Consumer Problems with Prior Authorization: Evidence from KFF Survey
Introduction
A KFF survey of adults with health insurance found that roughly 6 in 10 insured adults experience problems when they use their insurance. Problems examined include denied claims, network adequacy issues, preauthorization delays and denials, and others. This Data Note takes a closer look at insured adults who said that in the past year, their health insurance denied or delayed prior approval for a treatment, service, visit or drug before they received it, which we will refer to as “prior authorization” problems. A separate Data Note looks at survey findings specific to the denial of health insurance claims.
Characteristics of consumers who experience prior authorization problems
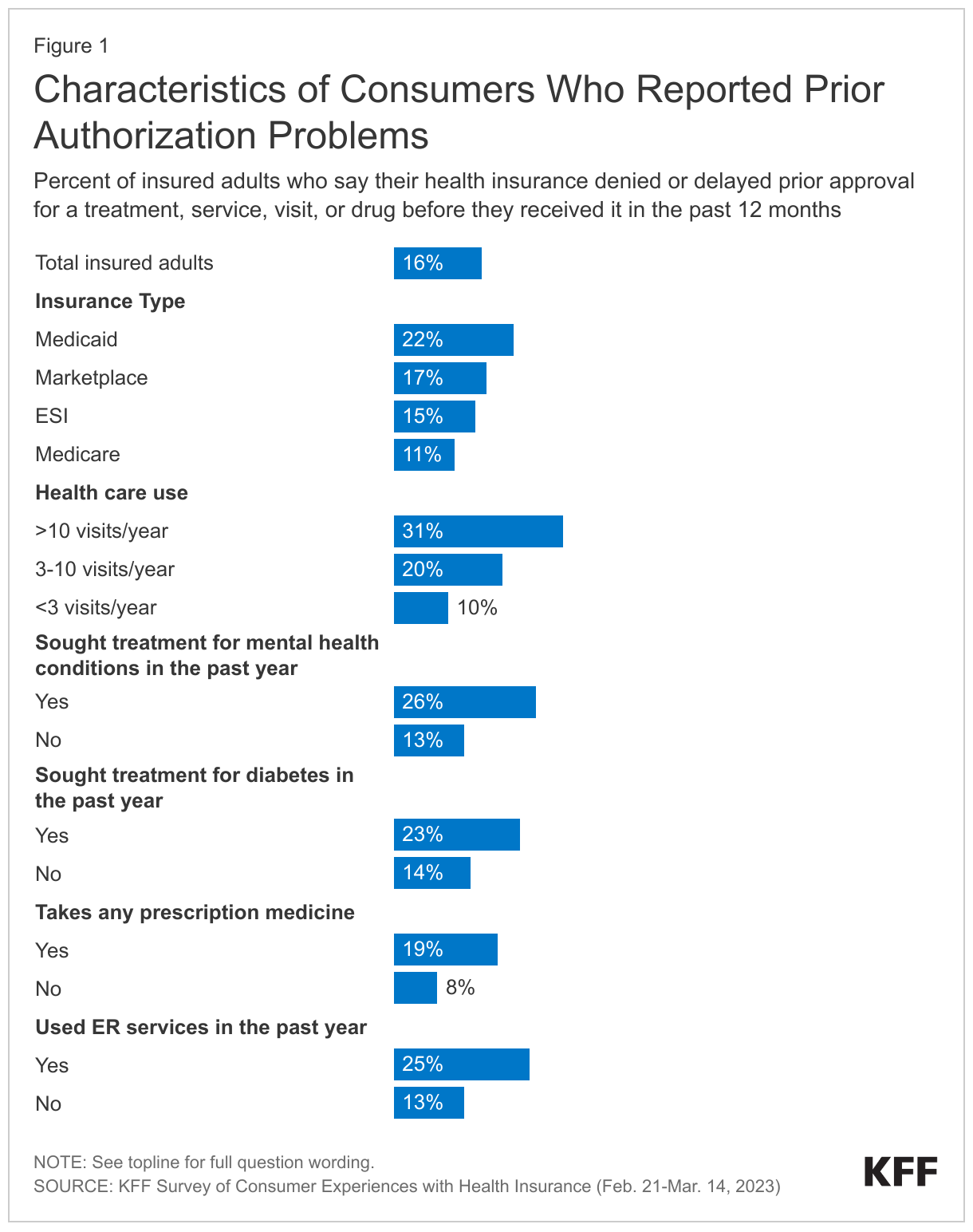
The survey found that 16% of all insured adults in the past year experienced prior authorization problems; and consumers with certain characteristics are more likely to encounter such problems:
Enrolled in Medicaid: About one in four (22%) adults insured under Medicaid experienced prior authorization problems in the past year, compared to 11% with Medicare, and 15% with employer sponsored coverage.
Use more health care services: Among adults who had more than 10 physician visits in the past year, 31% experienced prior authorization problems. This compares to smaller shares of moderate users of health services (3-10 visits) and low users (2 or fewer visits), who experienced prior authorization problems at rates of roughly 20% and 10%, respectively.
In addition, consumers with certain health conditions or who use certain types of health services are more likely to experience prior authorization problems; although importantly, survey data cannot identify whether prior authorization was applied specifically to these conditions and services:
Mental health conditions: 26% of people who sought treatment for or took prescription medication for a mental health condition in the past year (e.g., depression, anxiety) experienced prior authorization problems in the past year, compared to 13% of insured adults who did not seek mental health treatment.
Diabetes: 23% of insured adults who sought treatment or took prescription medication for diabetes experienced prior authorization problems in the past year, compared to 14% of other insured adults.
Prescription drugs: 19% of adults who currently take at least one prescription medication experienced prior authorization problems, compared to 8% of those who do not take prescription medication.
Emergency services: Insured adults who received health care in an emergency room in the past year were about twice as likely to have experienced prior authorization problems, compared to those who did not use the ER (25% vs. 13%). Federal law prohibits private plans from requiring prior authorization for emergency services.
Consumers with prior authorization problems tend to experience other insurance problems
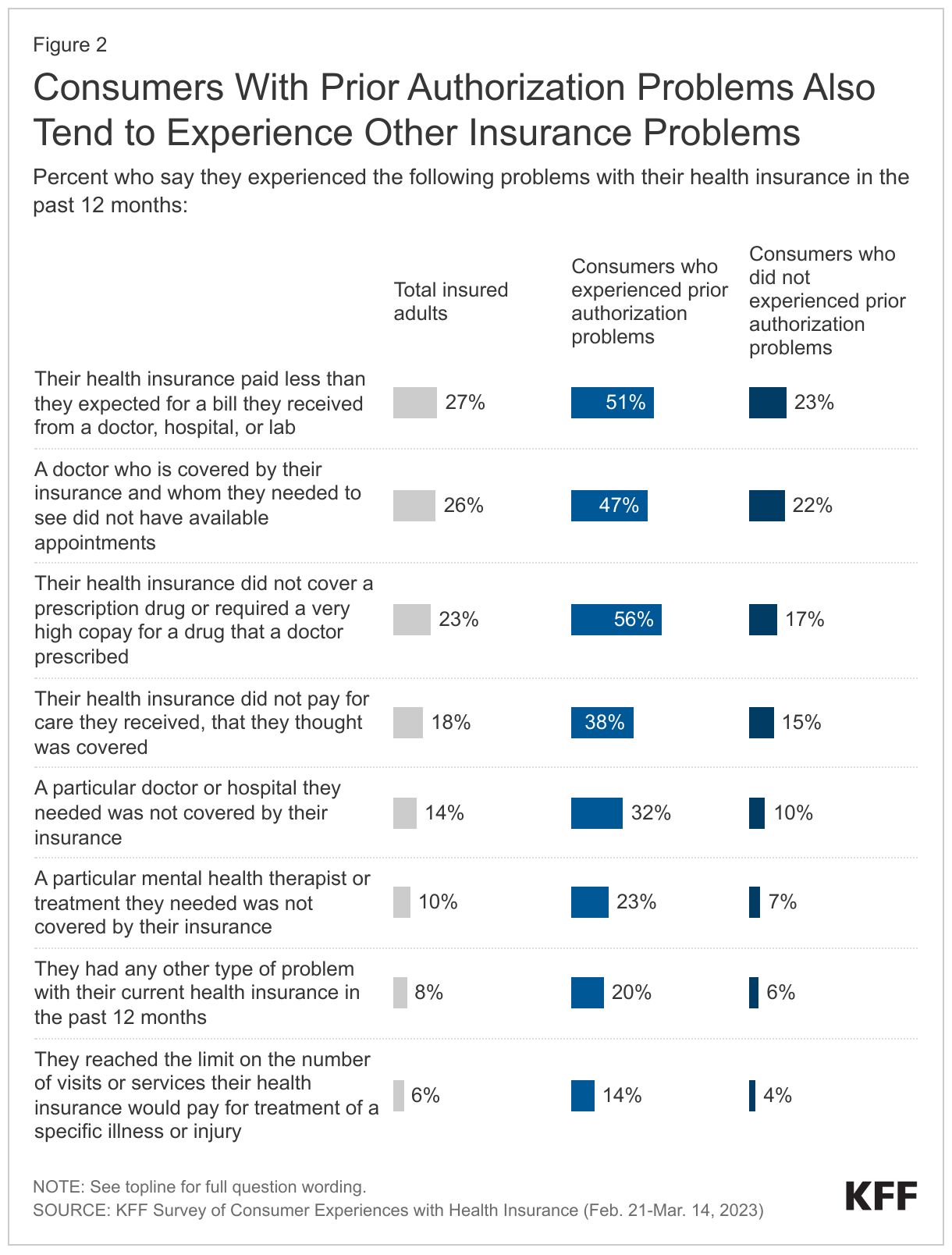
Consumers who experienced prior authorization problems were much more likely to have also encountered other problems using their coverage.
In addition to prior authorization, the survey asked about specific types of health insurance problems, such as reaching the limit on covered services, not being able to find or access an in-network provider, and denied claims. Insured adults overall said they experienced an average of 1.5 different types of insurance problems in the past year, while those who had prior authorization problems experienced about 4 different types of problems, on average. Only 9% of people with prior authorization problems said this was the only type of problem they experienced in the past 12 months.
Health and financial consequences when insurance problems include prior authorization
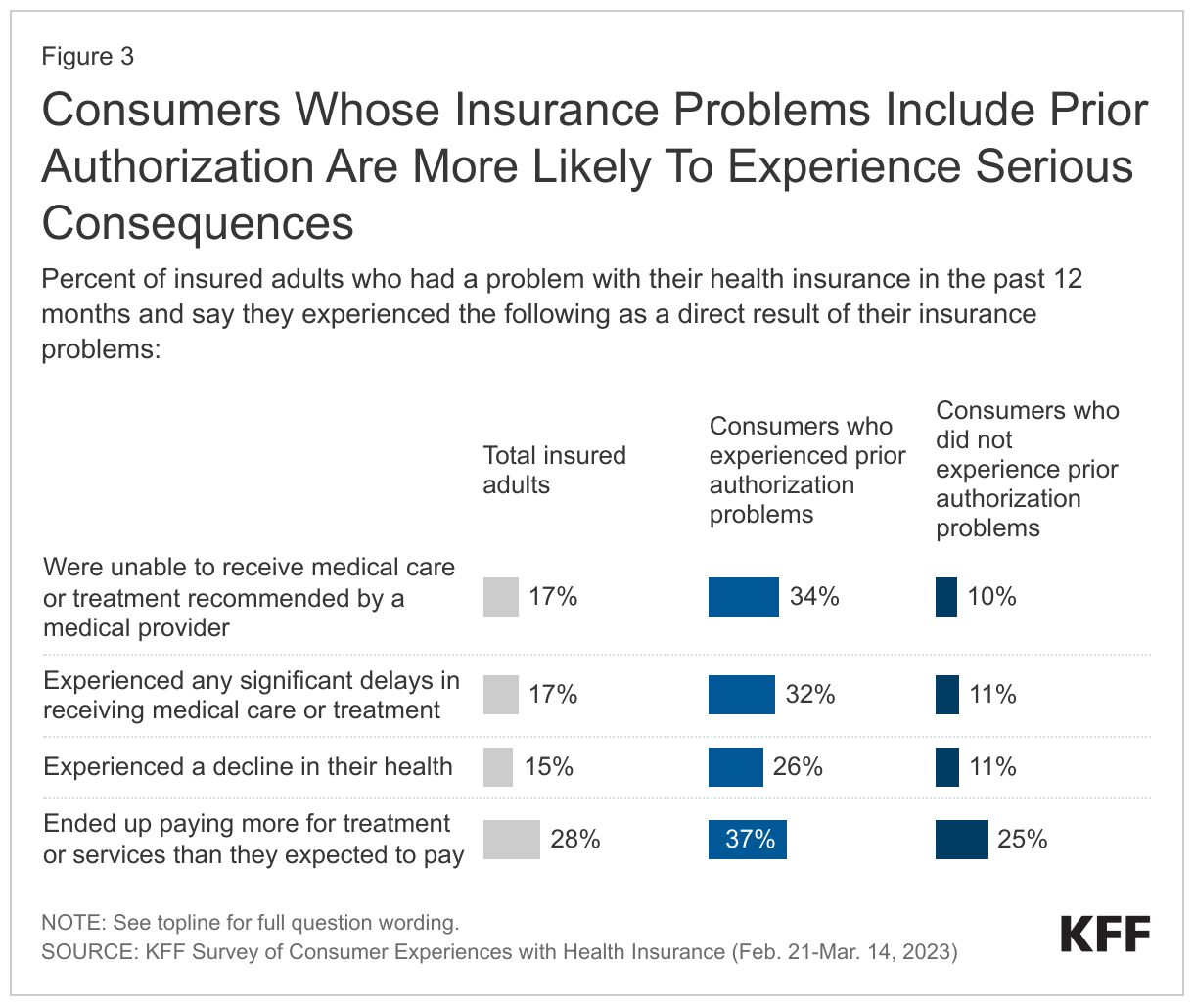
The survey asked people whether their insurance problems directly resulted in adverse outcomes such as delayed or denied access to needed care, a decline in health status, or having to pay higher out-of-pocket costs. Because people often reported experiencing multiple problems, the data cannot associate specific types of insurance problems with specific consequences. However, people whose problems included prior authorization were far more likely to experience serious health and financial consequences compared to people whose problems did not include prior authorization.
People whose problems include prior authorization were about 3 times more likely to report being unable to receive medical care or treatment recommended by a medical provider as a direct result of their health insurance problems compared to those whose problems did not include prior authorization (34% vs 10%), and about 3 times more likely to report significant delays in receiving medical care or treatment as a direct result of their problems (32% vs 11%). In addition, people whose problems included prior authorization were about twice as likely to say their health declined as a direct result. (26% v 11%). Finally, more than a third (37%) whose problems included prior authorization said they had to pay more out of pocket for care.
Discussion
Prior authorization is a tool intended to control spending and promote cost-effective care. While there is no way to tell from the survey whether or not prior authorization denials were clinically appropriate, one-quarter of adults whose insurance problems included prior authorization problems said their health status declined as a direct result of problems they had with their health insurance, while one-third said access to needed care was delayed or denied, and more than one-third said it resulted in higher out-of-pocket costs. Other studies indicate concerns about the use of prior authorization by health plans.
Survey results suggest that prior authorization problems are more prevalent among insured adults with certain characteristics. The more health services people use in a year, the more likely they are to encounter prior authorization problems. Such problems also are experienced disproportionately by people diagnosed with certain conditions, including about 1 in 4 insured adults who sought treatment for diabetes (23%) and mental health disorders (26%). Prior authorization problems also arise more often among people who use certain services, including emergency services (25%) and prescription drugs (19%). Importantly, the survey data do not identify which services or conditions were the subject of prior authorization requirements.
Current law authorizes federal regulators to collect from private health plans and make publicly available data on which services are subject to prior authorization and how often it is granted or denied. However, this law remains largely unimplemented, with only partial data on certain in-network services collected from some Affordable Care Act marketplace plans. Recent proposed federal regulations related to compliance with the Mental Health Parity and Addition Equity Act (MHPAEA) would require private health plans to internally collect and evaluate data on whether certain practices, including prior authorization requirements, are being used comparably for behavioral health and medical/surgical benefits. Such data would not be readily transparent to the public as plans would only be required to report data or results to the Secretary or to certain plan beneficiaries upon request.
With respect to public coverage, Medicare enrollees experience the lowest rate of prior authorization problems (11%). However, a recent Inspector General audit of this practice in Medicare Advantage (MA) plans found 13% of prior authorization denials were for benefits that should otherwise have been covered under Medicare. (Traditional Medicare generally does not use prior authorization). The Inspector General recommended Medicare should take a closer look at the appropriateness of criteria used by MA plans in making coverage determinations. This year CMS finalized new standards for prior authorization and coverage decisions in Medicare Advantage plans.
Nearly one in four adults insured under the Medicaid program say they experienced a prior authorization problem (22%). A recent report by the Inspector General of the Department of Health and Human Services reviewed data on more than 17 million prior authorization request to Medicaid managed care organizations (MCOs) and found more than 2 million had been denied. It also found substantial variation in denial rates across parent firms of MCOs, ranging from 7% to 41%. The IG recommended stronger state monitoring of denials and automatic external medical reviews when such denials are appealed (which happens infrequently). The Biden Administration has proposed new regulations around prior authorization that would apply to Medicaid and other coverage types. These rules focus mostly on streamlining processes and reducing approval wait times and have not yet been finalized.
A range of state regulatory actions have also focused on prior authorization practices. New state laws or updates to existing ones have passed in states such as Georgia, Illinois, Washington state, Arkansas and Texas. State requirements include: new reporting on prior authorization standards and claims denials, shortened time frames for decision-making, allowing providers to bypass prior authorization to limit delays (e.g. “gold carding”), and restrictions on the use of clinical criteria developed by insurers to make coverage decisions. While states have the authority to regulate insured plans purchased by employers or individuals, they lack authority to regulate self-insured employer plans, which cover the majority of those with health benefits through a job.
This work was supported in part by a grant from the Robert Wood Johnson Foundation. The views and analysis contained here do not necessarily reflect the views of the Foundation. KFF maintains full editorial control over all of its policy analysis, polling, and journalism activities.