Nursing Facility Staffing Shortages During the COVID-19 Pandemic
The disproportionate impact of the COVID-19 pandemic on nursing facility residents and staff has brought increased attention to long-standing workforce issues that can affect care quality and safety, such as staffing shortages and high turnover rates. These issues have existed for decades and have been associated with adverse outcomes, including increased mortality rates, hospitalization rates, and emergency department visits. In a recent KFF poll, a majority (70%) of adults said that this country’s nursing facilities and other long-term facilities are doing a “bad job” of maintaining adequate staffing levels.
Since the onset of the pandemic, more than 200,000 COVID-19 deaths have occurred among long-term care residents and staff, with most of these deaths (150,000 COVID-19 deaths) occurring among residents and staff in nursing facilities that are certified to receive Medicare and/or Medicaid payments. In response to these issues, the Biden Administration recently announced a set of nursing facility reforms, which were highlighted in the State of the Union address.
This analysis presents the most recent national and state-level data on nursing facility-reported staff shortages and describes the Biden Administration’s new policy initiatives to address staffing and other quality issues in nursing facilities. National staff shortage trend data spans from May 2020, the first month when nursing facilities were required to report COVID-19 facility data to the CDC, through March 20, 2022, the most recent week of data available. See the Methods box below for more details.
1. What do the data show about nursing facility staffing?
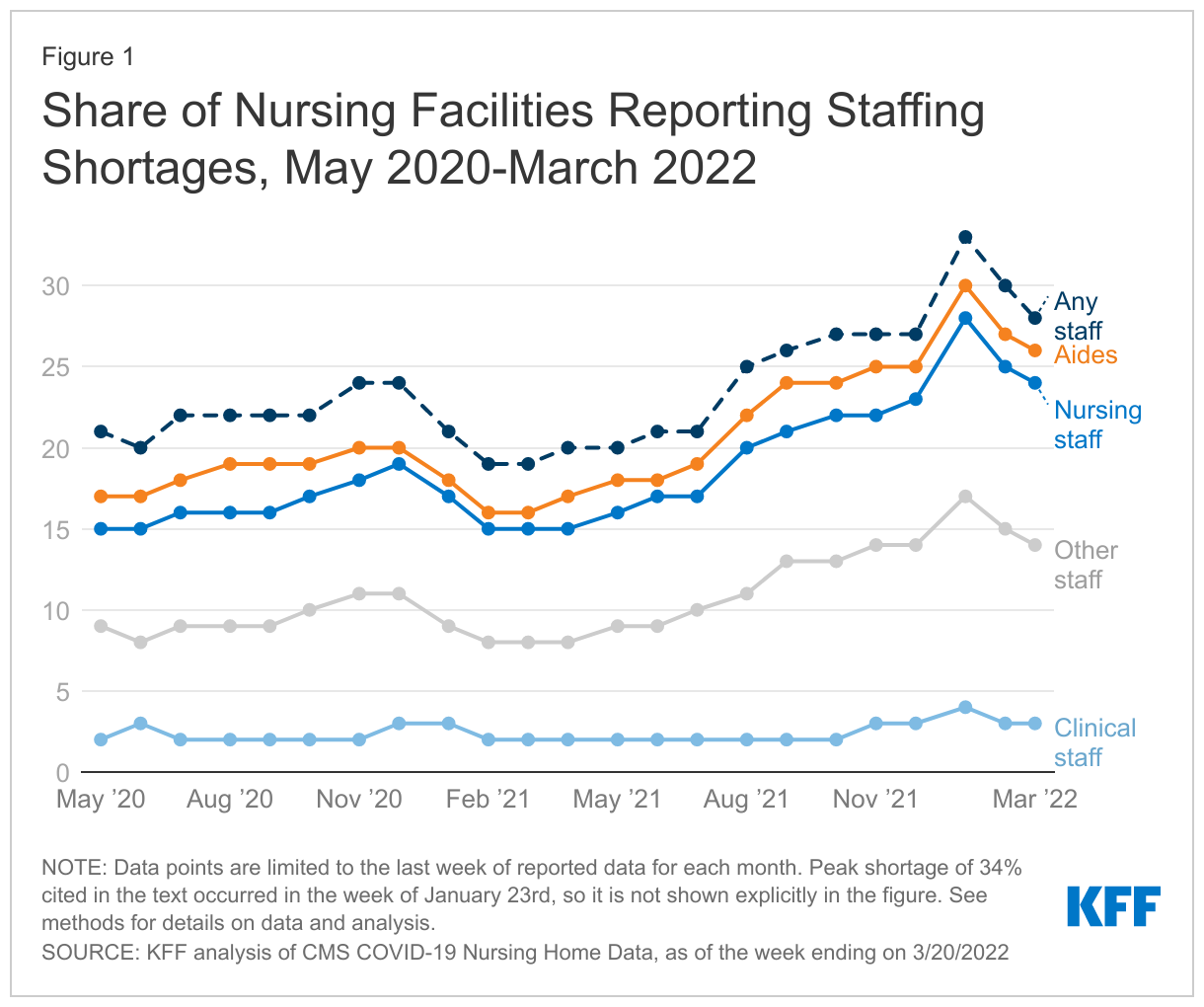
As of the week ending March 20, 2022, the most recent data available, 28% of nursing facilities reported at least one staffing shortage (approximately 3,900 out of 14,000 facilities) (Figure 1). The current rate represents a slight drop since the week ending January 23, 2022, when the share of nursing facilities reporting a staff shortage peaked at 34%. This slight decline between January and March may be partly due to the decline in cases related to the Omicron variant as well as other potential factors, including anecdotal accounts of nursing facilities offering higher wages to attract workers. The current rate, 28%, is higher than the rate reported in May 2020, when 21% of nursing facilities reported at least one type of staff shortage.
The current level of staff shortages coincides with a period when health care providers, including nursing facilities, grappled with the impact of the Omicron variant, a highly transmissible variant that broke case and hospitalization records. This variant primarily affected residents and staff who were not vaccinated or boosted, though vaccinated older adults and those with other health conditions still faced a high risk of infection and mortality.
Nursing facilities were most likely to report a shortage of aides and least likely to report a shortage of clinical staff as of March 20, 2022. (Figure 1). Among the approximately 14,000 nursing facilities reporting complete and reliable data for the week ending March 20th, 26% reported aide shortages while just 3% reported clinical staff shortages. Staff shortages were nearly as high for nursing staff as they were for aides, with 24% of facilities reporting nursing staff shortages. In the same time period, 14% reported other staff shortages. These patterns have held steady since nursing facilities began reporting this data in May 2020. For purposes of reporting staff shortages, the Centers for Medicare & Medicaid Services (CMS) defines aides to include certified nursing assistants (CNAs), nurse aides, and medication aides or technicians. Aides typically oversee overall care needs, including assistance with personal care needs and ensuring that each resident’s plan of care is being followed. Clinical staff primarily oversee medical needs and include physicians, physician assistants, and advanced practice nurses. Nursing staff include registered nurses, licensed practical nurses, and vocational nurses.
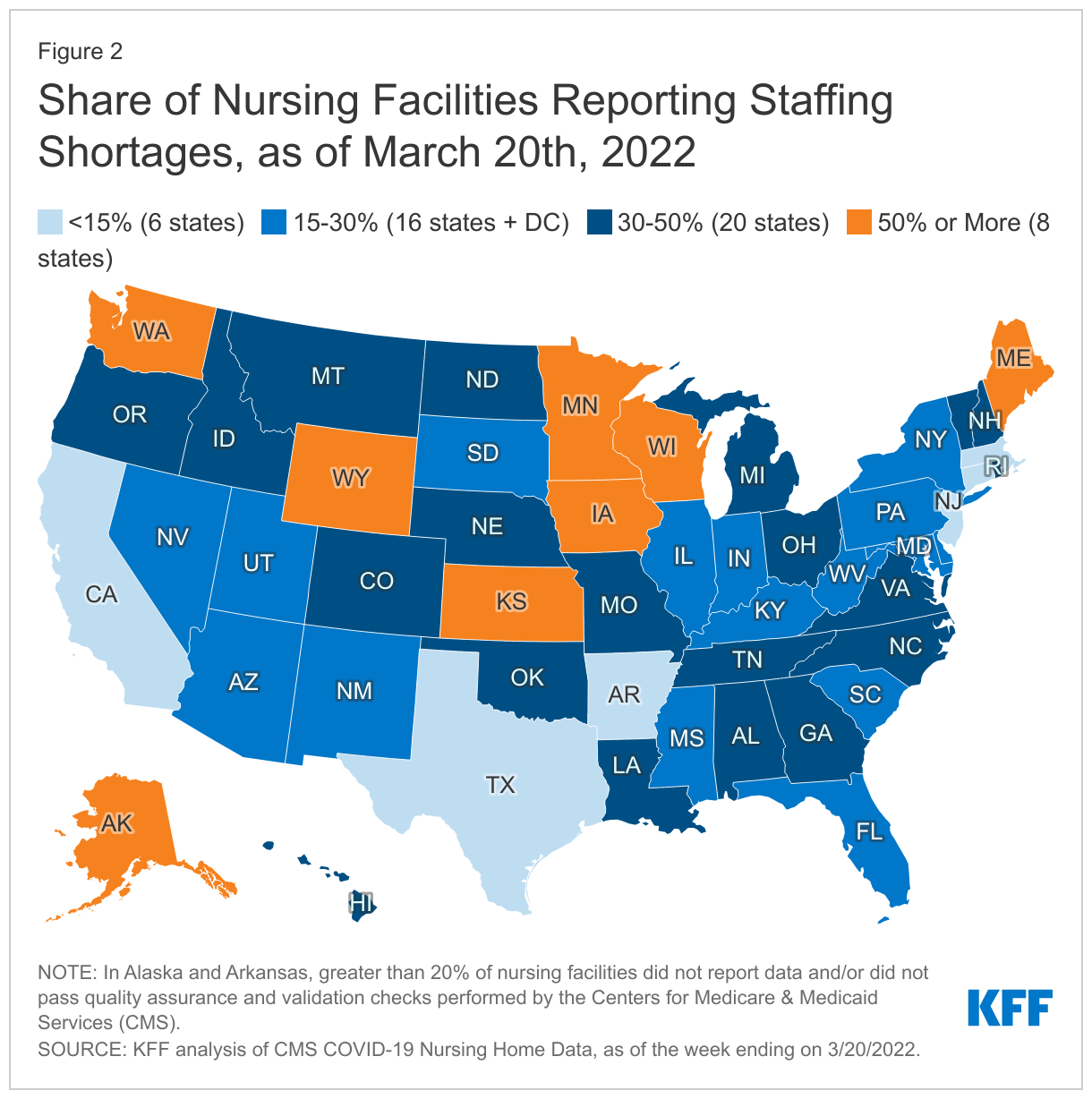
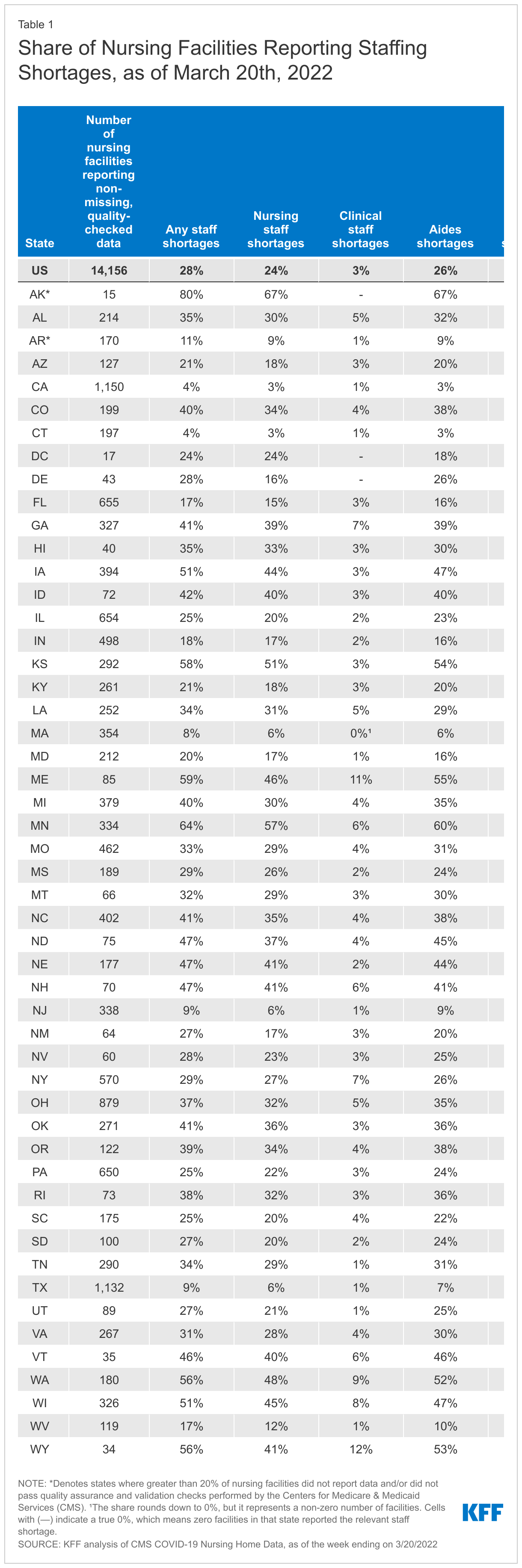
The share of nursing facilities reporting staffing shortages varies widely by state (Figure 2 and Table 1). As of the week ending March 20, 2022, the share of nursing facilities reporting staff shortages ranged from 4% of nursing facilities in Connecticut and California to 80% in Alaska (Figure 2, Table 1). Of note, less than 80% of nursing facilities in Alaska reported data and passed quality-checks performed by CMS.
In eight states, at least half of nursing facilities reported one or more staff shortage as of March 20, 2022. The five states with the highest shares of nursing facilities reporting any staffing shortages include Alaska (80%), Minnesota (64%), Maine (59%), Kansas (58%), and Wyoming (56%). Conversely, the five states with the lowest share of nursing facilities reporting staff shortages include California (4%), Connecticut (4%), Massachusetts (8%), Texas (9%), and New Jersey (9%) (Table 1). State variation in staffing shortages at the facility-level may be attributable to variation in local economies and labor markets, and could also be due to differences in the way in which nursing facilities define staff shortages.
2. What new policies did the Biden Administration announce?
The Biden Administration’s new initiatives are focused on improving care quality, nursing facility oversight, data transparency, career pathways, and pandemic and emergency preparedness. Key policy proposals include establishing minimum staffing levels for Medicare and Medicaid-certified nursing facilities, strengthening oversight of poor-performing nursing facilities, supporting state efforts to tie Medicaid reimbursement rates to increases in staff compensation, and launching a national nursing career pathways campaign to recruit, train, and retain long-term care staff, among others. While some of the new policies can be adopted by the Administration, others would require Congressional action.
The Biden Administration plans to propose new regulations that would establish a minimum nursing facility staffing requirement within the next year. The fact sheet announcing this new proposal highlights adequate staffing levels as the “measure most closely linked to the quality of care residents receive.” The fact sheet cites a study of Connecticut nursing facilities, which found that an increase in registered nurse staffing of 20 minutes per resident day was associated with 22 percent fewer confirmed COVID-19 cases and 26 percent fewer COVID-19 deaths. Before proposing new regulations, CMS will conduct a new study to “determine the level and type of staffing needed to ensure safe and quality care.” Policymakers and other stakeholders have debated issues about care quality and staffing levels ever since federal requirements for nursing facilities to receive Medicare and Medicaid funds were established. The 1987 Nursing Home Reform Act adopted the current federal requirement that facilities provide 24-hour licensed nursing services “sufficient to meet resident needs,” including registered nurse services at least eight consecutive hours per day. However, there are no other federal requirements for minimum staffing hours per resident day, and staffing levels and their impact on care quality remain a topic of recurring concern among government regulators and other stakeholders. While these proposed Biden reforms could take place administratively, some policy changes can be done via legislation. Provisions in the Build Back Better Act (BBBA) passed by the U.S. House of Representatives would have required HHS to conduct regular studies and report to Congress on the appropriateness of establishing minimum staffing ratios in nursing homes and to specify any appropriate minimum ratios for nurses and aides in regulations. However, whether the BBBA advances in the Senate remains uncertain.
3. What issues are important to watch?
Looking ahead, open questions remain about how and when the new Biden policy proposals will be implemented. The specific details about what minimum staff levels will be proposed are not yet known, and as noted above, CMS intends to conduct a study to inform the new proposed regulations. While the Administration plans to issue proposed rules within a year, it is not yet known when the new rules would be finalized or take effect. Enforcement of the new rules will likely be through the existing state inspection process, with facilities potentially subject to penalties such as fines or loss of Medicare or Medicaid funding. Another open question is how stakeholder reaction will affect the new rules. The proposal faces stiff opposition from the nursing home industry, which argues that facilities will be unable to meet new staffing and oversight requirements without additional federal funding. Proponents of the new rules contend that minimum staffing requirements are an important protection for nursing home residents. Others argue that the Biden proposal does not go far enough and should also address issues around Medicaid reimbursement rates and worker compensation. It is not clear whether Congress will authorize additional federal funding beyond the pandemic relief funds already provided for nursing facilities.
Another open question is how the pandemic and CMS’s health care provider vaccination mandate will affect nursing facility staffing shortages. When issuing the mandate, CMS acknowledged that some staff may leave their jobs because they do not want to receive the vaccine, but cited examples of vaccine mandates adopted by health systems in Texas and Detroit and a long-term care parent corporation with 250 facilities as well as the New York state health care worker mandate, all of which resulted in high rates of compliance and few employee resignations. Staff vaccination rates currently vary by state, likely reflecting a mix of federal mandate deadlines not yet passing, varying state and/or local mandates, and different degrees of vaccine hesitancy among staff. Data also show that the number of workers in nursing care and elder care facilities has continued to decline even while other health settings have returned to nearly pre-pandemic levels, raising questions about the long-term effects of the pandemic on the workforce. Forthcoming KFF analyses will analyze the impact of the mandate when data is available, as well as evaluate state minimum staffing requirement changes post-COVID. It will be important to watch whether and how lessons from the pandemic are integrated into new policies to improve nursing facility care quality and protect residents and staff.
Methods
This analysis uses federal data on staffing reported weekly by facilities to the CDC’s National Healthcare Safety Network (NHSN) and reflects data from mid-May 2020 through March 20, 2022. These data are updated regularly to reflect revised data from previous weeks, so future versions of this dataset reflecting the same time period may output different values.
Each week, approximately 15,200 nursing facilities submit data through NHSN, including whether they are experiencing a shortage in nursing staff (including registered nurses, licensed practical nurses, and vocational nurses), clinical staff (including physicians, physician assistants, and advanced practice nurses), aides (including certified nursing assistants, nurse aides, medication aides, and medication technicians), or other staff (including administrative, custodial, and other environmental service staff). These measures are asked and reported as binary measures (yes/no) and reflect staffing shortages as of the week of data reporting; therefore, we are unable to determine the magnitude of staffing shortages among nursing facilities that report “yes” to one or more staff positions. Additionally, these measures differ from other measures of staffing sufficiency, including the minimum staffing levels required by the federal government and states.
CMS performs data quality checks to identify facilities that may have entered incorrect data before publishing this data for public download. Facilities that have submitted erroneous data will have an “N” displayed in the column titled “Passed Quality Assurance Check”. Our final sample of nursing facilities in this analysis excludes facilities that CMS flagged in their data quality check, as well as facilities that are missing shortage measures. With these exclusions, each week of data in Figure 1 represents anywhere from 14,100 to 15,100 facilities. Each week of data represents a slightly different set of facilities due to weekly variation in nursing facility reporting. The most recent week of data, as of March 20, 2022, includes 14,156 nursing facilities. The federal data includes only data on Medicare or Medicaid certified nursing facilities. This analysis therefore does not reflect other long-term care settings, such as assisted living facilities, residential care facilities, group homes, or intermediate care facilities.