and health outcomes.
This issue brief builds on a previous literature review that broadly investigated the effects of Medicaid expansion by examining how the expansion has affected racial disparities in health coverage, access to care, health outcomes, and economic outcomes. It is based on a review of 65 studies published beginning in January 2014 (when the coverage provisions of the ACA went into effect) through July 2020. This brief groups outcomes into four broad categories: coverage; access to and use of care; health outcomes and quality of care; and economic measures. Key findings include (Figure 1):
- Most of the 29 studies that examined how Medicaid expansion has affected disparities in health coverage found it helped narrow but did not eliminate racial disparities in health coverage.
- The 24 studies that examined how Medicaid expansion affected access to and use of care generally found expansion was associated with improvements in these measures for some groups but more limited evidence that it reduced racial disparities that existed prior to expansion.
- Some studies find that Medicaid expansion was associated with narrowed disparities in health outcomes for Black and Hispanic individuals, particularly for measures of maternal and infant health.
- The limited number of studies that considered effects of expansion on disparities in economic measures had mixed results but suggested some narrowing of differences in the payer mix for provider reimbursement for health care services (the proportion of uninsured patients vs. Medicaid patients) by patient race/ethnicity and for measures of individual economic well-being.
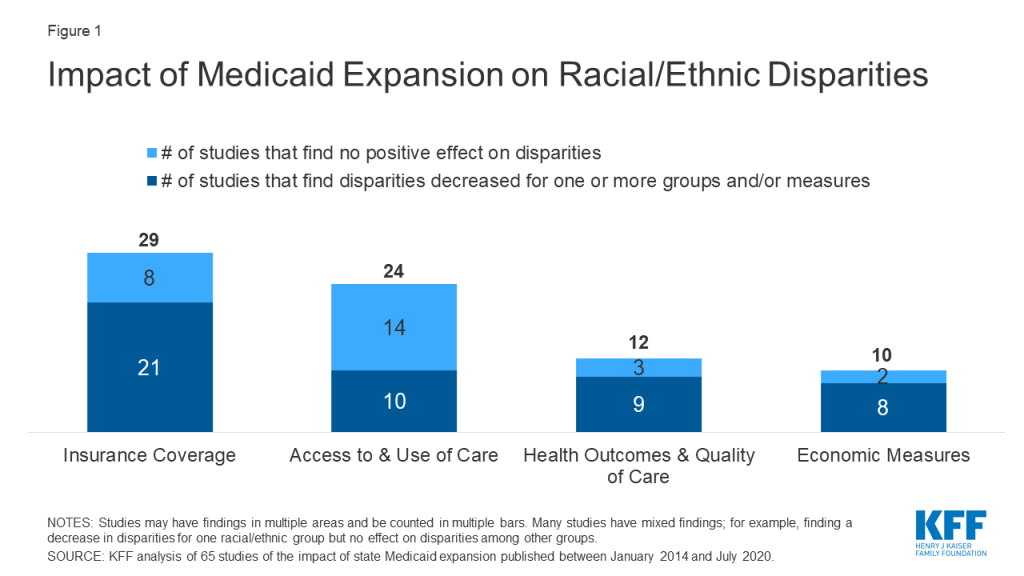
Together these findings illustrate that Medicaid expansion has contributed to reductions in longstanding racial disparities in health coverage. They further suggest that, while increased coverage can help improve access to care and contribute to improvements in health, coverage alone is not enough to eliminate disparities in these measures. This finding reflects that a broad range of social and economic factors beyond health coverage influence and drive health. As such, the findings point to the importance of ongoing efforts to address health disparities considering a broad array of factors within and outside the heath sector, including historic and ongoing racism and discrimination.
Issue Brief
Introduction
This issue brief builds on a previous literature review that broadly investigated the effects of Medicaid expansion by examining how the expansion has affected racial disparities in health coverage, access to care, health outcomes, and economic outcomes. It is based on KFF’s review of 65 studies which examined the impacts of Medicaid expansion by race/ethnicity and were published beginning in January 2014 (when the coverage provisions of the ACA went into effect) through July 2020.1 This brief groups findings into four broad categories: coverage; access to and use of care; health outcomes and quality of care; and economic measures. (Appendix A provides a list of citations for each of the included studies, grouped by the four categories of findings.) Across categories, most research focused on disparities for Black and Hispanic individuals, leaving significant gaps in research to understand impacts for other groups of color.
This review only discusses findings related to changes in racial/ethnic disparities associated with Medicaid expansion. An additional body of work has examined effects of the ACA broadly and suggests significant decreases in disparities following the ACA, but did not examine effects of the Medicaid expansion specifically or differential effects by state Medicaid expansion status. While these studies are not included in this brief, expansion may have played a significant role in the effects found in these studies. (See Methods for more details.)
Key Findings: Effects of Medicaid Expansion
Disparities in Health Coverage
Across the 29 studies that examined how Medicaid expansion has affected disparities in health coverage, 21 found that Medicaid expansion helped narrow but did not eliminate racial/ethnic disparities in health coverage. Studies varied in the groups they examined and the metrics they included to assess coverage. Some of these studies had mixed results; for example, finding disparities narrowed for one racial/ethnic group but that expansion had no effect on or widened disparities for another group. Similarly, findings sometimes varied by measure; for example, some studies found disparities in uninsured rates decreased but those in Medicaid coverage did not, or vice versa. The few studies that did not find expansion had any positive effect on coverage disparities (including a few that found increased disparities) generally considered effects for a targeted population or only used data from the first year of expansion.2 ,3 ,4 ,5 ,6 ,7 ,8 ,9 ,10 ,11 ,12 ,13 ,14 ,15 ,16 ,17 ,18 ,19 ,20 ,21 ,22
Most studies examined changes in coverage disparities for Black and Hispanic individuals but did not provide findings for other groups of color. There was slightly stronger and more consistent evidence of narrowed coverage disparities for Black individuals compared to Hispanic individuals. A smaller number of studies considered how expansion affected coverage disparities for other groups of color, and findings for these groups were mixed.23 ,24 ,25 ,26 A few studies further found variation in how Medicaid expansion affected coverage disparities by country of origin, language, and gender.27 ,28 ,29
Several studies found decreased racial/ethnic coverage disparities among cancer patients and survivors. Specifically, studies suggest that expansion was associated with decreased coverage disparities among Black and Hispanic patients with newly diagnosed cancer; patients with lung, breast, or prostate cancer; patients with head and neck cancer; and women with endometrial cancer.30 ,31 ,32 ,33 ,34 ,35 Study authors explain that racial/ethnic disparities in cancer care and outcomes are longstanding and may be mitigated by increases in insurance coverage.
Disparities in Access to and Use of Care
Most of the 24 studies that examined how Medicaid expansion affected access to and use of care found that it was generally associated with improvements in these measures for some groups but more limited evidence that it reduced disparities that existed prior to the expansion. Ten studies found that Medicaid expansion was associated with narrowed disparities in at least one measure of access for at least one group of color. Within these studies, findings often varied by racial/ethnic group and measure; for example, finding reductions in disparities for some groups and in some measures but not others. The remaining studies did not find expansion reduced access disparities. Two studies found disparities widened for one more or more measures due to larger improvements among White individuals compared to people of color.36 ,37 Most studies considered disparities for Black and Hispanic individuals; few considered effects for other groups.38 ,39 ,40 ,41 ,42 ,43 ,44 ,45 ,46 ,47 ,48 ,49 ,50 ,51 ,52 ,53 ,54 ,55 ,56 ,57 ,58 ,59 Studies focused on several types of measures:
- Access to primary care: While most studies found overall improvements in the share of people having a usual source of care, a personal doctor, and a recent doctor’s visit, they generally did not find expansion was associated with narrowed racial disparities in these measures or had mixed findings across groups, with improvements for one group but not another.60 ,61 ,62 ,63 ,64 ,65
- Affordability of care: Studies generally found improvements in affordability of care across groups, but mixed findings regarding effects on disparities. Several studies found that expansion decreased the gap between Black and White individuals in ability to afford care, but studies generally did not find a narrowing of disparities in affordability between Hispanic and White individuals.66 ,67 ,68 ,69 ,70 ,71 ,72 ,73
- Receipt of preventive care: In contrast to narrowed disparities in coverage among cancer patients associated with expansion, studies did not find expansion was associated with reduced disparities in cancer screening rates, cancer stage at diagnosis, and utilization of cancer surgery.74 ,75 ,76 ,77 One study also found that expansion did not affect disparities in receipt of the flu shot, while other studies found it was associated with narrowed disparities in HIV testing rates and in perforated appendix admission rates (which provide insight into the extent to which patients are able to obtain care earlier to prevent perforation).78 ,79 ,80
- Utilization of health care services: Most studies that consider utilization of services such as surgery for specific conditions find no effect of expansion on disparities.81 ,82 ,83 ,84 ,85 ,86 ,87 ,88 In contrast, a few studies found decreased disparities for at least one racial group in utilization of other specific services, including heart transplant listing rates, high-risk cancer surgery, and receipt of naltrexone or counseling without medication to address opioid use disorder (although this final study also suggested that White adults were more likely than adults of color to receive buprenorphine for opioid use disorder).89 ,90 ,91
Disparities in Health Outcomes & Quality of Care
Studies suggest that Medicaid expansion narrowed disparities in some health outcomes for Black and Hispanic individuals, particularly related to infant and maternal health. Research in these areas generally did not examine effects for other groups of color. Studies suggest larger improvements for Black and, in some cases, Hispanic individuals as compared to White individuals in rates of infant mortality and other adverse birth outcomes and maternal mortality, helping to narrow but not eliminating disparities in these measures.92 ,93 ,94 ,95 ,96 Other studies also found disparities narrowed for at least one group in measures of self-reported health and one-year mortality among end-stage renal disease patients initiating dialysis, but findings were mixed across groups.97 ,98 ,99 Other research found no effect on survival rates among women with endometrial cancer across racial/ethnic groups.100 No studies found increased disparities in health outcomes, although two studies found increased disparities in certain measures of quality of hospital care.101 ,102
Disparities in Payer Mix and Other Economic Outcomes
The limited number of studies that considered effects of expansion on disparities in economic measures had mixed results but suggested some narrowing of differences in the payer mix for provider reimbursement for health care services (the proportion of uninsured patients vs. Medicaid patients) by patient race/ethnicity and for measures of individual economic well-being. Research found greater increases in Medicaid-insured visits and/or decreases in uninsured visits among people of color compared to White people for a variety of specific conditions, although a few other studies suggested that expansion had no effect on or widened disparities in reimbursement patterns for other conditions.103 ,104 ,105 ,106 ,107 ,108 ,109 ,110 A few studies examined disparities in employment and other measures of individual economic well-being. For example, studies suggested that expansion was associated with gains in employment, student status, and volunteerism that reduced racial disparities.111 ,112 However, findings varied across racial and ethnic groups.113 Overall, research in this area remains limited.
Conclusion
Prior to the ACA, there were significant disparities in health and health care. The ACA Medicaid expansion provided an opportunity to reduce longstanding disparities in health coverage, which may contribute to improvements in and narrowed disparities in access to and use of care and health outcomes. This review of the literature finds that Medicaid expansion has helped to narrow but has not eliminated disparities in coverage. It also shows that Medicaid expansion was associated with improvements in measures of access to care, use of care, health outcomes, and certain economic measures across racial/ethnic groups, but its effects on disparities were often mixed across groups and/or measures. This review further shows that most studies only examined effects for Black and Hispanic individuals, leaving continued gaps in data and research for other groups.
Together these findings illustrate that the Medicaid expansion has contributed to reductions in longstanding racial disparities in health coverage. They further suggest that, while increased coverage can help improve access to care and contribute to improvements in health, coverage alone is not enough to eliminate disparities in these measures. This finding reflects that a broad range of social and economic factors beyond health coverage and health care influence and drive health. As such, the findings point to the importance of ongoing efforts to address health disparities considering a broad array of factors within and outside the heath sector, including historic and ongoing racism and discrimination.
Methods
This literature review includes studies, analyses, and reports published by government, research, and policy organizations using data from 2014 or later. This brief includes studies that examine impacts of the Medicaid expansion by race/ethnicity (even if impacts on racial/ethnic disparities were not the primary focus of the study). It excludes studies on impacts of ACA coverage expansions generally (not specific to Medicaid expansion alone), studies investigating potential effects of expansion in states that have not (or had not, at the time of the study) expanded Medicaid, and reports from advocacy organizations and media sources.
To collect relevant studies, we conducted keyword searches of PubMed and other academic health/social policy search engines as well as websites of government, research, and policy organizations that publish health policy-related research. We also used a snowballing technique of pulling additional studies from reference lists in previously collected studies. While we tried to be as comprehensive as possible in our inclusion of studies and findings that meet our criteria, it is possible that we missed some relevant studies or findings. For each study, we read the final paper/report and summarized the population studied, data and methods used, and findings. In instances of conflicting findings within a study, or if a reviewer had questions about specific findings, multiple reviewers read and classified the study to characterize its findings. In the issue brief text, findings are broken out and reported separately in four broad categories: Medicaid expansion’s impact on coverage disparities; disparities in access to and use of care; disparities in health outcomes and quality of care; and disparities in economic metrics. Studies may be cited in multiple categories or in multiple places within a category. Appendix A provides a list of citations for each of the included studies, grouped by the four categories of findings.
Appendix
Appendix A: Studies by Topic
Coverage
Ankit Agarwal, Aaron Katz, and Ronald Chen, “The Impact of the Affordable Care Act on Disparities in Private and Medicaid Insurance Coverage among Patients Under 65 with Newly Diagnosed Cancer, International Journal of Radiation Oncology, Biology, Physics (May 2019), https://www.redjournal.org/article/S0360-3016(19)30783-7/pdf
Manzilat Akande, Peter Minneci, Katherine Deans, Henry Xiang, Deena Chisolm, and Jennifer Cooper, “Effects Of Medicaid Expansion On Disparities In Trauma Care And Outcomes In Young Adults,” Journal of Surgical Research 228 (August 2018): 42-53, https://www.sciencedirect.com/science/article/pii/S0022480418301562
Kelsey Avery, Kenneth Finegold, and Amelia Whitman, Affordable Care Act Has Led to Historic, Widespread Increase in Health Insurance Coverage (Office of the Assistant Secretary for Planning and Evaluation, September 2016), https://aspe.hhs.gov/sites/default/files/pdf/207946/ACAHistoricIncreaseCoverage.pdf
Archana Babu et al., “The Affordable Care Act: Implications for Underserved Populations with Head & Neck Cancer,” American Journal of Otolaryngology 41, no. 4 (July-August 2020), https://doi.org/10.1016/j.amjoto.2020.102464
David Barrington et. al., “Where You Live Matters: A National Cancer Database Study of Medicaid Expansion and Endometrial Cancer Outcomes,” Gynecologic Oncology Epub ahead of print (June 2020), https://doi.org/10.1016/j.ygyno.2020.05.018
Jesse C. Baumgartner, Sara R. Collins, David C. Radley, and Susan L. Hayes, How the Affordable Care Act Has Narrowed Racial and Ethnic Disparities in Access to Health Care (The Commonwealth Fund, January 2020), https://www.commonwealthfund.org/publications/2020/jan/how-ACA-narrowedracial-ethnic-disparities-access
Thomas Buchmueller, Zachary Levinson, Helen Levy, and Barbara Wolfe, “Effect of the Affordable Care Act on Racial and Ethnic Disparities in Health Insurance Coverage,” American Journal of Public Health (May 2016), http://www.ncbi.nlm.nih.gov/pubmed/27196653
Thomas Buchmueller and Helen Levy, “The ACA’s Impact On Racial And Ethnic Disparities In Health Insurance Coverage And Access To Care,” Health Affairs 39, no. 3 (March 2020): 395-402, https://doi.org/10.1377/hlthaff.2019.01394
Fumiko Chino, Gita Suneja, Haley Moss, S. Yousuf Zafar, Laura Havrilesky, and Junzo Chino, “Healthcare Disparities in Cancer Patients Receiving Radiation: Changes in Insurance Status After Medicaid Expansion Under the Affordable Care Act,” International Journal of Radiation Oncology (December 2017), http://www.sciencedirect.com/science/article/pii/S0360301617341883
Charles Courtemanche, James Marton, Benjamin Ukert, Aaron Yelowitz, and Daniela Zapata, Impacts of the Affordable Care Act on Health Insurance Coverage in Medicaid Expansion and Non-Expansion States (Working Paper No. 22182, The National Bureau of Economic Research, April 2016), http://www.nber.org/papers/w22182
Charles Courtemanche, James Marton, Benjamin Ukert, Aaron Yelowitz, Daniela Zapata, and Ishtiaque Fazlul, “The Three‐Year Impact of the Affordable Care Act on Disparities in Insurance Coverage,” Health Services Research (October 2018), https://onlinelibrary.wiley.com/doi/10.1111/1475-6773.13077
Charles J. Courtemanche et al., The Impact of the ACA on Insurance Coverage Disparities After Four Years (National Bureau of Economic Research, Working Paper No. 26157, August 2019),http://www.nber.org/papers/w26157
Sandra Decker, Brandy Lipton, and Benjamin Sommers, “Medicaid Expansion Coverage Effects Grew in 2015 With Continued Improvements in Coverage Quality,” Health Affairs 36 no. 5 (May 2017): 819-825, http://content.healthaffairs.org/content/36/5/819.full
Alina Denham and Peter Veazie, “Did Medicaid Expansion Matter in States with Generous Medicaid?” The American Journal of Managed Care 25, no. 3 (March 2019): 129-134, https://www.ajmc.com/journals/issue/2019/2019-vol25-n3/did-medicaid-expansion-matter-in-states-with-generous-medicaid
Michael Dworsky and Christine Eibner, The Effect of the 2014 Medicaid Expansion on Insurance Coverage for Newly Eligible Childless Adults (Santa Monica, CA: Rand Corporation, 2016), https://www.rand.org/pubs/research_reports/RR1736.htm
Rene Flores and Robert Vargas, “Medicaid Expansion And Ethnoracial Disparities In Health Insurance Coverage,” Journal of Ethnic and Migration Studies 43, no. 12 (June 2017), https://www.tandfonline.com/doi/full/10.1080/1369183X.2017.1323451?needAccess=true
Anna L. Goldman and Benjamin D. Sommers, “Among Low-Income Adults Enrolled In Medicaid, Churning Decreased After The Affordable Care Act,” Health Affairs 39, no. 1 (January 2020): 85-93, https://doi.org/10.1377/hlthaff.2019.00378
Sergio Gonzales and Benjamin Sommers, “Intra-Ethnic Coverage Disparities among Latinos and the Effects of Health Reform” Health Services Research epub ahead of print (June 2017), http://onlinelibrary.wiley.com/wol1/doi/10.1111/1475-6773.12733/full
Xuesong Han, Robin Yabroff, Elizabeth Ward, Otis Brawley, and Ahmedin Jemal, “Comparison of Insurance Status and Diagnosis Stage Among Patients With Newly Diagnosed Cancer Before vs After Implementation of the Patient Protection and Affordable Care Act,” JAMA Oncology 4, no. 12 (August 2018): 1713-1720, https://jamanetwork.com/journals/jamaoncology/article-abstract/2697226
Xuesong Han et al., “Changes in Noninsurance and Care Unaffordability Among Cancer Survivors Following the Affordable Care Act,” Journal of the National Cancer Institute Epub ahead of print (November 2019), https://doi.org/10.1093/jnci/djz218
Susan Hayes, Pamela Riley, David Radley, and Douglas McCarthy, Reducing Racial and Ethnic Disparities in Access to Care: Has the Affordable Care Act Made a Difference? (The Commonwealth Fund, August 2017), http://www.commonwealthfund.org/publications/issue-briefs/2017/aug/racial-ethnicdisparities-care
John Heintzman, Steffani Bailey, Jennifer DeVoe, Stuart Cowburn, Tanya Kapka, Truc-Vi Duong, and Miguel Marino, “In Low-Income Latino Patients, Post-Affordable Care Act Insurance Disparities May Be Reduced Even More than Broader National Estimates: Evidence from Oregon,” Journal of Racial and Ethnic Health Disparities (April 2016), http://www.ncbi.nlm.nih.gov/pubmed/27105630
Hyunjung Lee and Frank Porell, “The Effect of the Affordable Care Act Medicaid Expansion on Disparities in Access to Care and Health Status,” Medical Care Research and Review epub ahead of print (October 2018), https://journals.sagepub.com/doi/abs/10.1177/1077558718808709?rfr_dat=cr_pub%3Dpubmed&url_ver=Z39.88-2003&rfr_id=ori%3Arid%3Acrossref.org&journalCode=mcrd
Brandy Lipton, Sandra Decker, and Benjamin Sommers, “The Affordable Care Act Appears to Have Narrowed Racial and Ethnic Disparities in Insurance Coverage and Access to Care Among Young Adults” Medical Care Research and Review 76, no.1 (April 2017): 32–55, https://www.ncbi.nlm.nih.gov/pubmed/29148341
Amandeep R. Mahal et al., “Early Impact of the Affordable Care Act and Medicaid Expansion on Racial and Socioeconomic Disparities in Cancer Care,” American Journal of Clinical Oncology Epub ahead of print (January 2020), https://doi.org/10.1097/coc.0000000000000588
Nevada’s Medicaid Population, (Las Vegas, NV: The Guinn Center, September 2019), https://guinncenter.org/wp-content/uploads/2019/09/Guinn-Center-NV-Medicaid-PopulationCharacteristics-2019.pdf
Scott R. Sanders et al., “Infants Without Health Insurance: Racial/Ethnic and Rural/Urban Disparities in Infant Households’ Insurance Coverage,” PLoS One 15, no. 1 (January 2020), https://doi.org/10.1371/journal.pone.0222387
George Wehby and Wei Lyu, “The Impact of the ACA Medicaid Expansions on Health Insurance Coverage through 2015 and Coverage Disparities by Age, Race/Ethnicity, and Gender” Health Services Research epub ahead of print (May 2017), http://onlinelibrary.wiley.com/doi/10.1111/1475-6773.12711/abstract
Dahai Yue, Petra Rasmussen, and Ninez Ponce, “Racial/Ethnic Differential Effects of Medicaid Expansion on Health Care Access,” Health Services Research (February 2018), http://onlinelibrary.wiley.com/doi/10.1111/1475-6773.12834/abstract
Access to and Use of Care (back to top)
David Barrington et. al., “Where You Live Matters: A National Cancer Database Study of Medicaid Expansion and Endometrial Cancer Outcomes,” Gynecologic Oncology Epub ahead of print (June 2020), https://doi.org/10.1016/j.ygyno.2020.05.018
Jesse C. Baumgartner, Sara R. Collins, David C. Radley, and Susan L. Hayes, How the Affordable Care Act Has Narrowed Racial and Ethnic Disparities in Access to Health Care (The Commonwealth Fund, January 2020), https://www.commonwealthfund.org/publications/2020/jan/how-ACA-narrowedracial-ethnic-disparities-access
Khadijah Breathett et al., “The Affordable Care Act Medicaid Expansion Correlated with Increased Heart Transplant Listings in African Americans but Not Hispanics or Caucasians,” JACC: Heart Failure 5 no. 2 (January 2017): 136-147, https://www.ncbi.nlm.nih.gov/pubmed/28109783
Khadijah Breathett et al., “Is the Affordable Care Act Medicaid Expansion Linked to Change in Rate of Ventricular Assist Device Implantation for Blacks and Whites?” Circulation: Heart Failure 13, no. 4 (April 2020), https://doi.org/10.1161/CIRCHEARTFAILURE.119.006544
Thomas Buchmueller and Helen Levy, “The ACA’s Impact On Racial And Ethnic Disparities In Health Insurance Coverage And Access To Care,” Health Affairs 39, no. 3 (March 2020): 395-402, https://doi.org/10.1377/hlthaff.2019.01394
Andrew Crocker et al., “Expansion Coverage And Preferential Utilization Of Cancer Surgery Among Racial And Ethnic Minorities And Low-Income Groups,” Surgery epub ahead of print (June 2019), https://www.surgjournal.com/article/S0039-6060(19)30198-9/fulltext
Adrian Diaz, Daniel Chavarin, Anghela Z. Paredes, and Timothy M. Pawlik, “Utilization of High-Volume Hospitals for High-Risk Cancer Surgery in California Following Medicaid Expansion,” Journal of Gastrointestinal Surgery Epub ahead of print (July 2020), https://link.springer.com/article/10.1007/s11605-020-04747-8
Afshin Ehsan et al., “Utilization of Left Ventricular Assist Devices in Vulnerable Adults Across Medicaid Expansion,” Journal of Surgical Research 243 (November 2019): 503-508, https://doi.org/10.1016/j.jss.2019.05.015
Yunwei Gai and John Marthinsen, “Medicaid Expansion, HIV Testing, and HIV-Related Risk Behaviors in the United States, 2010-2017,” American Journal of Public Health 109, no. 10 (October 2019): 1404- 1412, https://doi.org/10.2105/ajph.2019.305220
Kelsie M. Gould et al., “Bariatric Surgery Among Vulnerable Populations: The Effect of the Affordable Care Act’s Medicaid Expansion,” Surgery 166, no. 5 (November 2019): 820-828, https://doi.org/10.1016/j.surg.2019.05.005
Xuesong Han et al., “Changes in Noninsurance and Care Unaffordability Among Cancer Survivors Following the Affordable Care Act,” Journal of the National Cancer Institute Epub ahead of print (November 2019), https://doi.org/10.1093/jnci/djz218
Susan Hayes, Sara Collins, David Radley, and Douglas McCarthy, What’s at Stake: States’ Progress on Health Coverage and Access to Care, 2013-2016 (The Commonwealth Fund, December 2017), http://www.commonwealthfund.org/publications/issue-briefs/2017/dec/states-progress-health-coverageand-access
Susan Hayes, Pamela Riley, David Radley, and Douglas McCarthy, Reducing Racial and Ethnic Disparities in Access to Care: Has the Affordable Care Act Made a Difference? (The Commonwealth Fund, August 2017), https://www.commonwealthfund.org/publications/issue-briefs/2017/aug/reducing-racial-and-ethnic-disparities-access-care-has
Nathalie Huguet et al., “Cervical And Colorectal Cancer Screening Prevalence Before And After Affordable Care Act Medicaid Expansion,” Preventative Medicine (May 2019), https://doi.org/10.1016/j.ypmed.2019.05.003
Nadia Laniado, Avery R. Brow, Eric Tranby, and Victor M. Badner, “Trends in Non-Traumatic Dental Emergency Department Use in New York and New Jersey: A Look at Medicaid Expansion from Both Sides of the Hudson River,” Journal of Public Health Dentistry Epub ahead of print (October 2019), https://doi.org/10.1111/jphd.12343
Justin Le Blanc, Danielle Heller, Ann Friedrich, Donald Lannin, and Tristen Park, “Association of Medicaid Expansion Under the Affordable Care Act With Breast Cancer Stage at Diagnosis,” JAMA Surgery (July 2020), https://doi.org/10.1001/jamasurg.2020.1495
Brandy Lipton, Sandra Decker, and Benjamin Sommers, “The Affordable Care Act Appears to Have Narrowed Racial and Ethnic Disparities in Insurance Coverage and Access to Care Among Young Adults” Medical Care Research and Review 76, no.1 (April 2017): 32–55, https://www.ncbi.nlm.nih.gov/pubmed/29148341
Miguel Marino et al., “Disparities in Biomarkers for Patients With Diabetes After the Affordable Care Act,” Medical Care 58 (June 2020), https://doi.org/10.1097/mlr.0000000000001257
Hyunjung Lee and Frank Porell, “The Effect of the Affordable Care Act Medicaid Expansion on Disparities in Access to Care and Health Status,” Medical Care Research and Review epub ahead of print (October 2018), https://journals.sagepub.com/doi/abs/10.1177/1077558718808709?rfr_dat=cr_pub%3Dpubmed&url_ver=Z39.88-2003&rfr_id=ori%3Arid%3Acrossref.org&journalCode=mcrd
James McDermott et al., “Affordable Care Act’s Medicaid Expansion and Use of Regionalized Surgery at High-Volume Hospitals,” Journal of the American College of Surgeons 227, no. 5 (November 2018): 507-520.e9, https://doi.org/10.1016/j.jamcollsurg.2018.08.693
Brendan Saloner, Rachel Landis, Bradley Stein, and Colleen Barry, “The Affordable Care Act in the Heart of the Opioid Crisis: Evidence from West Virginia,” Health Affairs 38, no. 4 (April 2019), https://www.healthaffairs.org/doi/full/10.1377/hlthaff.2018.05049
Dahai Yue, Petra Rasmussen, and Ninez Ponce, “Racial/Ethnic Differential Effects of Medicaid Expansion on Health Care Access,” Health Services Research (February 2018), http://onlinelibrary.wiley.com/doi/10.1111/1475-6773.12834/abstract
Yasmin Zerhouni et al., “Effect of Medicaid Expansion on Colorectal Cancer Screening Rates,” Diseases of the Colon & Rectum 62, no. 1 (January 2019): 97-103, https://journals.lww.com/dcrjournal/Abstract/2019/01000/Effect_of_Medicaid_Expansion_on_Colorectal_Cancer.16.aspx
Cheryl Zogg et al., “Impact of Affordable Care Act Insurance Expansion on Pre-Hospital Access to Care: Changes in Adult Perforated Appendix Admission Rates after Medicaid Expansion and the Dependent Coverage Provision,” Journal of the American College of Surgeons 228, no. 1 (January 2019): 29-43, https://doi.org/10.1016/j.jamcollsurg.2018.09.022
Health Outcomes and Quality of Care (back to top)
Manzilat Akande, Peter Minneci, Katherine Deans, Henry Xiang, Deena Chisolm, and Jennifer Cooper, “Effects Of Medicaid Expansion On Disparities In Trauma Care And Outcomes In Young Adults,” Journal of Surgical Research 228 (August 2018): 42-53, https://www.sciencedirect.com/science/article/pii/S0022480418301562
David Barrington et. al., “Where You Live Matters: A National Cancer Database Study of Medicaid Expansion and Endometrial Cancer Outcomes,” Gynecologic Oncology Epub ahead of print (June 2020), https://doi.org/10.1016/j.ygyno.2020.05.018
Chintan Bhatt and Consuelo Beck-Sague, “Medicaid Expansion and Infant Mortality in the United States,” American Journal of Public Health 108, no. 4 (April 2018): 565-567, https://ajph.aphapublications.org/doi/full/10.2105/AJPH.2017.304218
Clare Brown, Jennifer Moore, Felix Holly, Kathryn Stewart, and Mick Tilford, “County-level Variation in Low Birthweight and Preterm Birth: An Evaluation of State Medicaid Expansion Under the Affordable Care Act,” Medical Care 58, no. 6 (June 2020): 497-503, https://doi.org/10.1097/mlr.0000000000001313
Clare Brown et al., “Association of State Medicaid Expansion Status With Low Birth Weight and Preterm Birth” Journal of the American Medical Association 321, no. 16 (April 2019), https://jamanetwork.com/journals/jama/fullarticle/2731179
Erica Eliason, “Adoption of Medicaid Expansion Is Associated with Lower Maternal Mortality,” Women’s Health Issues 30, no. 3 (May-June 2020): 147-152, https://doi.org/10.1016/j.whi.2020.01.005
Hyunjung Lee and Frank Porell, “The Effect of the Affordable Care Act Medicaid Expansion on Disparities in Access to Care and Health Status,” Medical Care Research and Review epub ahead of print (October 2018), https://journals.sagepub.com/doi/abs/10.1177/1077558718808709?rfr_dat=cr_pub%3Dpubmed&url_ver=Z39.88-2003&rfr_id=ori%3Arid%3Acrossref.org&journalCode=mcrd
Miguel Marino et al., “Disparities in Biomarkers for Patients With Diabetes After the Affordable Care Act,” Medical Care 58 (June 2020), https://doi.org/10.1097/mlr.0000000000001257
Minal R. Patel et al., “Examination of Changes in Health Status Among Michigan Medicaid Expansion Enrollees From 2016 to 2017,” JAMA Network Open 3, no. 7 (July 2020), https://doi.org/10.1001/jamanetworkopen.2020.8776
Shailender Swaminathan, Benjamin Sommers, Rebecca Thorsness, Rajnish Mehrotra, Yoojin Lee, and Amal Trivedi, “Association of Medicaid Expansion With 1-Year Mortality Among Patients With End Stage Renal Disease,” Journal of the American Medical Association (JAMA) 320, no. 21 (December 2018): 2242 2250, https://jamanetwork.com/journals/jama/fullarticle/2710505?guestAccessKey=ea3a8641-320b-4afd-b96edc59fbd90b20&utm_source=TrendMD&utm_medium=cpc&utm_campaign=J_Am_Med_TrendMD_1&utm_content=olf&utm_term=102518
Alexandra Wiggins, Ibraheem M. Karaye, Jennifer A. Horney, “Medicaid Expansion and Infant Mortality, Revisited: A Difference-In-Differences Analysis,” Health Services Research 55, no. 3 (March 2020): 393-398, https://doi.org/10.1111/1475-6773.13286
Cheryl Zogg et al., “Association of Medicaid Expansion With Access to Rehabilitative Care in Adult Trauma Patients,” JAMA Surgery epub ahead of print (January 2019), https://jamanetwork.com/journals/jamasurgery/articleabstract/2719270?utm_campaign=articlePDF&utm_medium=articlePDFlink&utm_source=articlePDF&utm_content=jamasurg.2018.5177
Economic Measures (back to top)
Heather Angier et al., “Racial/Ethnic Disparities in Health Insurance and Differences in Visit Type for a Population of Patients with Diabetes after Medicaid Expansion,” Journal of Health Care for the Poor and Underserved 30, no.1, (March 2019): 116–130, https://www.ncbi.nlm.nih.gov/pmc/articles/PMC6429963/
Heather Angier et al., “Uninsured Primary Care Visit Disparities under the Affordable Care Act,” Annals of Family Medicine, 15 no. 5 (September 2017): 434-442, http://www.annfammed.org/content/15/5/434.full.pdf+html
Kevin Callison and Paul Sicilian, “Economic Freedom and the Affordable Care Act: Medicaid Expansions and Labor Mobility by Race and Ethnicity,” Public Finance Review 46, no. 2 (March 2018), https://journals.sagepub.com/doi/abs/10.1177/1091142116668254
Adrian Diaz, Daniel Chavarin, Anghela Z. Paredes, and Timothy M. Pawlik, “Utilization of High-Volume Hospitals for High-Risk Cancer Surgery in California Following Medicaid Expansion,” Journal of Gastrointestinal Surgery Epub ahead of print (July 2020), https://link.springer.com/article/10.1007/s11605-020-04747-8
Meera Harhay et al., “Association between Medicaid Expansion under the Affordable Care Act and Preemptive Listings for Kidney Transplantation,” Clinical Journal of the American Society of Nephrology 13 (July 2018), https://cjasn.asnjournals.org/content/13/7/1069
J.W. Awori Hayanga et al., “Lung Transplantation and Affordable Care Act Medicaid Expansion in the Era of Lung Allocation Score” Transplant International Epub ahead of print (February 2019), https://onlinelibrary.wiley.com/doi/pdf/10.1111/tri.13420
Justin Le Blanc, Danielle Heller, Ann Friedrich, Donald Lannin, and Tristen Park, “Association of Medicaid Expansion Under the Affordable Care Act With Breast Cancer Stage at Diagnosis,” JAMA Surgery (July 2020), https://doi.org/10.1001/jamasurg.2020.1495
Heeju Sohn and Stefan Timmermans, “Social Effects of Health Care Reform: Medicaid Expansion under the Affordable Care Act and Changes in Volunteering,” Socius: Socialogical Research for a Dynamic World 3 (March 2017): 1-12, http://journals.sagepub.com/doi/full/10.1177/2378023117700903
Renuka Tipirneni et al., “Association of Medicaid Expansion With Enrollee Employment and Student Status in Michigan,” JAMA Network Open 3, no. 1 (January 2020), https://doi.org/10.1001/jamanetworkopen.2019.20316
Cheryl Zogg et al., “Association of Medicaid Expansion With Access to Rehabilitative Care in Adult Trauma Patients,” JAMA Surgery epub ahead of print (January 2019), https://jamanetwork.com/journals/jamasurgery/articleabstract/2719270?utm_campaign=articlePDF&utm_medium=articlePDFlink&utm_source=articlePDF&utm_content=jamasurg.2018.5177
Cheryl Zogg et al., “Impact of Affordable Care Act Insurance Expansion on Pre-Hospital Access to Care: Changes in Adult Perforated Appendix Admission Rates after Medicaid Expansion and the Dependent Coverage Provision,” Journal of the American College of Surgeons 228, no. 1 (January 2019): 29-43, https://www.journalacs.org/article/S1072-7515(18)32078-7/fulltext
Endnotes
- Studies measured effects on racial and ethnic disparities in several ways, including assessing whether modeled effects of Medicaid expansion were larger for people of color compared to White people, comparing trends in expansion vs. non-expansion states by race and ethnicity, and examining trends within an expansion state by race and ethnicity. ↩︎
- Ankit Agarwal, Aaron Katz, and Ronald Chen, “The Impact of the Affordable Care Act on Disparities in Private and Medicaid Insurance Coverage among Patients Under 65 with Newly Diagnosed Cancer, International Journal of Radiation Oncology, Biology, Physics (May 2019), https://www.redjournal.org/article/S0360-3016(19)30783-7/pdf ↩︎
- John Heintzman, Steffani Bailey, Jennifer DeVoe, Stuart Cowburn, Tanya Kapka, Truc-Vi Duong, and Miguel Marino, “In Low-Income Latino Patients, Post-Affordable Care Act Insurance Disparities May Be Reduced Even More than Broader National Estimates: Evidence from Oregon,” Journal of Racial and Ethnic Health Disparities (April 2016), http://www.ncbi.nlm.nih.gov/pubmed/27105630 ↩︎
- Brandy Lipton, Sandra Decker, and Benjamin Sommers, “The Affordable Care Act Appears to Have Narrowed Racial and Ethnic Disparities in Insurance Coverage and Access to Care Among Young Adults” Medical Care Research and Review 76, no.1 (April 2017): 32–55, https://www.ncbi.nlm.nih.gov/pubmed/29148341 ↩︎
- George Wehby and Wei Lyu, “The Impact of the ACA Medicaid Expansions on Health Insurance Coverage through 2015 and Coverage Disparities by Age, Race/Ethnicity, and Gender” Health Services Research epub ahead of print (May 2017), http://onlinelibrary.wiley.com/doi/10.1111/1475-6773.12711/abstract ↩︎
- Archana Babu et al., “The Affordable Care Act: Implications for Underserved Populations with Head & Neck Cancer,” American Journal of Otolaryngology 41, no. 4 (July-August 2020), https://doi.org/10.1016/j.amjoto.2020.102464 ↩︎
- Thomas Buchmueller, Zachary Levinson, Helen Levy, and Barbara Wolfe, “Effect of the Affordable Care Act on Racial and Ethnic Disparities in Health Insurance Coverage,” American Journal of Public Health (May 2016), http://www.ncbi.nlm.nih.gov/pubmed/27196653 ↩︎
- Fumiko Chino, Gita Suneja, Haley Moss, S. Yousuf Zafar, Laura Havrilesky, and Junzo Chino, “Healthcare Disparities in Cancer Patients Receiving Radiation: Changes in Insurance Status After Medicaid Expansion Under the Affordable Care Act,” International Journal of Radiation Oncology (December 2017), http://www.sciencedirect.com/science/article/pii/S0360301617341883 ↩︎
- Charles Courtemanche, James Marton, Benjamin Ukert, Aaron Yelowitz, and Daniela Zapata, Impacts of the Affordable Care Act on Health Insurance Coverage in Medicaid Expansion and Non-Expansion States (Working Paper No. 22182, The National Bureau of Economic Research, April 2016), http://www.nber.org/papers/w22182 ↩︎
- Charles Courtemanche, James Marton, Benjamin Ukert, Aaron Yelowitz, Daniela Zapata, and Ishtiaque Fazlul, “The Three‐Year Impact of the Affordable Care Act on Disparities in Insurance Coverage,” Health Services Research (October 2018), https://onlinelibrary.wiley.com/doi/10.1111/1475-6773.13077 ↩︎
- Sergio Gonzales and Benjamin Sommers, “Intra-Ethnic Coverage Disparities among Latinos and the Effects of Health Reform” Health Services Research epub ahead of print (June 2017), http://onlinelibrary.wiley.com/wol1/doi/10.1111/1475-6773.12733/full ↩︎
- Xuesong Han, Robin Yabroff, Elizabeth Ward, Otis Brawley, and Ahmedin Jemal, “Comparison of Insurance Status and Diagnosis Stage Among Patients With Newly Diagnosed Cancer Before vs After Implementation of the Patient Protection and Affordable Care Act,” JAMA Oncology 4, no. 12 (August 2018): 1713-1720, https://jamanetwork.com/journals/jamaoncology/article-abstract/2697226 ↩︎
- Susan Hayes, Pamela Riley, David Radley, and Douglas McCarthy, Reducing Racial and Ethnic Disparities in Access to Care: Has the Affordable Care Act Made a Difference? (The Commonwealth Fund, August 2017), https://www.commonwealthfund.org/publications/issue-briefs/2017/aug/reducing-racial-and-ethnic-disparities-access-care-has ↩︎
- John Heintzman, Steffani Bailey, Jennifer DeVoe, Stuart Cowburn, Tanya Kapka, Truc-Vi Duong, and Miguel Marino, “In Low-Income Latino Patients, Post-Affordable Care Act Insurance Disparities May Be Reduced Even More than Broader National Estimates: Evidence from Oregon,” Journal of Racial and Ethnic Health Disparities (April 2016), http://www.ncbi.nlm.nih.gov/pubmed/27105630 ↩︎
- Manzilat Akande, Peter Minneci, Katherine Deans, Henry Xiang, Deena Chisolm, and Jennifer Cooper, “Effects Of Medicaid Expansion On Disparities In Trauma Care And Outcomes In Young Adults,” Journal of Surgical Research 228 (August 2018): 42-53, https://www.sciencedirect.com/science/article/pii/S0022480418301562 ↩︎
- Kelsey Avery, Kenneth Finegold, and Amelia Whitman, Affordable Care Act Has Led to Historic, Widespread Increase in Health Insurance Coverage (Office of the Assistant Secretary for Planning and Evaluation, September 2016), https://aspe.hhs.gov/sites/default/files/pdf/207946/ACAHistoricIncreaseCoverage.pdf ↩︎
- Charles J. Courtemanche et al., The Impact of the ACA on Insurance Coverage Disparities After Four Years (National Bureau of Economic Research, Working Paper No. 26157, August 2019), http://www.nber.org/papers/w26157 ↩︎
- Jesse C. Baumgartner, Sara R. Collins, David C. Radley, and Susan L. Hayes, How the Affordable Care Act Has Narrowed Racial and Ethnic Disparities in Access to Health Care (The Commonwealth Fund, January 2020), https://www.commonwealthfund.org/publications/2020/jan/how-ACA-narrowedracial-ethnic-disparities-access ↩︎
- Scott R. Sanders et al., “Infants Without Health Insurance: Racial/Ethnic and Rural/Urban Disparities in Infant Households’ Insurance Coverage,” PLoS One 15, no. 1 (January 2020), https://doi.org/10.1371/journal.pone.0222387 ↩︎
- Amandeep R. Mahal et al., “Early Impact of the Affordable Care Act and Medicaid Expansion on Racial and Socioeconomic Disparities in Cancer Care,” American Journal of Clinical Oncology Epub ahead of print (January 2020), https://doi.org/10.1097/coc.0000000000000588 ↩︎
- David Barrington et. al., “Where You Live Matters: A National Cancer Database Study of Medicaid Expansion and Endometrial Cancer Outcomes,” Gynecologic Oncology Epub ahead of print (June 2020), https://doi.org/10.1016/j.ygyno.2020.05.018 ↩︎
- Thomas Buchmueller and Helen Levy, “The ACA’s Impact On Racial And Ethnic Disparities In Health Insurance Coverage And Access To Care,” Health Affairs 39, no. 3 (March 2020): 395-402, https://doi.org/10.1377/hlthaff.2019.01394 ↩︎
- Kelsey Avery, Kenneth Finegold, and Amelia Whitman, Affordable Care Act Has Led to Historic, Widespread Increase in Health Insurance Coverage (Office of the Assistant Secretary for Planning and Evaluation, September 2016), https://aspe.hhs.gov/sites/default/files/pdf/207946/ACAHistoricIncreaseCoverage.pdf ↩︎
- Ankit Agarwal, Aaron Katz, and Ronald Chen, “The Impact of the Affordable Care Act on Disparities in Private and Medicaid Insurance Coverage among Patients Under 65 with Newly Diagnosed Cancer, International Journal of Radiation Oncology, Biology, Physics (May 2019), https://www.redjournal.org/article/S0360-3016(19)30783-7/pdf ↩︎
- Michael Dworsky and Christine Eibner, The Effect of the 2014 Medicaid Expansion on Insurance Coverage for Newly Eligible Childless Adults (Santa Monica, CA: Rand Corporation, 2016), https://www.rand.org/pubs/research_reports/RR1736.htm ↩︎
- Nevada’s Medicaid Population, (Las Vegas, NV: The Guinn Center, September 2019), https://guinncenter.org/wp-content/uploads/2019/09/Guinn-Center-NV-Medicaid-PopulationCharacteristics-2019.pdf ↩︎
- Sergio Gonzales and Benjamin Sommers, “Intra-Ethnic Coverage Disparities among Latinos and the Effects of Health Reform” Health Services Research epub ahead of print (June 2017), http://onlinelibrary.wiley.com/wol1/doi/10.1111/1475-6773.12733/full ↩︎
- John Heintzman, Steffani Bailey, Jennifer DeVoe, Stuart Cowburn, Tanya Kapka, Truc-Vi Duong, and Miguel Marino, “In Low-Income Latino Patients, Post-Affordable Care Act Insurance Disparities May Be Reduced Even More than Broader National Estimates: Evidence from Oregon,” Journal of Racial and Ethnic Health Disparities (April 2016), http://www.ncbi.nlm.nih.gov/pubmed/27105630 ↩︎
- George Wehby and Wei Lyu, “The Impact of the ACA Medicaid Expansions on Health Insurance Coverage through 2015 and Coverage Disparities by Age, Race/Ethnicity, and Gender” Health Services Research epub ahead of print (May 2017), http://onlinelibrary.wiley.com/doi/10.1111/1475-6773.12711/abstract ↩︎
- Ankit Agarwal, Aaron Katz, and Ronald Chen, “The Impact of the Affordable Care Act on Disparities in Private and Medicaid Insurance Coverage among Patients Under 65 with Newly Diagnosed Cancer, International Journal of Radiation Oncology, Biology, Physics (May 2019), https://www.redjournal.org/article/S0360-3016(19)30783-7/pdf ↩︎
- Fumiko Chino, Gita Suneja, Haley Moss, S. Yousuf Zafar, Laura Havrilesky, and Junzo Chino, “Healthcare Disparities in Cancer Patients Receiving Radiation: Changes in Insurance Status After Medicaid Expansion Under the Affordable Care Act,” International Journal of Radiation Oncology (December 2017), http://www.sciencedirect.com/science/article/pii/S0360301617341883 ↩︎
- Xuesong Han, Robin Yabroff, Elizabeth Ward, Otis Brawley, and Ahmedin Jemal, “Comparison of Insurance Status and Diagnosis Stage Among Patients With Newly Diagnosed Cancer Before vs After Implementation of the Patient Protection and Affordable Care Act,” JAMA Oncology 4, no. 12 (August 2018): 1713-1720, https://jamanetwork.com/journals/jamaoncology/article-abstract/2697226 ↩︎
- Amandeep R. Mahal et al., “Early Impact of the Affordable Care Act and Medicaid Expansion on Racial and Socioeconomic Disparities in Cancer Care,” American Journal of Clinical Oncology Epub ahead of print (January 2020), https://doi.org/10.1097/coc.0000000000000588 ↩︎
- Archana Babu et al., “The Affordable Care Act: Implications for Underserved Populations with Head & Neck Cancer,” American Journal of Otolaryngology 41, no. 4 (July-August 2020), https://doi.org/10.1016/j.amjoto.2020.102464 ↩︎
- David Barrington et. al., “Where You Live Matters: A National Cancer Database Study of Medicaid Expansion and Endometrial Cancer Outcomes,” Gynecologic Oncology Epub ahead of print (June 2020), https://doi.org/10.1016/j.ygyno.2020.05.018 ↩︎
- Hyunjung Lee and Frank Porell, “The Effect of the Affordable Care Act Medicaid Expansion on Disparities in Access to Care and Health Status,” Medical Care Research and Review epub ahead of print (October 2018), https://journals.sagepub.com/doi/abs/10.1177/1077558718808709?rfr_dat=cr_pub%3Dpubmed&url_ver=Z39.88-2003&rfr_id=ori%3Arid%3Acrossref.org&journalCode=mcrd ↩︎
- Brendan Saloner, Rachel Landis, Bradley Stein, and Colleen Barry, “The Affordable Care Act in the Heart of the Opioid Crisis: Evidence from West Virginia,” Health Affairs 38, no. 4 (April 2019), https://www.healthaffairs.org/doi/full/10.1377/hlthaff.2018.05049 ↩︎
- Susan Hayes, Pamela Riley, David Radley, and Douglas McCarthy, Reducing Racial and Ethnic Disparities in Access to Care: Has the Affordable Care Act Made a Difference? (The Commonwealth Fund, August 2017), http://www.commonwealthfund.org/publications/issue-briefs/2017/aug/racial-ethnicdisparities-care ↩︎
- Brandy Lipton, Sandra Decker, and Benjamin Sommers, “The Affordable Care Act Appears to Have Narrowed Racial and Ethnic Disparities in Insurance Coverage and Access to Care Among Young Adults” Medical Care Research and Review 76, no.1 (April 2017): 32–55, https://www.ncbi.nlm.nih.gov/pubmed/29148341 ↩︎
- Dahai Yue, Petra Rasmussen, and Ninez Ponce, “Racial/Ethnic Differential Effects of Medicaid Expansion on Health Care Access,” Health Services Research (February 2018), http://onlinelibrary.wiley.com/doi/10.1111/1475-6773.12834/abstract ↩︎
- Andrew Crocker et al., “Expansion Coverage And Preferential Utilization Of Cancer Surgery Among Racial And Ethnic Minorities And Low-Income Groups,” Surgery epub ahead of print (June 2019), https://www.surgjournal.com/article/S0039-6060(19)30198-9/fulltext ↩︎
- Nathalie Huguet et al., “Cervical And Colorectal Cancer Screening Prevalence Before And After Affordable Care Act Medicaid Expansion,” Preventative Medicine (May 2019), https://doi.org/10.1016/j.ypmed.2019.05.003 ↩︎
- James McDermott et al., “Affordable Care Act’s Medicaid Expansion and Use of Regionalized Surgery at High-Volume Hospitals,” Journal of the American College of Surgeons 227, no. 5 (November 2018): 507-520.e9, https://www.journalacs.org/article/S1072-7515(18)31993-8/abstrac ↩︎
- Afshin Ehsan et al., “Utilization of Left Ventricular Assist Devices in Vulnerable Adults Across Medicaid Expansion,” Journal of Surgical Research 243 (November 2019): 503-508, https://doi.org/10.1016/j.jss.2019.05.015 ↩︎
- Kelsie M. Gould et al., “Bariatric Surgery Among Vulnerable Populations: The Effect of the Affordable Care Act’s Medicaid Expansion,” Surgery 166, no. 5 (November 2019): 820-828, https://doi.org/10.1016/j.surg.2019.05.005 ↩︎
- Nadia Laniado, Avery R. Brow, Eric Tranby, and Victor M. Badner, “Trends in Non-Traumatic Dental Emergency Department Use in New York and New Jersey: A Look at Medicaid Expansion from Both Sides of the Hudson River,” Journal of Public Health Dentistry Epub ahead of print (October 2019), https://doi.org/10.1111/jphd.12343 ↩︎
- Khadijah Breathett et al., “The Affordable Care Act Medicaid Expansion Correlated with Increased Heart Transplant Listings in African Americans but Not Hispanics or Caucasians,” JACC: Heart Failure 5 no. 2 (January 2017): 136-147, https://www.ncbi.nlm.nih.gov/pubmed/28109783 ↩︎
- Yasmin Zerhouni et al., “Effect of Medicaid Expansion on Colorectal Cancer Screening Rates,” Diseases of the Colon & Rectum 62, no. 1 (January 2019): 97-103, https://journals.lww.com/dcrjournal/Abstract/2019/01000/Effect_of_Medicaid_Expansion _on_Colorectal_Cancer.16.aspx ↩︎
- David Barrington et. al., “Where You Live Matters: A National Cancer Database Study of Medicaid Expansion and Endometrial Cancer Outcomes,” Gynecologic Oncology Epub ahead of print (June 2020), https://doi.org/10.1016/j.ygyno.2020.05.018 ↩︎
- Khadijah Breathett et al., “Is the Affordable Care Act Medicaid Expansion Linked to Change in Rate of Ventricular Assist Device Implantation for Blacks and Whites?” Circulation: Heart Failure 13, no. 4 (April 2020), https://doi.org/10.1161/CIRCHEARTFAILURE.119.006544 ↩︎
- Thomas Buchmueller and Helen Levy, “The ACA’s Impact On Racial And Ethnic Disparities In Health Insurance Coverage And Access To Care,” Health Affairs 39, no. 3 (March 2020): 395-402, https://doi.org/10.1377/hlthaff.2019.01394 ↩︎
- Justin Le Blanc, Danielle Heller, Ann Friedrich, Donald Lannin, and Tristen Park, “Association of Medicaid Expansion Under the Affordable Care Act With Breast Cancer Stage at Diagnosis,” JAMA Surgery (July 2020), https://doi.org/10.1001/jamasurg.2020.1495 ↩︎
- Miguel Marino et al., “Disparities in Biomarkers for Patients With Diabetes After the Affordable Care Act,” Medical Care 58 (June 2020), https://doi.org/10.1097/mlr.0000000000001257 ↩︎
- Brendan Saloner, Rachel Landis, Bradley Stein, and Colleen Barry, “The Affordable Care Act in the Heart of the Opioid Crisis: Evidence from West Virginia,” Health Affairs 38, no. 4 (April 2019), https://www.healthaffairs.org/doi/full/10.1377/hlthaff.2018.05049 ↩︎
- Susan Hayes, Pamela Riley, David Radley, and Douglas McCarthy, Reducing Racial and Ethnic Disparities in Access to Care: Has the Affordable Care Act Made a Difference? (The Commonwealth Fund, August 2017), http://www.commonwealthfund.org/publications/issue-briefs/2017/aug/racial-ethnicdisparities-care ↩︎
- Dahai Yue, Petra Rasmussen, and Ninez Ponce, “Racial/Ethnic Differential Effects of Medicaid Expansion on Health Care Access,” Health Services Research (February 2018), http://onlinelibrary.wiley.com/doi/10.1111/1475-6773.12834/abstract ↩︎
- Xuesong Han et al., “Changes in Noninsurance and Care Unaffordability Among Cancer Survivors Following the Affordable Care Act,” Journal of the National Cancer Institute Epub ahead of print (November 2019), https://doi.org/10.1093/jnci/djz218 ↩︎
- Jesse C. Baumgartner, Sara R. Collins, David C. Radley, and Susan L. Hayes, How the Affordable Care Act Has Narrowed Racial and Ethnic Disparities in Access to Health Care (The Commonwealth Fund, January 2020), https://www.commonwealthfund.org/publications/2020/jan/how-ACA-narrowedracial-ethnic-disparities-access ↩︎
- Thomas Buchmueller and Helen Levy, “The ACA’s Impact On Racial And Ethnic Disparities In Health Insurance Coverage And Access To Care,” Health Affairs 39, no. 3 (March 2020): 395-402, https://doi.org/10.1377/hlthaff.2019.01394 ↩︎
- Susan Hayes, Pamela Riley, David Radley, and Douglas McCarthy, Reducing Racial and Ethnic Disparities in Access to Care: Has the Affordable Care Act Made a Difference? (The Commonwealth Fund, August 2017), https://www.commonwealthfund.org/publications/issue-briefs/2017/aug/reducing-racial-and-ethnic-disparities-access-care-has ↩︎
- Hyunjung Lee and Frank Porell, “The Effect of the Affordable Care Act Medicaid Expansion on Disparities in Access to Care and Health Status,” Medical Care Research and Review epub ahead of print (October 2018), https://journals.sagepub.com/doi/abs/10.1177/1077558718808709?rfr_dat=cr_pub%3Dpubmed&url_ver=Z39.88-2003&rfr_id=ori%3Arid%3Acrossref.org&journalCode=mcrd ↩︎
- Brandy Lipton, Sandra Decker, and Benjamin Sommers, “The Affordable Care Act Appears to Have Narrowed Racial and Ethnic Disparities in Insurance Coverage and Access to Care Among Young Adults” Medical Care Research and Review 76, no.1 (April 2017): 32–55, https://www.ncbi.nlm.nih.gov/pubmed/29148341 ↩︎
- Dahai Yue, Petra Rasmussen, and Ninez Ponce, “Racial/Ethnic Differential Effects of Medicaid Expansion on Health Care Access,” Health Services Research (February 2018), http://onlinelibrary.wiley.com/doi/10.1111/1475-6773.12834/abstract ↩︎
- Thomas Buchmueller and Helen Levy, “The ACA’s Impact On Racial And Ethnic Disparities In Health Insurance Coverage And Access To Care,” Health Affairs 39, no. 3 (March 2020): 395-402, https://doi.org/10.1377/hlthaff.2019.01394 ↩︎
- Jesse C. Baumgartner, Sara R. Collins, David C. Radley, and Susan L. Hayes, How the Affordable Care Act Has Narrowed Racial and Ethnic Disparities in Access to Health Care (The Commonwealth Fund, January 2020), https://www.commonwealthfund.org/publications/2020/jan/how-ACA-narrowedracial-ethnic-disparities-access ↩︎
- Hyunjung Lee and Frank Porell, “The Effect of the Affordable Care Act Medicaid Expansion on Disparities in Access to Care and Health Status,” Medical Care Research and Review epub ahead of print (October 2018), https://journals.sagepub.com/doi/abs/10.1177/1077558718808709?rfr_dat=cr_pub%3Dpubmed&url_ver=Z39.88-2003&rfr_id=ori%3Arid%3Acrossref.org&journalCode=mcrd ↩︎
- Jesse C. Baumgartner, Sara R. Collins, David C. Radley, and Susan L. Hayes, How the Affordable Care Act Has Narrowed Racial and Ethnic Disparities in Access to Health Care (The Commonwealth Fund, January 2020), https://www.commonwealthfund.org/publications/2020/jan/how-ACA-narrowedracial-ethnic-disparities-access ↩︎
- Susan Hayes, Sara Collins, David Radley, and Douglas McCarthy, What’s at Stake: States’ Progress on Health Coverage and Access to Care, 2013-2016 (The Commonwealth Fund, December 2017), http://www.commonwealthfund.org/publications/issue-briefs/2017/dec/states-progress-health-coverageand-access ↩︎
- Susan Hayes, Pamela Riley, David Radley, and Douglas McCarthy, Reducing Racial and Ethnic Disparities in Access to Care: Has the Affordable Care Act Made a Difference? (The Commonwealth Fund, August 2017), http://www.commonwealthfund.org/publications/issue-briefs/2017/aug/racial-ethnicdisparities-care ↩︎
- Dahai Yue, Petra Rasmussen, and Ninez Ponce, “Racial/Ethnic Differential Effects of Medicaid Expansion on Health Care Access,” Health Services Research (February 2018), http://onlinelibrary.wiley.com/doi/10.1111/1475-6773.12834/abstract ↩︎
- Xuesong Han et al., “Changes in Noninsurance and Care Unaffordability Among Cancer Survivors Following the Affordable Care Act,” Journal of the National Cancer Institute Epub ahead of print (November 2019), https://doi.org/10.1093/jnci/djz218 ↩︎
- Jesse C. Baumgartner, Sara R. Collins, David C. Radley, and Susan L. Hayes, How the Affordable Care Act Has Narrowed Racial and Ethnic Disparities in Access to Health Care (The Commonwealth Fund, January 2020), https://www.commonwealthfund.org/publications/2020/jan/how-ACA-narrowedracial-ethnic-disparities-access ↩︎
- Thomas Buchmueller and Helen Levy, “The ACA’s Impact On Racial And Ethnic Disparities In Health Insurance Coverage And Access To Care,” Health Affairs 39, no. 3 (March 2020): 395-402, https://doi.org/10.1377/hlthaff.2019.01394 ↩︎
- Andrew Crocker et al., “Expansion Coverage And Preferential Utilization Of Cancer Surgery Among Racial And Ethnic Minorities And Low-Income Groups,” Surgery epub ahead of print (June 2019), https://www.surgjournal.com/article/S0039-6060(19)30198-9/fulltext ↩︎
- Nathalie Huguet et al., “Cervical And Colorectal Cancer Screening Prevalence Before And After Affordable Care Act Medicaid Expansion,” Preventative Medicine (May 2019), https://doi.org/10.1016/j.ypmed.2019.05.003 ↩︎
- David Barrington et. al., “Where You Live Matters: A National Cancer Database Study of Medicaid Expansion and Endometrial Cancer Outcomes,” Gynecologic Oncology Epub ahead of print (June 2020), https://doi.org/10.1016/j.ygyno.2020.05.018 ↩︎
- Justin Le Blanc, Danielle Heller, Ann Friedrich, Donald Lannin, and Tristen Park, “Association of Medicaid Expansion Under the Affordable Care Act With Breast Cancer Stage at Diagnosis,” JAMA Surgery (July 2020), https://doi.org/10.1001/jamasurg.2020.1495 ↩︎
- Dahai Yue, Petra Rasmussen, and Ninez Ponce, “Racial/Ethnic Differential Effects of Medicaid Expansion on Health Care Access,” Health Services Research (February 2018), http://onlinelibrary.wiley.com/doi/10.1111/1475-6773.12834/abstract ↩︎
- Yunwei Gai and John Marthinsen, “Medicaid Expansion, HIV Testing, and HIV-Related Risk Behaviors in the United States, 2010-2017,” American Journal of Public Health 109, no. 10 (October 2019): 1404- 1412, https://doi.org/10.2105/ajph.2019.305220 ↩︎
- Cheryl Zogg et al., “Impact of Affordable Care Act Insurance Expansion on Pre-Hospital Access to Care: Changes in Adult Perforated Appendix Admission Rates after Medicaid Expansion and the Dependent Coverage Provision,” Journal of the American College of Surgeons 228, no. 1 (January 2019): 29-43, https://www.journalacs.org/article/S1072-7515(18)32078-7/fulltext ↩︎
- Andrew Crocker et al., “Expansion Coverage And Preferential Utilization Of Cancer Surgery Among Racial And Ethnic Minorities And Low-Income Groups,” Surgery epub ahead of print (June 2019), https://www.surgjournal.com/article/S0039-6060(19)30198-9/fulltext ↩︎
- James McDermott et al., “Affordable Care Act’s Medicaid Expansion and Use of Regionalized Surgery at High-Volume Hospitals,” Journal of the American College of Surgeons 227, no. 5 (November 2018): 507-520.e9, https://www.journalacs.org/article/S1072-7515(18)31993-8/abstrac ↩︎
- Kelsie M. Gould et al., “Bariatric Surgery Among Vulnerable Populations: The Effect of the Affordable Care Act’s Medicaid Expansion,” Surgery 166, no. 5 (November 2019): 820-828, https://doi.org/10.1016/j.surg.2019.05.005 ↩︎
- Afshin Ehsan et al., “Utilization of Left Ventricular Assist Devices in Vulnerable Adults Across Medicaid Expansion,” Journal of Surgical Research 243 (November 2019): 503-508, https://doi.org/10.1016/j.jss.2019.05.015 ↩︎
- Khadijah Breathett et al., “Is the Affordable Care Act Medicaid Expansion Linked to Change in Rate of Ventricular Assist Device Implantation for Blacks and Whites?” Circulation: Heart Failure 13, no. 4 (April 2020), https://doi.org/10.1161/CIRCHEARTFAILURE.119.006544 ↩︎
- Khadijah Breathett et al., “The Affordable Care Act Medicaid Expansion Correlated with Increased Heart Transplant Listings in African Americans but Not Hispanics or Caucasians,” JACC: Heart Failure 5 no. 2 (January 2017): 136-147, https://www.ncbi.nlm.nih.gov/pubmed/28109783 ↩︎
- Brendan Saloner, Rachel Landis, Bradley Stein, and Colleen Barry, “The Affordable Care Act in the Heart of the Opioid Crisis: Evidence from West Virginia,” Health Affairs 38, no. 4 (April 2019), https://www.healthaffairs.org/doi/full/10.1377/hlthaff.2018.05049 ↩︎
- Nadia Laniado, Avery R. Brow, Eric Tranby, and Victor M. Badner, “Trends in Non-Traumatic Dental Emergency Department Use in New York and New Jersey: A Look at Medicaid Expansion from Both Sides of the Hudson River,” Journal of Public Health Dentistry Epub ahead of print (October 2019), https://doi.org/10.1111/jphd.12343 ↩︎
- Khadijah Breathett et al., “The Affordable Care Act Medicaid Expansion Correlated with Increased Heart Transplant Listings in African Americans but Not Hispanics or Caucasians,” JACC: Heart Failure 5 no. 2 (January 2017): 136-147, https://www.ncbi.nlm.nih.gov/pubmed/28109783 ↩︎
- Adrian Diaz, Daniel Chavarin, Anghela Z. Paredes, and Timothy M. Pawlik, “Utilization of High-Volume Hospitals for High-Risk Cancer Surgery in California Following Medicaid Expansion,” Journal of Gastrointestinal Surgery Epub ahead of print (July 2020), https://link.springer.com/article/10.1007/s11605-020-04747-8 ↩︎
- Brendan Saloner, Rachel Landis, Bradley Stein, and Colleen Barry, “The Affordable Care Act in the Heart of the Opioid Crisis: Evidence from West Virginia,” Health Affairs 38, no. 4 (April 2019), https://www.healthaffairs.org/doi/full/10.1377/hlthaff.2018.05049 ↩︎
- Erica Eliason, “Adoption of Medicaid Expansion Is Associated with Lower Maternal Mortality,” Women’s Health Issues 30, no. 3 (May-June 2020): 147-152, https://doi.org/10.1016/j.whi.2020.01.005 ↩︎
- Chintan Bhatt and Consuelo Beck-Sague, “Medicaid Expansion and Infant Mortality in the United States,” American Journal of Public Health 108, no. 4 (April 2018): 565-567, https://ajph.aphapublications.org/doi/full/10.2105/AJPH.2017.304218 ↩︎
- Alexandra Wiggins, Ibraheem M. Karaye, Jennifer A. Horney, “Medicaid Expansion and Infant Mortality, Revisited: A Difference-In-Differences Analysis,” Health Services Research 55, no. 3 (March 2020): 393-398, https://doi.org/10.1111/1475-6773.13286 ↩︎
- Clare Brown et al., “Association of State Medicaid Expansion Status With Low Birth Weight and Preterm Birth” Journal of the American Medical Association 321, no. 16 (April 2019), https://jamanetwork.com/journals/jama/fullarticle/2731179 ↩︎
- Clare Brown, Jennifer Moore, Felix Holly, Kathryn Stewart, and Mick Tilford, “County-level Variation in Low Birthweight and Preterm Birth: An Evaluation of State Medicaid Expansion Under the Affordable Care Act,” Medical Care 58, no. 6 (June 2020): 497-503, https://doi.org/10.1097/mlr.0000000000001313 ↩︎
- Hyunjung Lee and Frank Porell, “The Effect of the Affordable Care Act Medicaid Expansion on Disparities in Access to Care and Health Status,” Medical Care Research and Review epub ahead of print (October 2018), https://journals.sagepub.com/doi/abs/10.1177/1077558718808709?rfr_dat=cr_pub%3Dpubmed&url_ver=Z39.88-2003&rfr_id=ori%3Arid%3Acrossref.org&journalCode=mcrd ↩︎
- Minal R. Patel et al., “Examination of Changes in Health Status Among Michigan Medicaid Expansion Enrollees From 2016 to 2017,” JAMA Network Open 3, no. 7 (July 2020), https://doi.org/10.1001/jamanetworkopen.2020.8776 ↩︎
- Shailender Swaminathan, Benjamin Sommers, Rebecca Thorsness, Rajnish Mehrotra, Yoojin Lee, and Amal Trivedi, “Association of Medicaid Expansion With 1-Year Mortality Among Patients With End Stage Renal Disease,” Journal of the American Medical Association (JAMA) 320, no. 21 (December 2018): 2242 2250, https://jamanetwork.com/journals/jama/fullarticle/2710505?guestAccessKey=ea3a8641-320b-4afd-b96edc59fbd90b20&utm_source=TrendMD &utm_medium=cpc&utm_campaign=J_Am_Med_TrendMD_1&utm_content=olf&utm_term=102518 ↩︎
- David Barrington et. al., “Where You Live Matters: A National Cancer Database Study of Medicaid Expansion and Endometrial Cancer Outcomes,” Gynecologic Oncology Epub ahead of print (June 2020), https://doi.org/10.1016/j.ygyno.2020.05.018 ↩︎
- Manzilat Akande, Peter Minneci, Katherine Deans, Henry Xiang, Deena Chisolm, and Jennifer Cooper, “Effects Of Medicaid Expansion On Disparities In Trauma Care And Outcomes In Young Adults,” Journal of Surgical Research 228 (August 2018): 42-53, https://www.sciencedirect.com/science/article/pii/S0022480418301562 ↩︎
- Cheryl Zogg et al., “Association of Medicaid Expansion With Access to Rehabilitative Care in Adult Trauma Patients,” JAMA Surgery epub ahead of print (January 2019), https://jamanetwork.com/journals/jamasurgery/articleabstract/2719270?utm_campaign=articlePDF&utm_medium=articlePDFlink&utm_source=articlePDF &utm_content=jamasurg.2018.5177 ↩︎
- Cheryl Zogg et al., “Impact of Affordable Care Act Insurance Expansion on Pre-Hospital Access to Care: Changes in Adult Perforated Appendix Admission Rates after Medicaid Expansion and the Dependent Coverage Provision,” Journal of the American College of Surgeons 228, no. 1 (January 2019): 29-43, https://www.journalacs.org/article/S1072-7515(18)32078-7/fulltext ↩︎
- Cheryl Zogg et al., “Association of Medicaid Expansion With Access to Rehabilitative Care in Adult Trauma Patients,” JAMA Surgery epub ahead of print (January 2019), https://jamanetwork.com/journals/jamasurgery/articleabstract/2719270?utm_campaign=articlePDF&utm_medium=articlePDFlink&utm_source=articlePDF &utm_content=jamasurg.2018.5177 ↩︎
- Meera Harhay et al., “Association between Medicaid Expansion under the Affordable Care Act and Preemptive Listings for Kidney Transplantation,” Clinical Journal of the American Society of Nephrology 13 (July 2018), https://cjasn.asnjournals.org/content/13/7/1069 ↩︎
- Heather Angier et al., “Racial/Ethnic Disparities in Health Insurance and Differences in Visit Type for a Population of Patients with Diabetes after Medicaid Expansion,” Journal of Health Care for the Poor and Underserved 30, no.1, (March 2019): 116–130, https://www.ncbi.nlm.nih.gov/pmc/articles/PMC6429963/ ↩︎
- J.W. Awori Hayanga et al., “Lung Transplantation and Affordable Care Act Medicaid Expansion in the Era of Lung Allocation Score” Transplant International Epub ahead of print (February 2019), https://onlinelibrary.wiley.com/doi/pdf/10.1111/tri.13420 ↩︎
- Heather Angier et al., “Uninsured Primary Care Visit Disparities under the Affordable Care Act,” Annals of Family Medicine, 15 no. 5 (September 2017): 434-442, http://www.annfammed.org/content/15/5/434.full.pdf+html ↩︎
- Heather Angier et al., “Racial/Ethnic Disparities in Health Insurance and Differences in Visit Type for a Population of Patients with Diabetes after Medicaid Expansion,” Journal of Health Care for the Poor and Underserved 30, no.1, (March 2019): 116–130, https://www.ncbi.nlm.nih.gov/pmc/articles/PMC6429963/ ↩︎
- Adrian Diaz, Daniel Chavarin, Anghela Z. Paredes, and Timothy M. Pawlik, “Utilization of High-Volume Hospitals for High-Risk Cancer Surgery in California Following Medicaid Expansion,” Journal of Gastrointestinal Surgery Epub ahead of print (July 2020), https://link.springer.com/article/10.1007/s11605-020-04747-8 ↩︎
- Renuka Tipirneni et al., “Association of Medicaid Expansion With Enrollee Employment and Student Status in Michigan,” JAMA Network Open 3, no. 1 (January 2020), https://doi.org/10.1001/jamanetworkopen.2019.20316 ↩︎
- Heeju Sohn and Stefan Timmermans, “Social Effects of Health Care Reform: Medicaid Expansion under the Affordable Care Act and Changes in Volunteering,” Socius: Socialogical Research for a Dynamic World 3 (March 2017): 1-12, http://journals.sagepub.com/doi/full/10.1177/2378023117700903 ↩︎
- Kevin Callison and Paul Sicilian, “Economic Freedom and the Affordable Care Act: Medicaid Expansions and Labor Mobility by Race and Ethnicity,” Public Finance Review 46, no. 2 (March 2018), https://journals.sagepub.com/doi/abs/10.1177/1091142116668254 ↩︎