Continued Rises in Extreme Heat and Implications for Health Disparities
Climate change-related extreme heat events have lengthened, become more frequent, and increased in intensity over the past few decades with some of the worst conditions and impacts observed in Summer 2023. Across the globe and the country there have been rising incidents of extreme heat, and air quality events. June 2023 became the hottest June on record, globally, while smoke from wildfires in Canada driven by climate change-related heat resulted in significant air pollution that affected more than 60 million people in the U.S. In August, prolonged dry conditions and high winds in Hawai’i laid the foundation for wildfires that caused massive destruction on the island of Maui and other areas of the islands, resulting in the largest loss of life due to wildfires in modern U.S. history. As temperatures continue to rise and extreme heat events that are linked to adverse health outcomes become more frequent in the U.S., people of color and other underserved communities are disproportionately affected.
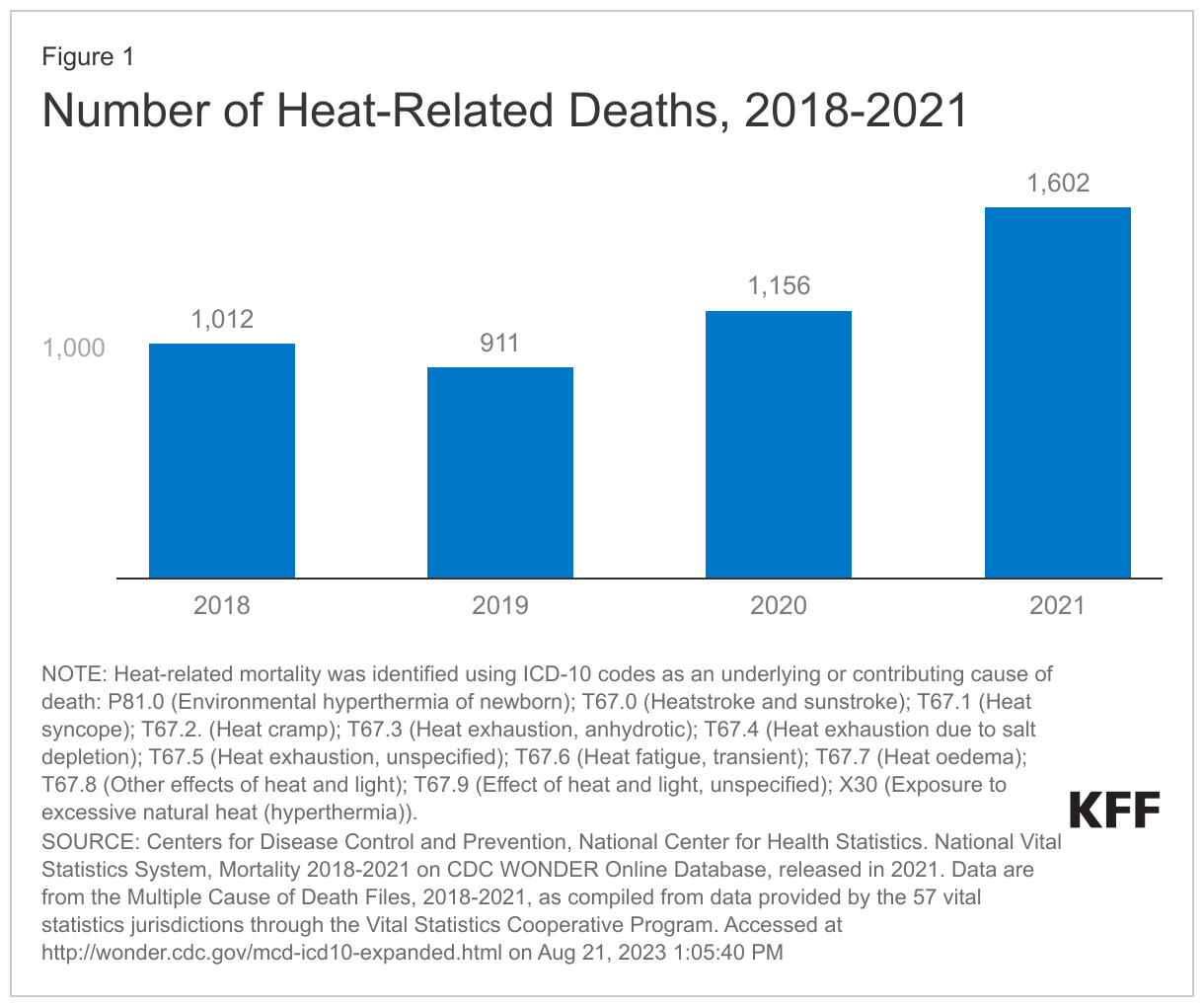
Extreme heat can have serious health impacts, including death. According to the Community Resilience Estimates (CRE) for Heat tool developed by the U.S. Census Bureau and Arizona State University, which accounts for factors such as housing quality, transportation exposure, and financial hardship, nearly a quarter of people in the U.S. are socially vulnerable if exposed to extreme heat. Extreme heat is the leading cause of weather-related deaths, killing more people in the U.S. than any other weather phenomenon. According to mortality data from the Centers for Disease Control and Prevention, between 2018 and 2021, there were a total of 4,681 heat-related deaths, with the number of deaths rising each year from 2019 onward (Figure 1). However, studies suggest that this is likely a vast undercount, and other evidence shows that extreme heat is associated with higher all-cause mortality. One estimate pegs the cost of heat events in the U.S. at approximately $1 billion in excess health care costs each year and, if unaddressed, could cost the U.S. economy approximately $14.5 trillion over the next fifty years.
While extreme heat and other climate-related weather events have implications for everyone, they disproportionately affect historically marginalized groups who are at higher risk for dying from heat exposure. Recent literature shows that within the U.S., some communities of color have higher risks of heat-related mortality than White people. Consistent with trends in earlier years, between 2018-2021, AIAN people were most likely to die due to heat compared to all other racial and ethnic groups, and Black people had a higher rate of heat-related deaths compared to White people. The rate for Hispanic people was similar to that of White people, while Asian people had a lower rate of heat-related death (Table 1). Data also show that noncitizens are more likely to die from heat exposure compared with citizens.
These higher mortality risks reflect increased exposure to heat due to underlying inequities. Due to historically-codified residential segregation in the U.S. including “redlining,” on average, people of color have a higher likelihood of living in a census tract with higher summer daytime surface urban heat island intensity compared to their White counterparts. Low income communities and communities of color also suffer from tree inequity, increasing the risk of exposure to extreme heat and subsequent heat-related illnesses. Communities that live in these historically zoned areas are also more likely to have higher rates of asthma and cardiovascular illnesses and other diseases that increase their risk of poor health outcomes associated with exposure to climate change-related extreme heat and air pollution. The Southern U.S. and some areas in the Northeast and Midwest have experienced the greatest increases in the number of heat wave days in the U.S., which may have equity implications because these affected areas include higher shares of people of color, and are therefore more likely to be exposed to longer and more intense heat waves. Projections suggest that disparities in extreme heat exposure will continue to persist thirty years from now.
More limited access to air conditioning also contributes to disproportionate exposure to extreme heat and heat-related illnesses. Low-income households, which include disproportionate shares of people of color, face affordability challenges to accessing air conditioning. Lack of air conditioning increases risk of negative health outcomes including death due to heat exposure. Rising temperatures have been associated with increases in mortality among incarcerated people, a population in which people of color are overrepresented, and that sometimes has more limited access to air conditioning. The 2023 Texas heat wave highlighted the impact of lack of air conditioning in prisons. Approximately 13% of deaths in Texas prisons during warm months between 2001 and 2019 were associated with extreme heat in unairconditioned prisons. Further, as temperatures continue to rise, U.S. power grids may be unable to support the surges in energy use due to increase air conditioning and cooling infrastructure usage during heat waves and other extreme weather events.
People of color, noncitizen immigrants, and people with low incomes are more likely to work in jobs with climate-related health risks, including heat. Heat is a top cause of exertion-related occupational injuries and deaths. Workers at risk of heat stress include outdoor workers and workers in hot environments, such as construction workers, agricultural workers, factory workers, firefighters, among others. Migrant or immigrant workers make up significant proportions of farmworkers and are disproportionately exposed to environmental hazards, including heat.
The Occupational Safety and Health Administration (OSHA) and the Center for Disease Control and Prevention have heat stress prevention recommendations, but there currently are no national standards in place to protect workers from exposure to extreme heat. In 2021, OSHA issued a proposed rulemaking to protect workers from extreme heat exposure and heat stress in indoor and outdoor settings by seeking information on issues that may be considered in developing a standard. Since then, OHSA has established an enforcement initiative on heat-related hazards and created a National Advisory Committee to better understand challenges and identify and share best practices to protect workers. However, to date, a standard has not been established. As of Summer 2023, OSHA is seeking feedback from small businesses and local governments on the potential impact of a workplace heat standard on small businesses. Five states currently have occupational heat protection standards. In contrast, Texas Governor Gregg Abbott signed House Bill 2127 that limited local governments’ abilities to regulate work breaks. The law is expected to overturn local ordinances that mandate regular water breaks for workers, including construction workers who are disproportionately exposed to extreme heat
As extreme heat continues to worsen, strategies to mitigate exposure and reduce health risk will be of increasing importance. The Biden Administration has taken some steps to increase awareness and understanding of heat exposure and health risks, including launching a new heat.gov website, and plans to develop a National Heat Strategy. The newly established Office of Climate Change and Health Equity within the Department of Health and Human services aims to address the impact of climate change on health and is developing new tools to help track heat-related illnesses. Other agencies have taken steps to educate individuals and communities about how to protect themselves from extreme heat and to develop more climate-resilient communities. Ongoing efforts to address rising temperatures, reduce risks of heat exposure, and increase protections for those most at-risk for heat exposure will be important for reducing negative health impacts due to extreme heat particularly for groups who already face disparities in health.