Women’s Experiences with Health Care During the COVID-19 Pandemic: Findings from the KFF Women’s Health Survey
Findings
Key Takeaways
- Women are more likely to have gone without health care during the pandemic compared to men, and women with health and economic challenges prior to the pandemic have experienced worsening health conditions as a result of skipping health care services during the pandemic. These gaps in care could translate into higher numbers of women experiencing severe health issues after the health emergency from the pandemic resolves.
- People have been largely satisfied with their telemedicine interactions. The share of men and women who at the time of the survey reported having a telemedicine visit during the pandemic tripled since before the pandemic. But not all have had the opportunity or access to telemedicine. Older women, women with higher educational attainment, insured women, and women living in states that have expanded Medicaid are more likely to have had a telehealth visit during the pandemic. While telemedicine played an important role during the pandemic, is it still not clear whether it will continue to be an approach that providers and health consumers will continue to utilize at high rates as the risk of exposure to the coronavirus recedes.
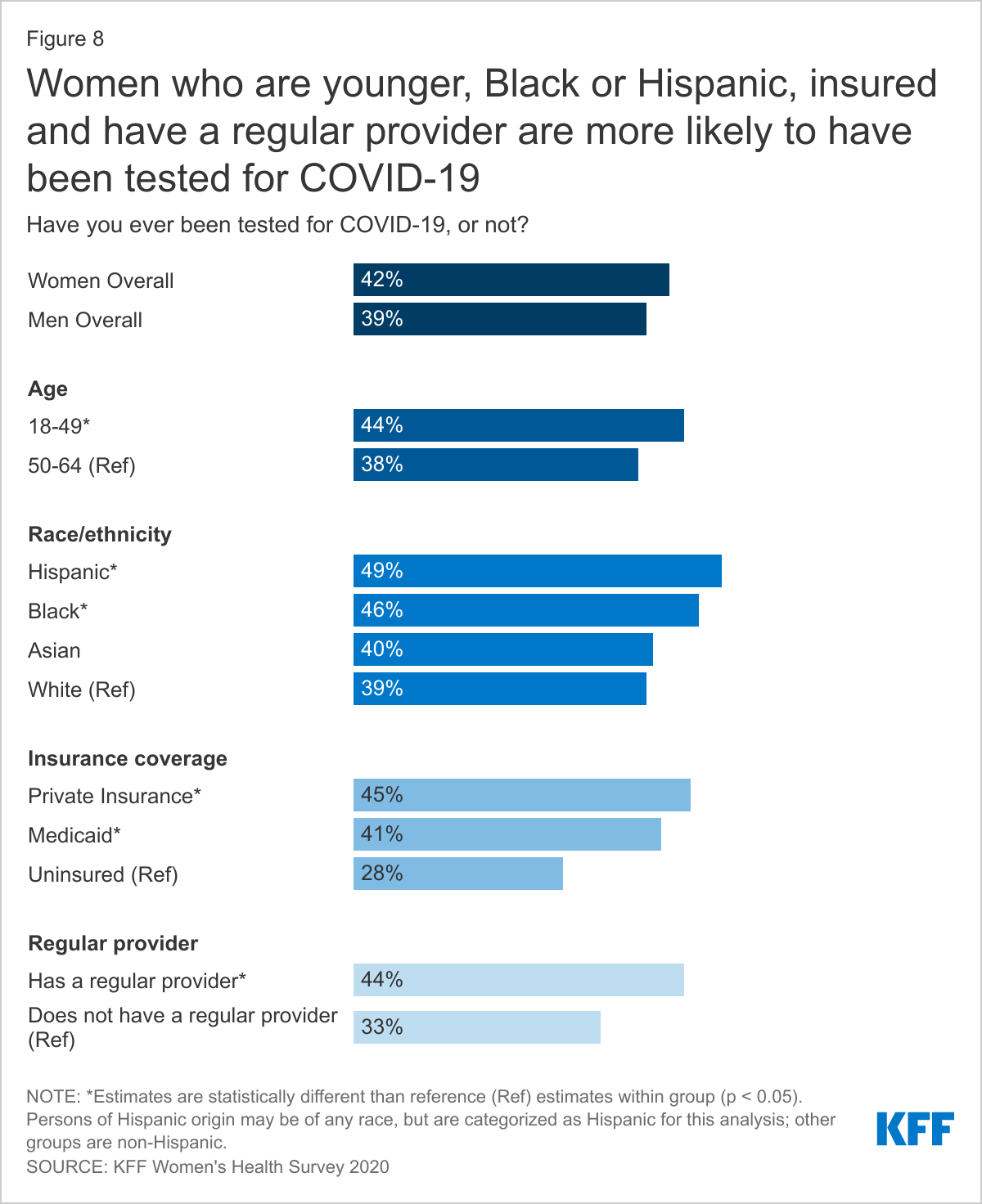
- Women with private insurance and Medicaid are nearly twice as likely to have received a COVID-19 test compared to uninsured women (45% and 41% vs. 28%). Uninsured individuals may have been less likely to seek a test out of fear of cost, which could have implications for uptake of COVID-19 vaccines, even though all COVID-19 vaccines are free regardless of insurance status.
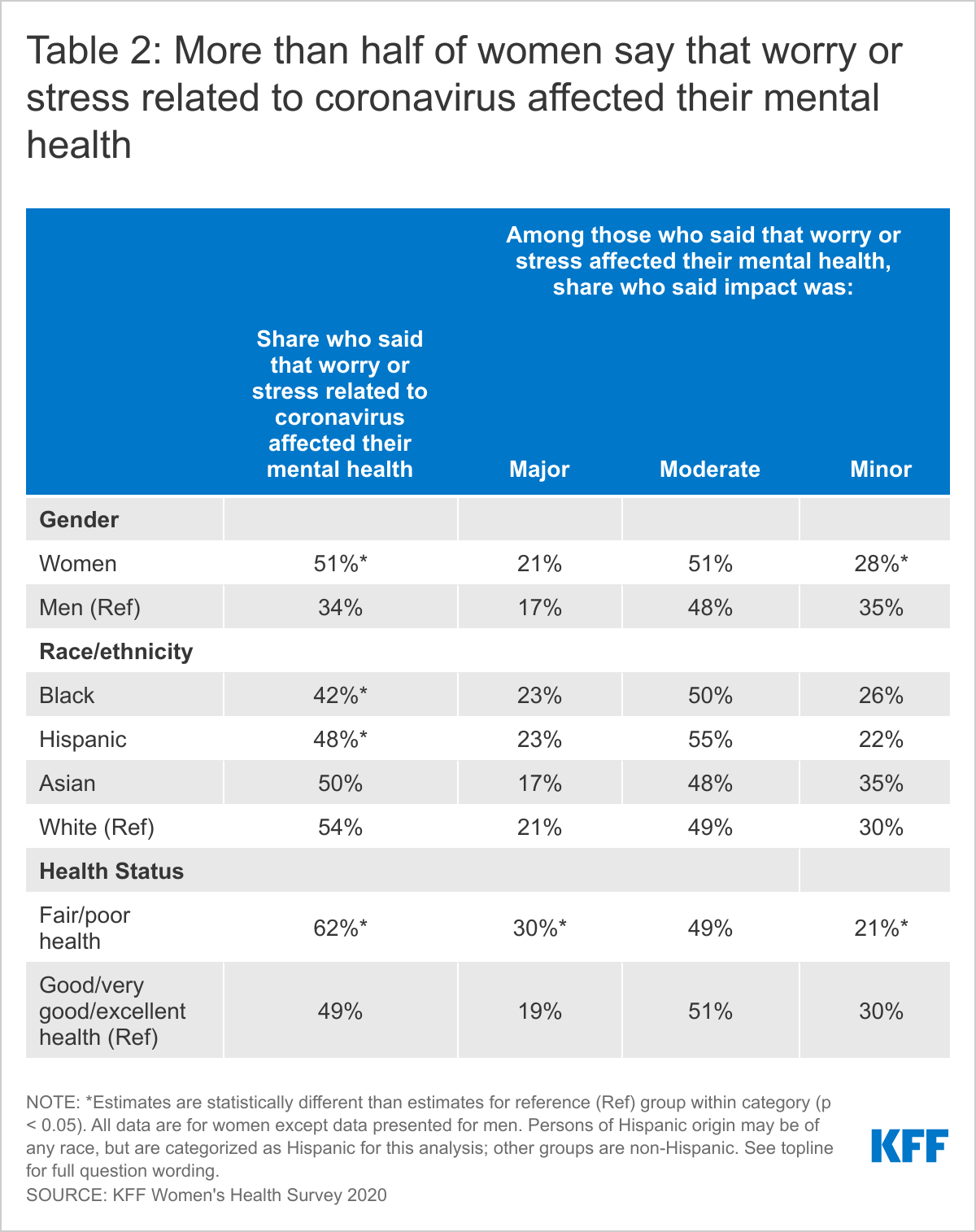
- The pandemic has had a significant effect on people’s mental health, with 51% of women and 34% of men saying that worry or stress related to the pandemic has affected their mental health. Most say that the impact has been moderate or minor, but almost one-fifth (21% women, 17% men) say the toll has taken a major impact on their mental health. The high need for mental health care has highlighted long-standing gaps in the availability and signals that the demand will likely continue as people begin to process the trauma and loss they have experienced over the past year.
Introduction
The COVID-19 pandemic transformed the way people access health care, with care quickly moving to telehealth. However, with fear of contracting the coronavirus and state emergency declarations limiting non-essential and elective services in the early days of the pandemic, many people have gone without health care services this year. The pandemic has highlighted and aggravated long-standing inequities in healthcare availability and access. This brief provides new data from the KFF Women’s Health Survey, a nationally representative survey of 3,661 women and 1,144 men ages 18-64 (Methodology) that was conducted November 19, 2020 – December 17, 2020. Among several topics related to women’s health and well-being, we asked respondents about experiences during the COVID-19 pandemic. In this brief, we document how experiences accessing health care during the COVID-19 pandemic have differed by gender, age, race/ethnicity, insurance coverage, and income and what this could mean moving forward.
Accessing Health Care During the COVID-19 Pandemic
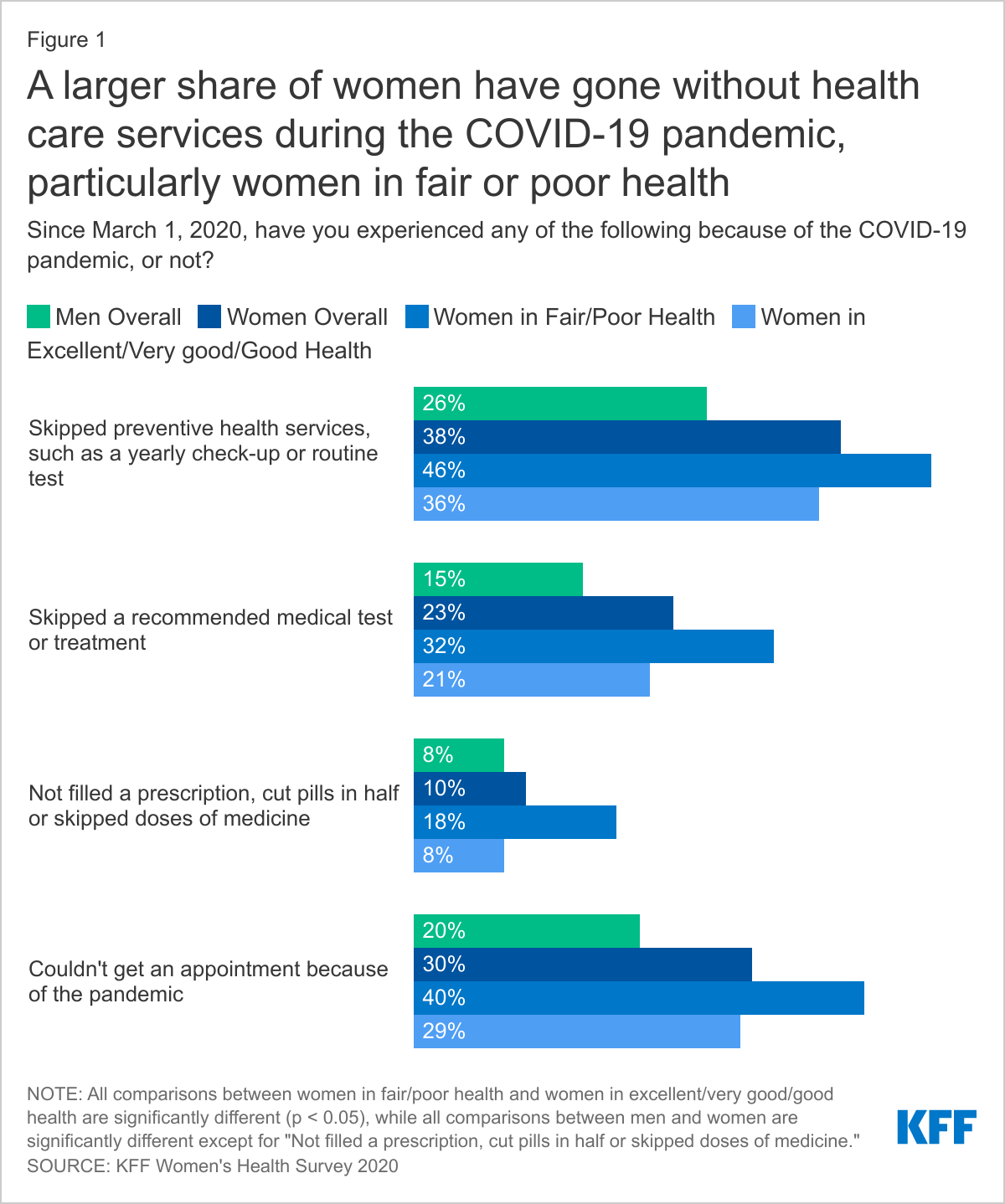
A higher share of women than men have skipped recommended preventive services in response to the pandemic. When asked about their experiences accessing health care services during the pandemic, a larger share of women than men say they have skipped preventive health services, such as a yearly check-up or routine test (38% vs. 26%) or skipped a recommended medical test or treatment (23% vs. 15%). Nearly half of women who report being in fair or poor health report skipping preventive care (46%) and nearly one-third have skipped recommended tests or treatment (32%) compared to women who reported being in good, very good, or excellent health (36% and 21%, respectively). Those in poor health may view themselves as more at risk for COVID exposure and opt to skip routine preventive care. This gap in care among those with the greatest health problems could portend an increase of the share of patients experiencing more severe health conditions resulting from care that was foregone or delayed during the pandemic.
Surprisingly, women with incomes ≥200% of the federal poverty level (FPL) are more likely to have skipped preventive health services during the pandemic compared to women with incomes <200% FPL (40% vs. 33%, respectively),1 as well as women with private insurance (39%) and Medicaid (38%) compared to uninsured women (30%). A larger share of women with private insurance (23%) and Medicaid (26%) also report skipping a recommended medical test or treatment compared to uninsured women (18%). In pre-pandemic times, the reverse was true, higher shares of women with lower incomes and who lacked insurance coverage reported skipping care. Women with more resources may be choosing to skip care because of concerns of COVID exposure.
Nearly one in five women in fair or poor health (18%) say they have either not filled a prescription, cut pills in half or skipped doses of medicine because of the COVID-19 pandemic, over twice the percentage of women in good, very good, or excellent health (8%). A higher percentage of low-income women < 200% FPL (14%), uninsured individuals (12%), and those with Medicaid (12%) also report not filling a prescription, cutting pills in half or skipping doses of medicine compared to higher income women (≥ 200% FPL) (8%) and individuals with private insurance (8%).i
More women than men report not being able to get an appointment because of the pandemic (30% vs. 20%), which could be a result of women being more likely to seek care. A larger share of women in poor or fair health (40%) compared to women in good or excellent health (29%) and low-income women (<200% FPL) (33%) compared to higher income women (≥ 200% FPL) (29%) say they were unable to get appointments. State emergency declarations limited services deemed non-essential or elective and reduced clinic hours and closures have made it particularly difficult to access care during the pandemic.
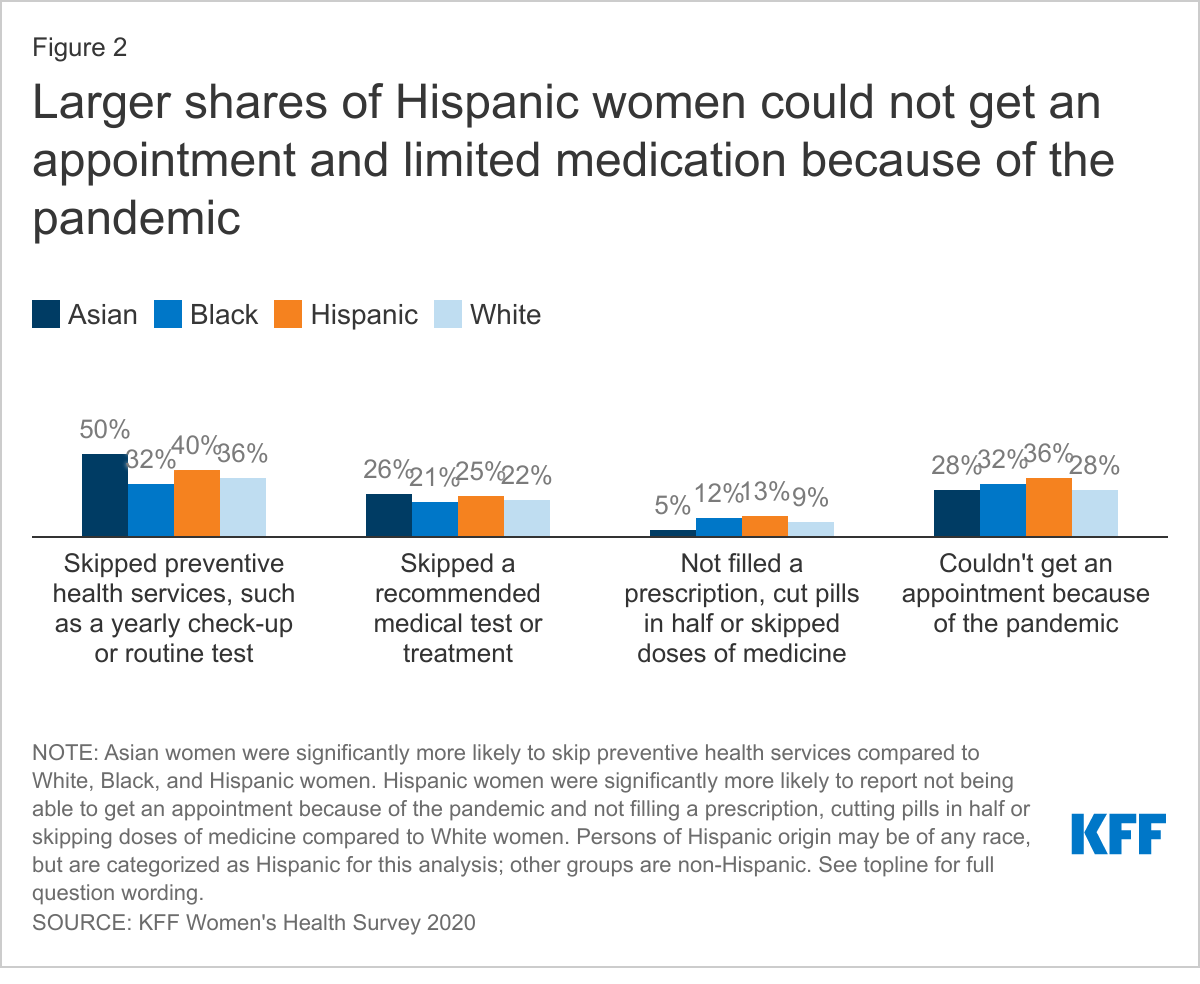
The pandemic has taken a disproportionate toll on some communities of color. Hispanic women, who have the highest rates of uninsurance, report higher rates of access barriers. Four in ten (40%) say they skipped preventive health services, 36% could not get a medical appointment, and 13% did not fill or skipped doses of prescription medicines because of the pandemic (Figure 2). Targeted outreach to this community regarding the COVID-19 vaccine will be important to ensure they have adequate access to and information about the vaccine, especially that the vaccine is free even without insurance.
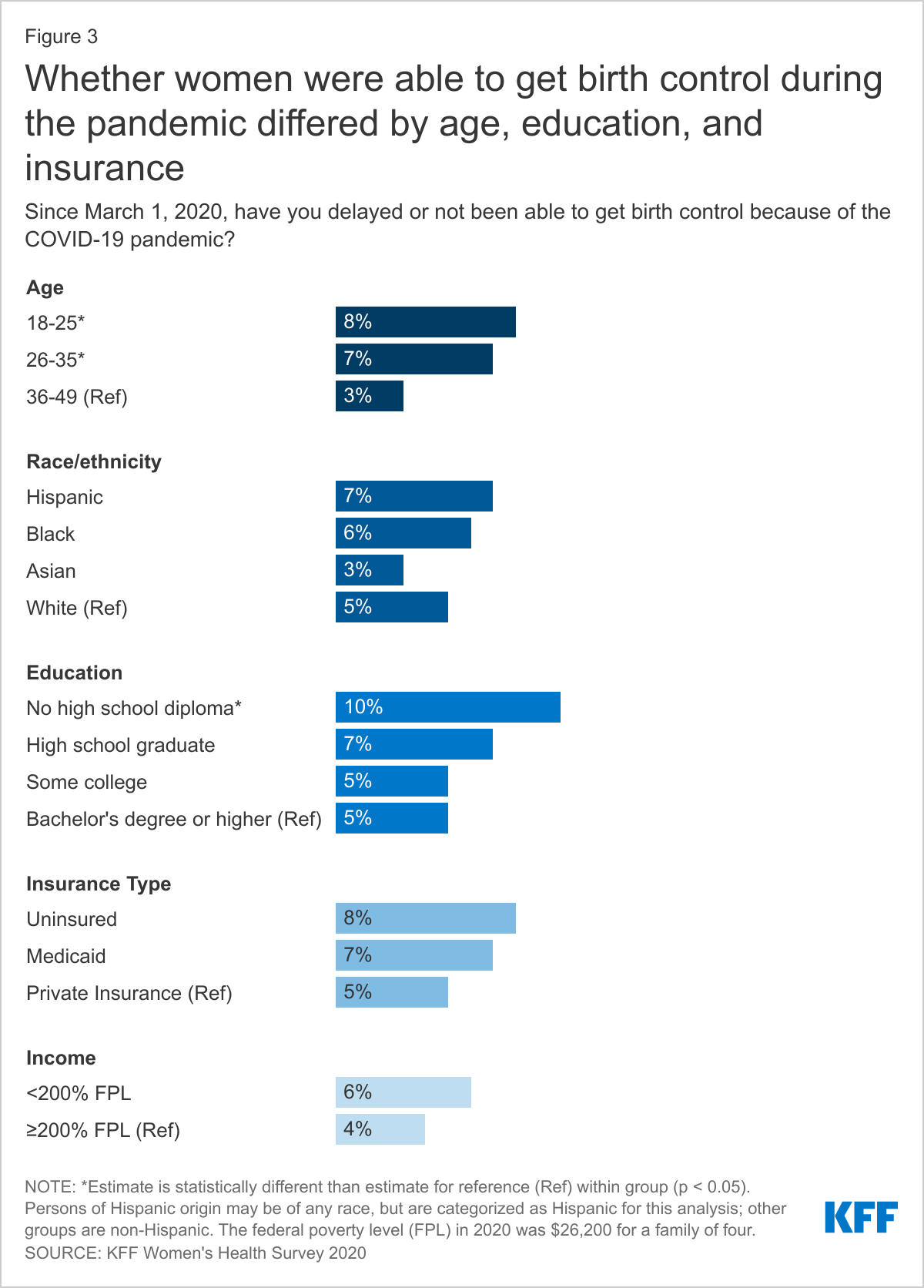
Nearly one in 10 women ages 18-25 (8%) and 7% of women ages 26-35 say they delayed or were not able to get birth control due to the COVID-19 pandemic, which is significantly higher than women ages 36-49 (3%) (Figure 3). Women without a high school diploma were more likely to report delaying or not being able to get birth control compared to women with a Bachelor’s degree or higher (10% vs. 5%). Individuals who face delays in contraceptive care could face negative health consequences, such as sexually transmitted infections or unwanted pregnancies. While many clinics developed protocols to distribute contraception to their clients by reducing the need for in-person visits through telemedicine or other distribution approaches, addressing access for younger women and those with few resources will continue to be important.
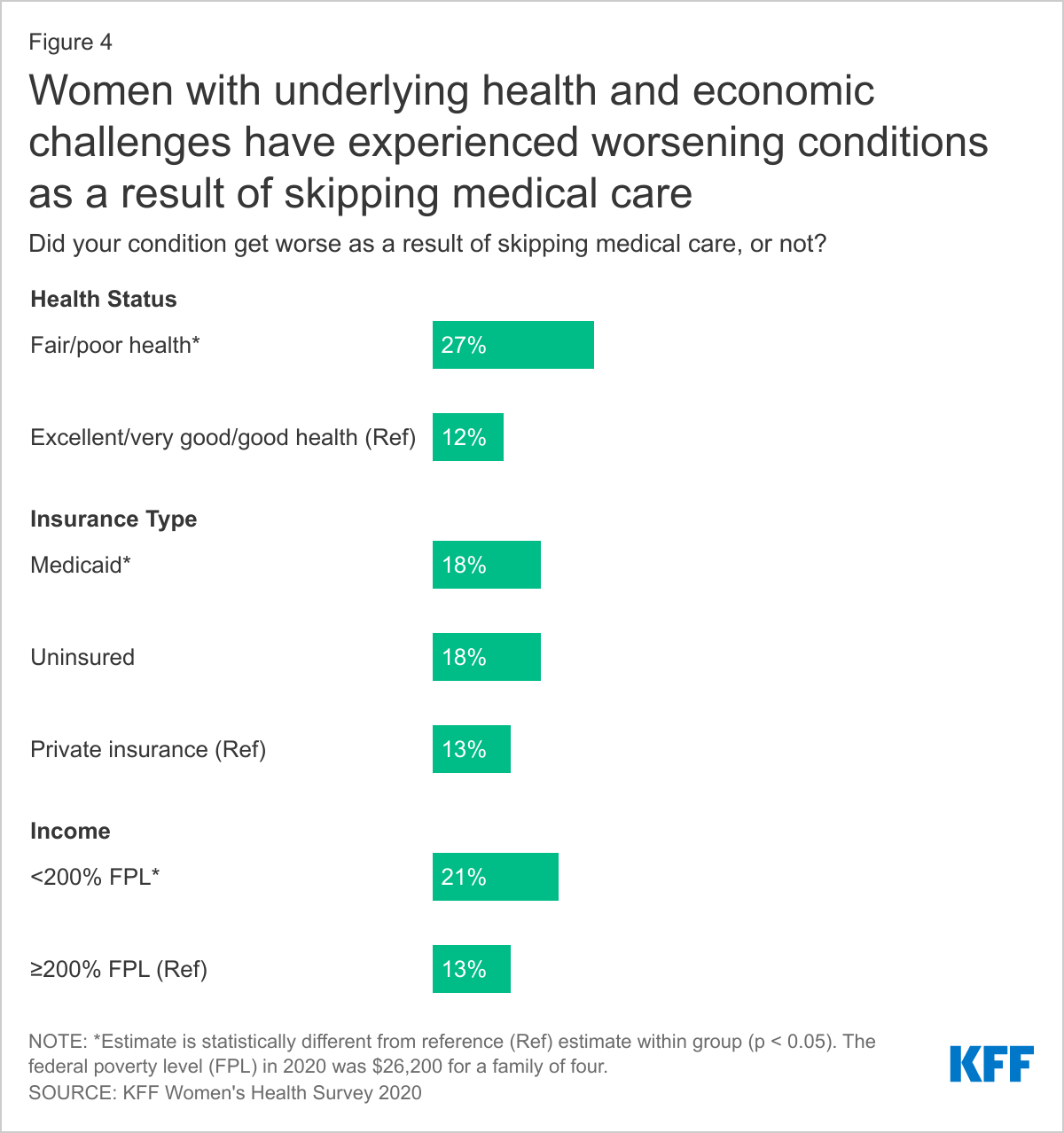
Delays in accessing health care can translate into worsening health conditions, especially for women with underlying health problems that have been exacerbated by lack of care and those who face economic challenges that have gone without care due to cost. Among those who have skipped receiving health care services, women in fair or poor health, those with Medicaid coverage, and those with low incomes are more likely than other groups of women to report that their condition has worsened as a result of skipping care (Figure 4). Providers should be prepared to respond to greater health needs among their patients who have skipped care.
Telehealth
The rapid expansion of telehealth visits has broadened the ways in which people have been able to access care throughout the pandemic. Our survey defines telehealth/telemedicine as an appointment with a provider conducted by telephone or video conference in place of an in-person visit. For this survey, telemedicine or telehealth does not include email, messages sent through a website, or general online health information. Please see the survey topline for full question wording.
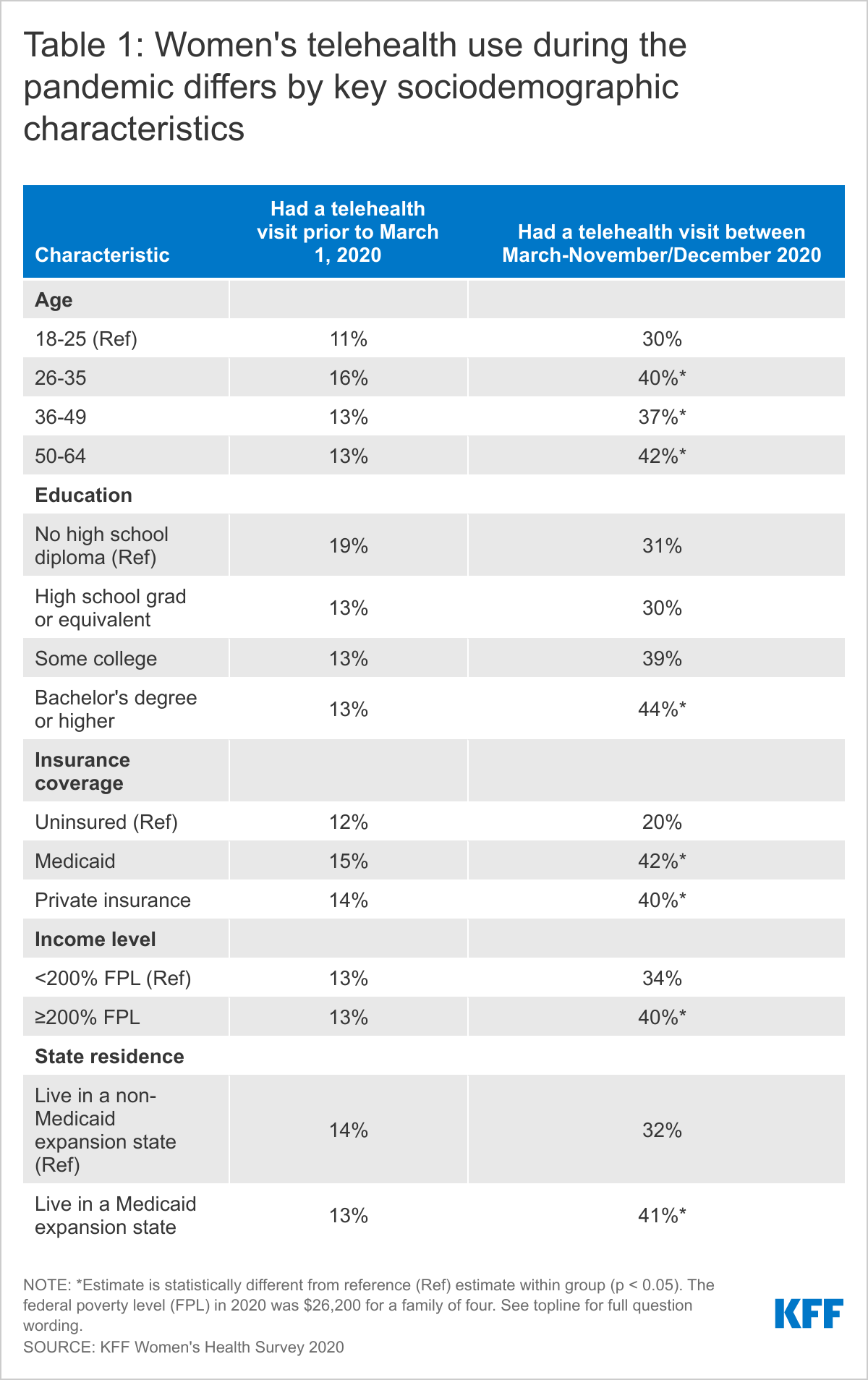
Prior to the pandemic, only about 1 in 10 men (11%) and women (13%) had received care via a telemedicine or telehealth visit. However, as of November/December when the survey was in the field approximately 1 in 3 men (32%) and women (38%) reported having a telemedicine or telehealth visit since March 1, 2020. Women over the age of 25, women with a college degree, insured women, and women living in states that have expanded Medicaid are more likely to have had a telehealth visit during the pandemic (Table 1).
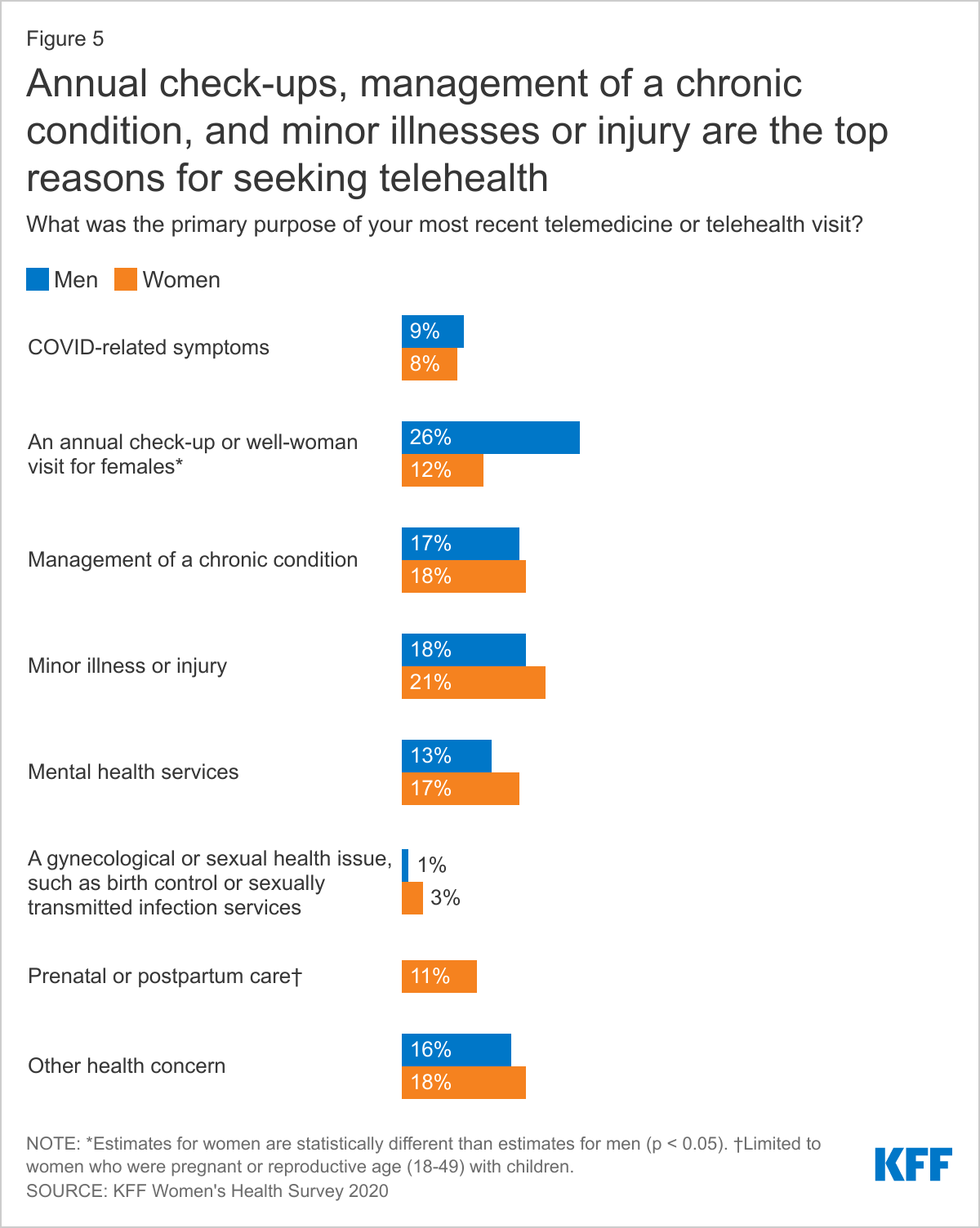
Surprisingly, COVID-related care was not a leading reason for seeking health care through telehealth. Just 8% of women and 9% of men say their most recent telehealth appointment was for COVID-related symptoms. More commonly, women report their most recent telehealth visits were to address a minor illness or injury (21%), management of a chronic condition (18%), and 17% for mental health services. While similar shares of women and men report these reasons for telehealth visits, one notable difference is that one-quarter of men (26%) say their most recent telehealth visit was for a checkup, compared to 12% of women (Figure 5).
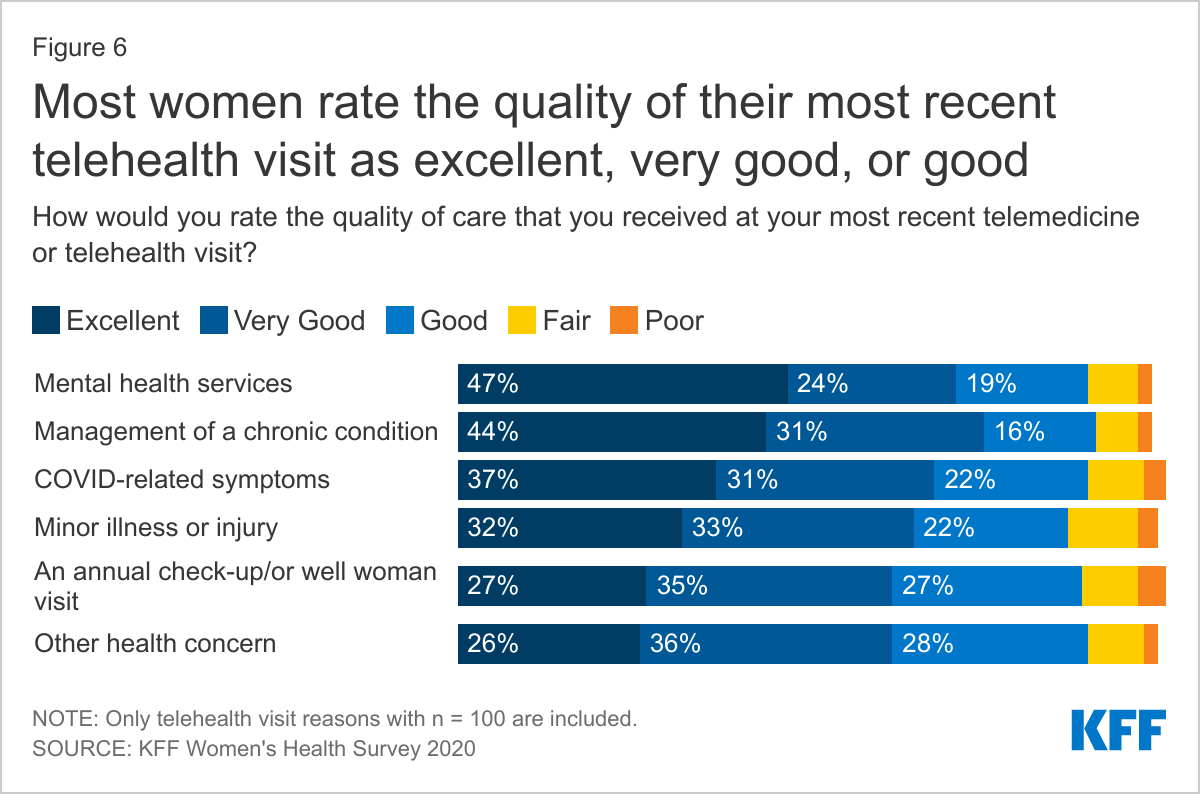
When asked to rate the care received at their most recent telemedicine or telehealth visit, most women showed high levels of satisfaction. A larger share of women rated the care they received at their most recent telemedicine or telehealth visit as excellent compared to men (35% vs. 29%). Telehealth care rated as excellent, very good, or good was more common among insured women with incomes ≥ 200% FPL compared to uninsured women with incomes < 200% FPL (91% vs. 86%) and women reporting being in excellent, very good, or good health compared to women who said their health was fair or poor (91% vs. 85%). There were no differences in ratings of telehealth quality by insurance status. Among women, telehealth mental health services received the largest share of excellent ratings and annual check-ups or well woman visits have the smallest share of excellent ratings, although ratings were still very positive with 89% of women rating their most recent telehealth annual check-up or well woman visit excellent, very good, or good (Figure 6). These data suggest most women are very satisfied with the telehealth services they have received and telehealth could continue to be a trusted approach to obtaining some types of health care services for individuals who would prefer or find it easier to access care from their home rather than traveling to a clinic or provider. However, there may be pressure from payers as the pandemic eases to once again limit telehealth due to cost concerns.
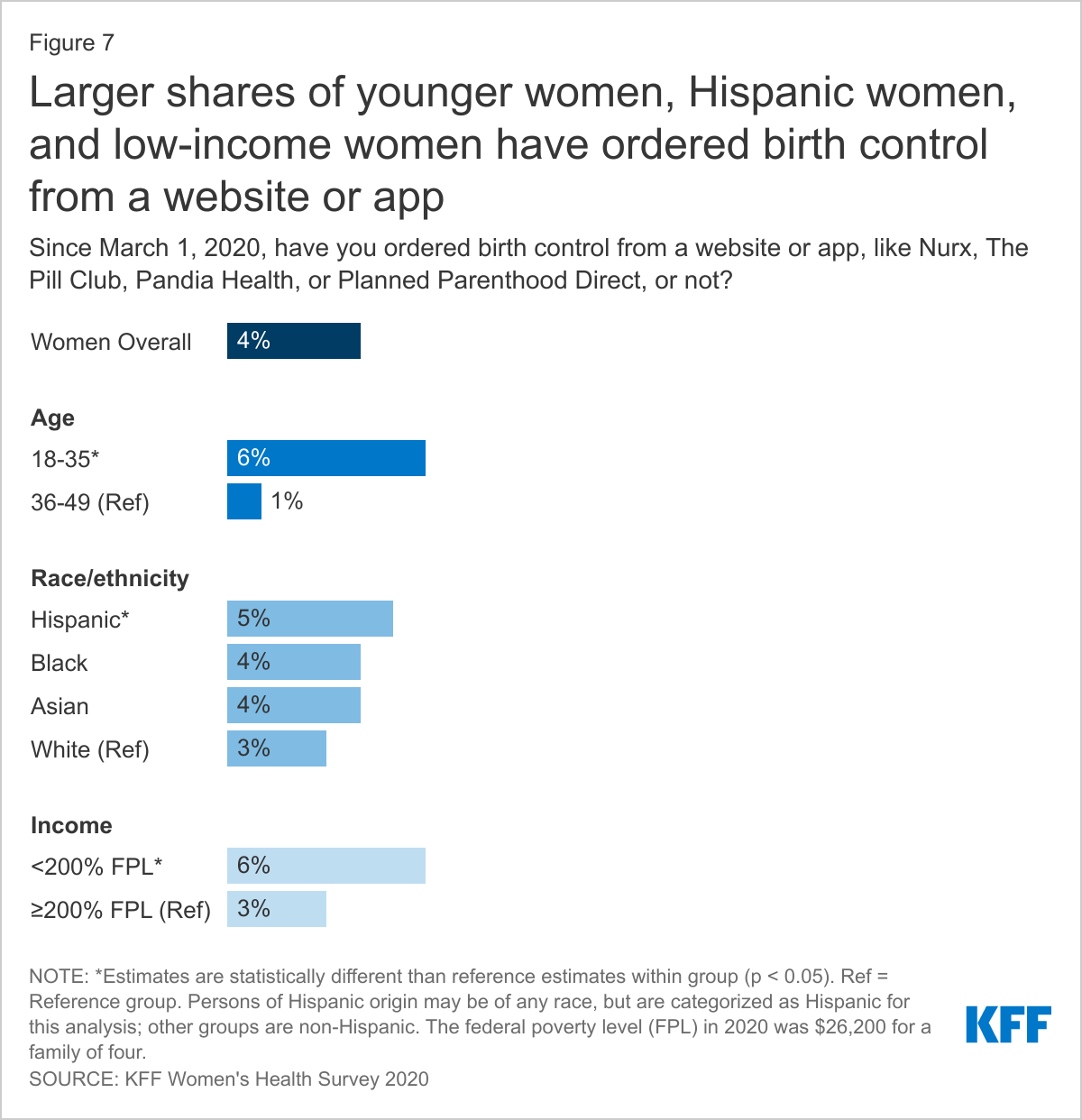
In recent years, there has been a proliferation of online companies that offer consumers access to primary care services, including sexual and reproductive health services like sexually transmitted infection testing, as well as prescriptions for everything from contraception to hair loss treatment. While these companies predate the pandemic, most are still relatively new. A small fraction of women (4%) ages 18-49 say they have ordered birth control from a website or app, like Nurx, The Pill Club, Pandia Health, or Planned Parenthood Direct. Younger women ages 18-35 (6%) in particular, are more likely to have ordered contraception from these companies compared to those ages 36-49 (1%). Some of these platforms do not accept insurance or Medicaid and may appeal to some uninsured or low-income women because of their costs. A larger share of Hispanic women (5%) compared to White women (3%) and low-income women (<200% FPL) (6%) compared to higher income women (≥ 200% FPL) (3%) have also used these online contraception platforms (Figure 7). While there is still a relatively small share of women using these online companies to obtain contraception, many of these companies have seen significant growth during the pandemic.
COVID-19 Testing
At the time that we fielded this survey in November-December 2020, four in ten women (42%) ages 18-64 had ever been tested for COVID-19 (Figure 8). Larger shares of younger women ages 18-49 (44%) had been tested compared to older women ages 50-64 (38%). Black (46%) and Hispanic (49%) women are also more likely to have been tested for COVID-19 compared to White women (39%).2 Women with private insurance and Medicaid have been nearly twice as likely to have received a COVID-19 test compared to uninsured women (45% and 41% vs. 28%), which could, in part, reflect uncertainty about or inability to afford out-of-pocket costs of COVID-19 tests without insurance. Women who reported having a regular provider are also more likely to have had a COVID-19 test compared to women who did not who do not have a regular health care provider (44% vs. 33%). Access to regular care results in more timely care and could also have implications for who is able to access COVID-19 vaccines, especially if documentation of a pre-existing condition is necessary for earlier vaccine groups.
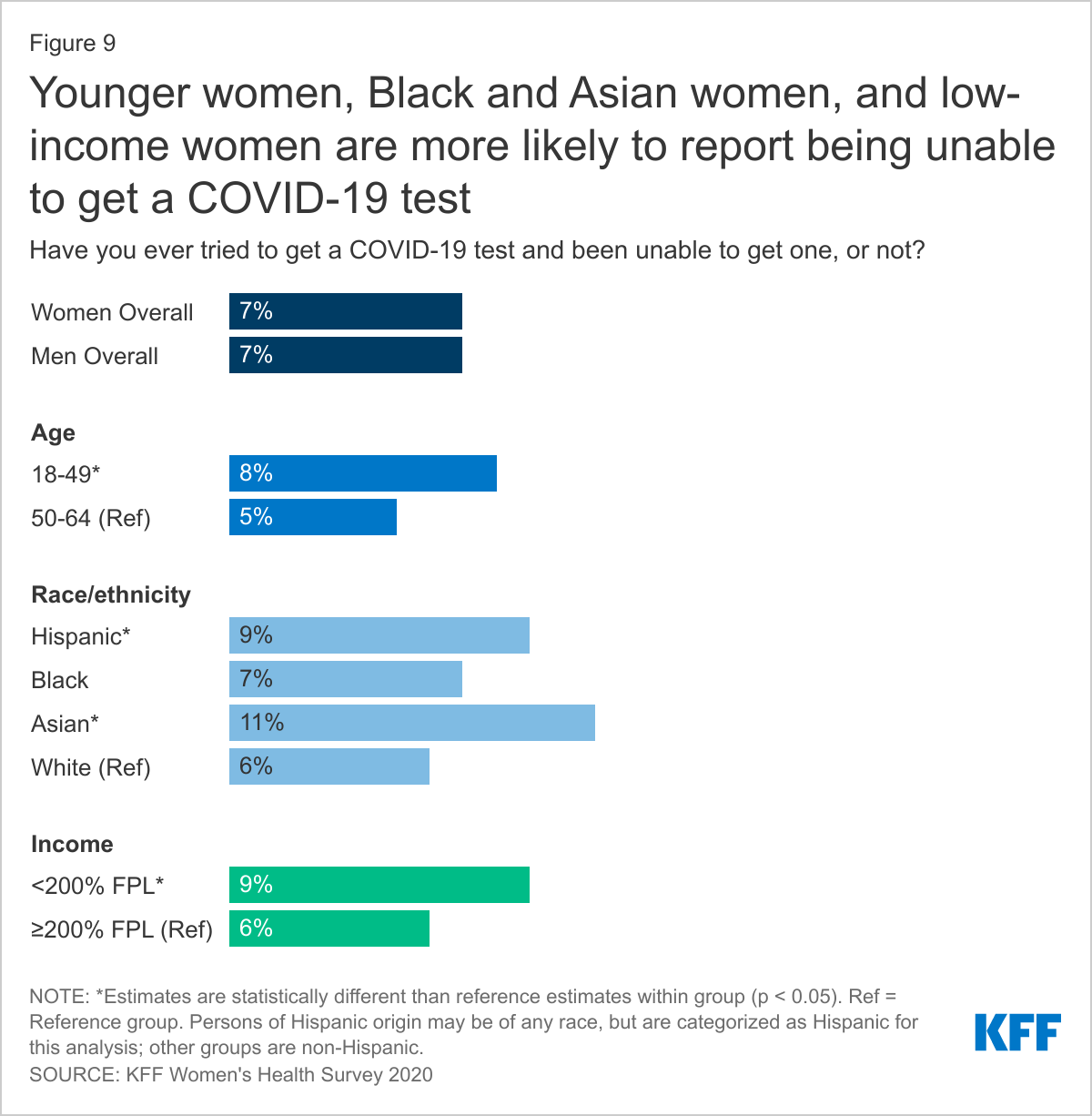
A small percentage of women reported trying to get a COVID-19 test and being unable to get one (7%) (Figure 9). While a higher share of younger women report being tested for COVID-19, they are also more likely to report not being able to get a test (8%) compared to women ages 50-64 (5%), which may reflect that younger women are more likely to be seeking tests than older women. A larger share of Asian/Pacific Islander (11%) and Hispanic (9%) women say they were unable to get a COVID-19 test compared to White (6%) women, while the share of Black women (7%) who couldn’t get a COVID test is similar to White women. A higher percentage of low-income women (< 200% FPL) (9%) report being unable to get a COVID-19 test compared to higher income (≥ 200% FPL) women (6%).
Impact on Mental Health
Numerous aspects of the pandemic have caused worry and stress, including concern about exposure to an infected individual, not being able to get tested, losing loved ones and jobs, working from home, and taking on additional childcare and homeschooling responsibilities. Half (51%) of women and about one-third of men (34%) say that worry or stress related to the pandemic has affected their mental health. While most (79% women, 83% men) say that the impact has been moderate or minor, almost one-fifth (21% women, 17% men) say the toll has had a major impact on their mental health (Table 2). Women who are already in fair or poor health are more likely than women in better health to say that the pandemic has had a major impact on their mental health.
Despite the toll of the pandemic on women’s mental health, relatively few (15%) say they sought mental health care. While White women (54%) are most likely to say that stress from the pandemic has affected their mental health, Hispanic (19%) and Asian (19%) women are most likely to report seeking mental health care. Uninsured women (10%) are less likely to seek mental health care compared to women with Medicaid (20%) and private insurance (15%). There is likely to be a growing need for mental health care as people process the trauma and loss they have experienced over the past year.
Conclusion
The COVID-19 pandemic changed how people access and use health care, and while the availability of options for telehealth care have grown rapidly and most people are satisfied with that care, it remains to be seen how acceptable these services will be as in person care resumes, and the requirements for payment parity are ended as the emergency measures are lifted by state and private sector payors. Many individuals are also having difficulties accessing care in this new environment or choosing not to seek care because of concerns about COVID exposure or risk. The survey finds that women have been more likely than men to forgo health care services during the pandemic, with many reporting worsening health conditions as a result. The expansion of telemedicine and virtual reproductive health care platforms have helped fill some of these gaps, but their reach is still limited, particularly for those without insurance or ready access to the internet or Wi-Fi. The burdens of the pandemic have had a negative impact on women’s mental health, though relatively few have reported seeking mental health care. Policies that promote stable insurance coverage, access to telehealth and mental health services, and the availability of safe in-person care can support women in obtaining needed health care for the remainder of the pandemic and beyond.
Methodology
The 2020 KFF Women’s Health Survey was designed and analyzed by researchers at the Kaiser Family Foundation (KFF) of a representative sample of 4,805 adults, ages 18-64 years old (3,661 women and 1,144 men). The survey was conducted online and telephone using AmeriSpeak®, the probability-based panel of NORC at the University of Chicago. U.S. households are recruited for participation using address-based sampling methodology and initial invitations for participation are sent by mail, telephone, and in-person interviews. Interviews for this survey were conducted between November 19 and December 17, 2020, among adults living in the United States. KFF paid for all costs associated with the survey.
The sample for this study was stratified by age, race/ethnicity, education, and gender as well as disproportionate stratification aimed at reaching uninsured women, women who identify as LGBT, and women 18-49 years old. The sampling also took into consideration differential survey completion rates by demographic groups so that the set of panel members with a completed interview for a study is a representative sample of the target population. Interviews were conducted in English and Spanish online (4,636) and via the telephone (169).
A series of data quality checks were run and cases determined to be poor-quality, as defined by surveys with a length of interview of less than 33% of the mean length of interview and with high levels of question refusal (>50%) were removed from the final data (n=96). Weighting involved multiple stages. First, the sample was weighted to match estimates for the national population from the 2020 Current Population Survey on age, gender, census division, race/ethnicity, and education. The second round of weights adjusted for the study’s sampling design. All statistical tests of significance account for the effect of weighting.
The margin of sampling error including the design effect for the full sample of women is plus or minus 2 percentage points. Numbers of respondents and margins of sampling error for key subgroups are shown in the table below. For results based on other subgroups, the margin of sampling error may be higher. Sample sizes and margins of sampling error for other subgroups are available by request. Note that sampling error is only one of many potential sources of error in this or any other public opinion poll.
| Group | N (unweighted) | M.O.S.E |
| Men Ages 18-64 | 1,144 | +/- 4 percentage points |
| Women Ages 18-64 | 3,661 | +/- 2 percentage points |
| Women Ages 18-49 | 2,695 | +/- 2 percentage points |
| White Women Ages 18-64 | 1,813 | +/- 3 percentage points |
| Black Women Ages 18-64 | 603 | +/- 5 percentage points |
| Hispanic Women Ages 18-64 | 801 | +/- 5 percentage points |
| Asian Women Ages 18-64 | 246 | +/- 8 percentage points |
| LGB Women Ages 18-64 | 392 | +/- 7 percentage points |
| Heterosexual Women Ages 18-64 | 3,239 | +/- 2 percentage points |
| Women < 200% FPL | 1,471 | +/- 3 percentage points |
| Women ≥200% FPL | 1,943 | +/- 3 percentage points |