External Review of Health Plan Decisions in the States and Medicare – Report
External Review of Health Plan Decisions:An Overview of Key Program Features in the States and Medicare

External Review of Health Plan Decisions:An Overview of Key Program Features in the States and Medicare
Prepared for the Kaiser Family Foundation by:Karen Pollitz, M.P.P., Geraldine Dallek, M.P.H., and Nicole Tapay, J.D.Institute for Health Care Research and Policy, Georgetown University
Executive Summary
In 1978, the state of Michigan established a system to call on independent medical experts to help resolve disputes between health plans and patients about the medical necessity and appropriateness of care. Since then, twelve other states and the Medicare program have established similar kinds of external review programs. In the first half of 1998, five more states enacted external review laws (and two states passed laws modifying or expanding existing programs).
The term “external review” means different things to different people. In this paper, “external review” refers to a formal dispute resolution process, established by a state or federal agency to be independent of disputing parties, that has the capacity to evaluate and resolve at least those disputes involving medical issues. State health plan regulators have other responsibilities that are sometimes characterized as external review. For example, virtually all state insurance departments, and many state health departments, accept, investigate and help resolve consumer complaints about their health plans regarding marketing behavior, premiums, and contractual terms of coverage and exclusion of benefits. However, these complaint resolution processes were not included in this study unless they also incorporate a formal process for resolving disputes over medical issues.
Using this definition, this research identified and studied external review programs in thirteen states and in the Medicare program. Medicare’s external review system, established in 1989, is one of the oldest-behind Michigan (1978) and Florida (1985). Unlike state programs, which require consumers to affirmatively request an appeal, Medicare requires that all denials upheld by the health plan’s internal review process must automatically be forwarded for external review. Only in three states and Medicare are external review systems set up to resolve all types of consumer disputes – whether or not they involve clinical issues. The other ten study states have established a separate external review process for disputes involving issues of medical necessity or appropriateness; other disputes not about clinical issues must be pursued through a different process. Based on a review of these programs and interviews of experts involved with them, this paper identifies critical features of external review systems and how they vary. (See Table 1.) State and federal policymakers contemplating creation of new external review requirements may benefit from the lessons learned by the states and Medicare.
Major Findings
Consumers seek external review of health plan decisions on a wide range of health care services based on issues that are medical, legal, or both. Disputes arise in all types of health plans, over denials of health services ranging from routine to life-saving. (See Table 1, Scope of External Review.) Such denials might be justified on the grounds that services are not medically necessary or appropriate. Or, they might be denied based on other coverage limitations in the health plan contract. Some external review programs hear all types of disputes. Experts from these programs believe their broad scope affords consumers the most comprehensive protection. Other external review programs limit their scope only to disputes over medical issues. Experts from these programs acknowledge that it can be difficult to disentangle clinical issues from other contractual and coverage issues in some cases. State programs that try to separate disputes by type tend to rely on regulatory staff experts to distinguish cases and steer non-clinical issues to other appropriate forums for resolution.
The types of cases for which consumers seek external review are varied and often complex. For example, Rhode Island reviews a significant number of mental health and substance abuse cases relating to the need for inpatient services. In Texas, the largest number of cases has been for pain management and substance abuse treatment, followed by oncology cases. Approximately half of the prospective review cases in Texas have been for “life-threatening” conditions. Cases reaching external review in Missouri included questions of whether speech therapy is restorative, whether hysterectomy or hormone therapy is appropriate treatment, whether a heart bypass surgery patient should receive cardiac rehabilitation, and whether therapy following knee surgery was medically necessary. Consumers also seek external review of health plan decisions involving less expensive care. For example, 20 percent of Medicare’s external reviews in 1997 involved denials of medical equipment and supplies, averaging $124 per case.
External review upholds health plan decisions about as frequently as it overturns them. The disposition of cases under external review splits fairly evenly. Across all programs studied, external review overturned health plan decisions between 32 and 68 percent of the time (See Table 1, No. and Disposition of Cases.)
Consumers seek external review infrequently; certain program features may further limit the use of external review. To date, the volume of cases under external review programs is small. In Medicare, external review is performed at a rate of about two cases per 1,000 managed care enrollees per year. (See Figure 1.)
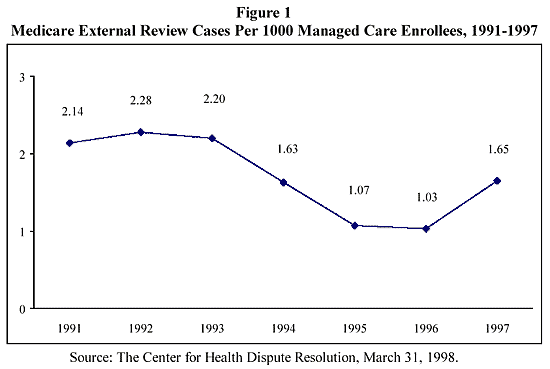
By contrast, even in large states with long-established external programs, external reviews are performed at a rate that is only a tiny fraction of Medicare’s. In Pennsylvania, for example, the external review rate in 1997 was less than 0.04 cases per 1,000 enrollees-less than one-fortieth the rate in Medicare in the same year. In several states, the rate is much lower than had been predicted at the program’s outset. Rates of external review per covered enrollees are not presented for all the study states because the scope of external review programs varies and not all health plan regulators were able to provide estimates of the number of consumers covered by their programs. However, the volume of cases in states is uniformly low – less than 250 cases per year in the largest states and even fewer in smaller states. For three states whose scope of external review is similar, Michigan had 49 cases from 1995 through June 1998, Florida had 403 cases from 1993 through April 1998, and Pennsylvania had 729 complaints from 1991 through June 1998. (See Table 1, No. and Disposition of Cases.)
Managed care industry representatives suggested that the small number of cases reflects the generally high quality of care provided by plans and the effectiveness of their internal appeals systems in resolving consumer disputes. However, several state regulators expressed concern over the infrequent use of external review. They cited lack of consumer awareness as a principal reason, followed by the burden of illness, which may prevent consumers from pursuing external review. Some states are exploring new strategies for consumer outreach to expand awareness of external review protections. In Medicare, consumers do not have to request external review. It is automatic for all denials upheld by a managed care plan’s internal review process.
Some state external review programs include features that were designed to deter frivolous cases or otherwise keep caseloads manageable – application fees, limits on the types and/or size of claims eligible for review, and imposition of filing deadlines, after which external review is no longer available. However, appeals volumes have been small and the problem of frivolous appeals has not materialized in states, with or without these features. While some health plan regulators did not view these features as impeding consumer access, others expressed concern that they might do so.
This report is also available in PDF format.
The Kaiser Family Foundation is an independent health care foundation and is not affiliated with Kaiser Permanente or Kaiser Industries.
External Review of Health Plan Decisions: An Overview of Key Program Features in the States and Medicare
Fact Sheet Part 1 Part 2 Library Index