Challenges in the U.S. Territories: COVID-19 and the Medicaid Financing Cliff
Issue Brief
More than a year into the public health emergency, the COVID-19 pandemic continues to impact the lives of Americans including those living in the U.S. territories. Prior to the pandemic, the U.S territories – American Samoa, the Commonwealth of the Northern Mariana Islands (CNMI), Guam, Puerto Rico, and the U.S. Virgin Islands (USVI) – faced an array of longstanding fiscal and health challenges that were exacerbated by recent natural disasters. Differences in Medicaid financing, including a statutory cap and match rate, have contributed to broader fiscal and health systems challenges for the territories. While additional federal funds have been provided over the statutory caps, these funds are set to expire at the end of September 2021. Without additional Congressional action, the territories will lose the vast majority of Medicaid financing which could result in reductions in coverage, services, and provider rates which could negatively impact the territories as they deal with the long-term health and economic consequences of the pandemic. This brief looks at how the pandemic is affecting the territories as well as issues related to the upcoming Medicaid fiscal cliff.
Health Status and Systems in the Territories Pre-Pandemic
Even prior to the pandemic, residents of the U.S territories experienced a range of health disparities compared to the states. For example, Puerto Rico and the U.S. Virgin Islands (USVI) both have higher rates of diabetes1 when compared to the United States overall. American Samoa, the Commonwealth of the Northern Mariana Islands (CNMI), and Guam have higher rates of obesity,2 high blood pressure,3 and smoking (respectively) when compared to the United States overall.
Additionally, the health care systems in U.S. territories have faced longstanding challenges, including deferred repairs to hospital facilities4 and major provider shortage issues. Recruitment and retainment is difficult as salaries for providers in the territories are substantially lower than they are for providers in the U.S. even though providers in most territories must be U.S.-licensed.5 Constraints with providers as well as system capacity sometimes requires that patients get care off-island.6 For example, prior to building its own oncology center on-island, CNMI sent over 300 patients a year to Guam or Hawaii for care.7
These health care system challenges were greatly exacerbated by recent natural disasters that occurred pre-pandemic. Typhoons, earthquakes, mudslides, and volcanic eruptions throughout the territories have caused extensive damage to hospital facilities, increased rates of provider outmigration, and increased the overall number of patients and the number of patients with more complex mental and physical health needs.
Effect of COVID-19 and Vaccine Roll-Out in the Territories
Early in the pandemic, the U.S. territories struggled with COVID-19 testing limitations and therefore COVID-19 cases and deaths may be underreported. In March 2020, only Guam and Puerto Rico were able to perform COVID-19 testing in their public labs but faced limited capacity due to supplies and staff.8 The other three territories had to send their testing samples to Hawaii or to the mainland – leading to longer turnaround time for results – until they acquired their own testing and analysis equipment.9 While Puerto Rico did have public labs to perform testing, in the spring of 2020, it had the lowest per-capita testing rates10 compared to any state and struggled to obtain the necessary supplies in order to increase its testing capacity.11 Guam, on the other hand, lacked staffing to administer tests.12
The pandemic exposed pre-pandemic health system issues that remained after the natural disasters. With the surge in COVID-19 cases, most territories reached hospital and ventilator capacity quickly and needed to recruit health care providers, especially nurses, from the mainland United States or neighboring international islands.13 ,14 ,15 For example, in September 2020 in Guam, when fatalities increased and as more providers left the island, island officials looked to recruit 100 nurses from mainland U.S. or nearby Philippines.16 An infusion of funds from the Coronavirus Aid, Relief, and Economic Security Act (CARES Act) helped some hospitals purchase additional hospital equipment and personal protective equipment (PPE).17 ,18
Puerto Rico saw increases in the average daily number of cases in March and April 2021, while the other territories remained steady. American Samoa is the only U.S. territory to have no cases or deaths to date. Despite increases in March and April in Puerto Rico, recent data show substantial decreases in the average daily number of cases. As of May 12, 2021, Puerto Rico’s average daily cases per million were 90.6, compared to 38.4 per million in Guam and 5.0 per million in CNMI. The average daily cases per million in USVI began increasing in early May, and as of May 12, it is the only current territory to surpass the U.S. rate of 111.9 cases per million (USVI had 139.3 cases per million population.19
Due to the previous surge in cases, Puerto Rico imposed more rigorous precautions. Early on, Puerto Rico issued overnight curfews and lock-down orders, which were punishable by fine or jail time.20 In June 2020, businesses were fully reopened,21 but variations of the curfew have remained in place. In-person schooling reopened in March but was closed as cases surged in April22 and beginning April 28, travelers must show proof of a negative COVID-19 test or face a $300 fine.23
Similar to the states, CNMI, Guam, and USVI also imposed lockdowns, including some travel restrictions into the islands, but have slowly reopened businesses with varying degrees of capacity and service.24 ,25 USVI has so far not altered its reopening plans to address the recent surge in cases in early May.26 American Samoa, which has had no reported COVID-19 fatalities, had already implemented social distancing and school closures in December 2019 due to a measles outbreak.27 In March 2020, in response to the pandemic, the government halted all flights in and out of the island, allowing only one weekly cargo flight in to provide medical supplies and food. Any American Samoa residents that left, including those needing medical services off the island during the pandemic, were not allowed to repatriate until early 2021.28
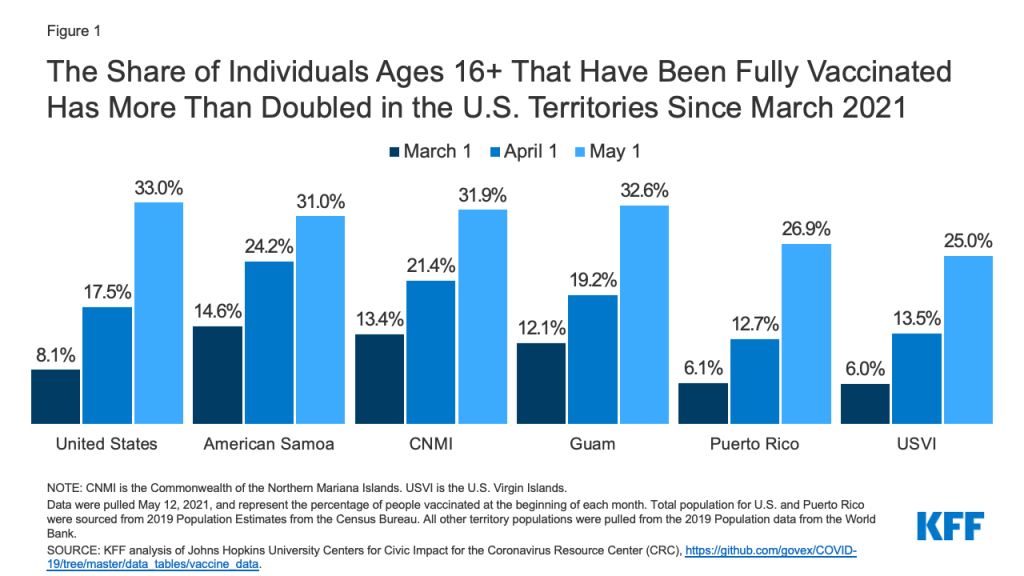
The share of individuals ages 16 and older that have been fully vaccinated has more than doubled, and in some territories quadrupled, from March 1 to May 1, 2021 (Figure 1). As of May 1, every territory, except Puerto Rico and USVI, has fully vaccinated more than 30% of the eligible population. The territories have received vaccines at rates similar to states in U.S,29 however some territories are administering a smaller share of delivered vaccines when compared to the U.S. overall. As of May 12, 2021, the share of delivered doses that had been administered in the U.S. was 78.5%, while CNMI and Puerto Rico’s shares were considerably lower (with 60.3% and 63.1% of delivered doses that have been administered, respectively). Issues related to administering vaccines could be caused by lack of staffing, challenges in reaching residents in more remote areas, or a lag in reporting.
The U.S. territories followed similar vaccination eligibility protocol to the U.S. with priority given to older populations, health care workers, and other essential workers. Additionally, all U.S. territories opened COVID-19 vaccinations to all adult residents earlier than President Biden’s April 19 deadline. Additionally, the territories utilized vaccination approaches that were tailored to their island’s needs to reach higher shares of their populations. For example, CNMI applied strategic outreach to the elders in the community,30 while American Samoa, which only has one public hospital, used a drive-through vaccination site as an additional means to reach a higher share of their population.31
Key Financing Issues for the Territories
Prior to the pandemic, the most of territories experienced fiscal stress that was exacerbated by natural disasters or emergencies. For example, USVI saw its economy declined by over 30% between 2008 and 2016, accompanied by population loss and job loss in certain industries, while Puerto Rico faced years of economic recession and debt, ultimately prompting the creation of the Financial Oversight and Management Board (FOMB). These economic challenges were exacerbated by the natural disasters which accelerated the outmigration of residents and health care providers, destroyed homes, schools, businesses and other infrastructure, and lead to the loss of revenue with reduced tourism and economic activity.
The structure of Medicaid financing for the territories has also contributed to fiscal stress. Unlike in the 50 states and D.C., annual federal funding for Medicaid in the U.S. territories is subject to a statutory cap and fixed matching rate. The territories’ federal matching rate (known as the federal medical assistance percentage, or FMAP) is fixed in statute, unlike the statutory formula for states, which is uncapped and adjusted annually based on a state’s relative per capita income. The U.S. territories’ FMAP rate is set to 55% (though it has been increased in the aftermath of natural disasters and the public health emergency), but if the matching rates were calculated using relative per capita income, all territories would receive a higher FMAP, likely at or close to the maximum allowable 83% matching rate. Notwithstanding temporary relief funds, once a territory exhausts its capped federal funds, it no longer receives federal financial support for its Medicaid program during that fiscal year. This places additional pressure on territory resources if Medicaid spending continues beyond the federal cap – making the effective matching rate lower than what is set in statute.
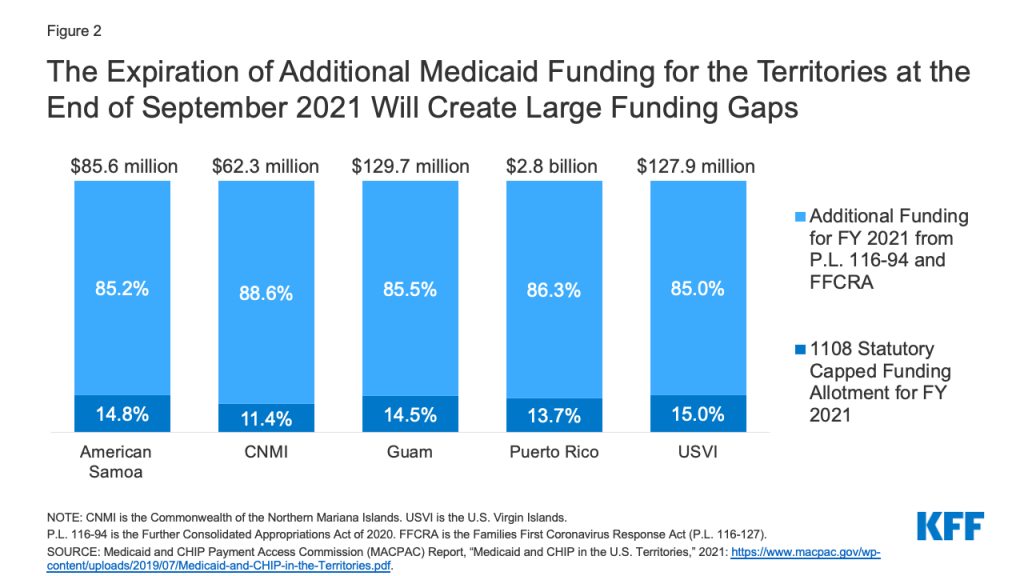
Over time, Congress has provided increases in federal funds for the territories broadly and in response to specific emergency events. Temporary funding can provide short-term relief, but also create fiscal funding cliffs that require ongoing Congressional action. The allotments for each of the territories for FY 2020 and FY 2021 are around seven to nine times the statutory levels as a result of additional funding added in the FY 2020 appropriation package and the Families First Coronavirus Response Act (FFCRA) (Figure 2). Puerto Rico was eligible for an additional $200 million in FY 2020 and FY 2021 contingent on a provider rate increase equal to at least 70 percent of what Medicare Part B would pay for services. In addition to increased federal funding, the traditional territory of 55 percent was increased to 76 percent for Puerto Rico and 83 percent for the territories through FY 2021 (with an addition increase of 6.2 percentage points as part of Medicaid fiscal relief available for all state and territories if certain maintenance of eligibility requirements are met). As noted in recent Congressional testimony, additional federal funding in Puerto Rico has been used to support increases in coverage, additional benefits (like hepatitis C treatment), and increased reimbursement for hospitals, physicians, and managed care plans.
While capped federal funding is often a constraint for the territories, territories have occasionally experienced difficulty putting up their share of funding that is necessary to draw down the federal funds. Loss of local revenue, especially revenue from tourism, both due to previous natural disasters and COVID-19 may impact the territories’ ability to use their federal funding. Increasing the federal match rate would assists the territories by requiring fewer territory funds to access to additional federal funding.
Unless Congress acts, the U.S. territories will lose over 80% of their funding and there will be a major Medicaid financing cliff in at the end of FY 2021. Without federal action, territories would need to make significant changes to their programs to cut Medicaid provider payments rates, benefits, or eligibility criteria while still managing the effects of the pandemic.
What to Watch Looking Ahead
New federal funds and efforts to provide vaccines will help address the pandemic. The American Rescue Plan Act provided $4.5 billion in Coronavirus State Fiscal Recovery Fund Payments that can be used to respond to the “negative economic impacts of COVID-19”32 and $700 million for critical capital projects to “directly enable work, education, and health monitoring in response to COVID-19”33 that may help alleviate some economic challenges for the islands.
The expiration of temporary Medicaid funding at the end of September 2021 will result in a major fiscal cliff if Congress does not act. The territories could lose the majority of federal Medicaid financing as the temporary funds make up more than eight in ten federal Medicaid dollars in each of territory. Without federal action, territories would need to make significant changes to their programs to cut Medicaid provider payments rates, benefits, or eligibility criteria while still managing the effects of the pandemic.
Congress may consider increasing the caps or more fundamental Medicaid financing changes such as eliminating the funding cap and revisiting how the FMAP is set. Increasing the funding caps could provide short-term relief. Congress may also consider proposals to eliminate Medicaid funding limits in the territories like, the Insular Area Medicaid Parity Act (HR 265), the Territorial Equity Act of 2021, or proposals that would transition funding from the current structure to achieve parity with other state programs over time (like HR 3371 from the last Congress that would achieve Medicaid financing for Puerto Rico over 10 years). Temporarily increasing the spending caps in the territories could avert the upcoming fiscal cliff; however, such action could also create another fiscal cliff in the future and create uncertainty in the availability of federal funding longer term without more permanent financing changes.
Endnotes
- Puerto Rico data are available for 2019. U.S. Virgin Islands data are available for 2016. ↩︎
- National Center for Chronic Disease Prevention and Health Promotion (NCCDPHP), How CDC Prevents Chronic Diseases and Promotes Health for US Territories and Affiliated Pacific Islands (Atlanta, GA: Centers for Disease Control, April 2019), https://www.cdc.gov/chronicdisease/resources/publications/factsheets/island-health.htm ↩︎
- Ibid. ↩︎
- U.S. Army Corps of Engineers, Facilities Condition Assessment Guam Memorial Hospital (Washington, D.C.: U.S. Army Corps of Engineers, April 2020), https://www.doi.gov/sites/doi.gov/files/uploads/oia-guam-memorial-hospital-facility-assessment.pdf ↩︎
- U.S. Department of the Interior, Office of the Inspector General, Insular Area Health Care: “At the Crossroads of a Total Breakdown” (Washington D.C.: U.S. Department of the Interior, Office of the Inspector General, September 2008), https://www.doioig.gov/sites/doioig.gov/files/2008-G-0040.pdf ↩︎
- U.S. Department of the Interior, Office of the Inspector General, Insular Area Health Care: “At the Crossroads of a Total Breakdown” (Washington D.C.: U.S. Department of the Interior, Office of the Inspector General, September 2008), https://www.doioig.gov/sites/doioig.gov/files/2008-G-0040.pdf ↩︎
- Averting A Crisis: Protecting Access To Health Care In The U.S. Territories, 117th Cong. (2021) (testimony of Congressman Gregorio Kilili Camacho Sablan). ↩︎
- Peter Georgiev and Adiel Kaplan, “American Samoa’s coronavirus conundrum: No Way to test,” NBC News (May 2020), https://www.nbcnews.com/health/health-care/american-samoa-s-coronavirus-conundrum-no-way-test-n1167776 ↩︎
- Ibid. ↩︎
- Dánica Coto, “Missteps mar Puerto Rico’s response to coronavirus,” AP News (April 2020), https://apnews.com/article/e5ba6c2639ee52dad5e367d2228ac764 ↩︎
- Patricia Mazzei, “Puerto Rico Lags Behind Everywhere Else in U.S. in Virus Testing,” The New York Times (August 2020), https://www.nytimes.com/2020/04/21/us/puerto-rico-coronavirus.html ↩︎
- Haidee Eugenio Gilbert, “Lack of nurses could slow community testing as COVID cases rise again,” The Guam Daily Post (August 2020), https://www.postguam.com/news/local/lack-of-nurses-could-slow-community-testing-as-covid-cases-rise-again/article_6a7808b8-d79d-11ea-9cd1-370bce05a80d.html ↩︎
- Emily Palmer, “Moored in a Fragile Paradise,” The New York Times (April 2020), https://www.nytimes.com/2020/04/17/travel/coronavirus-stjohn-caribbean.html ↩︎
- Michael Walsh and Elsie Lange, “How the tiny Pacific island of Guam became one of America’s coronavirus hotspots,” ABC News Australia (September 2020), https://www.abc.net.au/news/2020-09-11/guam-hospitals-under-pressure-after-coronavirus-outbreak/12637704 ↩︎
- Nicole Acevedo, “FEMA acknowledges Puerto Rico lacks rebuilt homes and a hospital to survive COVID-19,” NBC News (July 2020), https://www.nbcnews.com/news/latino/fema-acknowledges-puerto-rico-lacks-rebuilt-homes-hospital-survive-covid-n1234810 ↩︎
- Michael Walsh and Elsie Lange, “How the tiny Pacific island of Guam became one of America’s coronavirus hotspots,” ABC News Australia (September 2020), https://www.abc.net.au/news/2020-09-11/guam-hospitals-under-pressure-after-coronavirus-outbreak/12637704 ↩︎
- U.S. Department of the Interior, The Trump Administration is Supporting the People of the U.S. Virgin Islands (Washington, D.C.: U.S. Department of the Interior, 2020), https://www.doi.gov/sites/doi.gov/files/uploads/oia-covid19-wh-fact-sheet-usvi.pdf ↩︎
- U.S. Department of the Interior, Commonwealth of the Northern Mariana Islands Uses Interior CARES Act Funding to Strengthen COVID-19 Emergency Preparedness and Response Capabilities (Washington, D.C.: U.S. Department of the Interior, July 2020), https://www.doi.gov/oia/press/commonwealth-northern-mariana-islands-uses-interior-cares-act-funding-strengthen-covid-19 ↩︎
- Data are a KFF analysis of Johns Hopkins University Centers for Civic Impact for the Coronavirus Resource Center (CRC), https://github.com/govex/COVID-19/tree/master/data_tables/vaccine_data. Average daily number of cases are calculated as the average cases per million as a seven-day rolling average. For this analysis, the daily change in cases per million residents is averaged for the previous seven days. All data were pulled on May 12th, 2021. ↩︎
- Edmy Ayala and Patricia Mazzei, “Puerto Rico Orders Coronavirus Lockdown. Violators Could Be Fined,” The New York Times (March 2020), https://www.nytimes.com/2020/03/15/us/coronavirus-puerto-rico.html ↩︎
- Yanira Hernández Cabiya, “Dramatic economic reopening after 88-day lockdown,” Caribbean Business (June 2020), https://caribbeanbusiness.com/52221-2/ ↩︎
- Associated Press, “Puerto Rico will close schools amid COVID surge,” NBC News (April 2021), https://www.nbcnews.com/news/latino/puerto-rico-will-close-schools-covid-surge-rcna632 ↩︎
- Edmy Ayala and Patricia Mazzei, “Puerto Rico Just Had Its ‘Worst Moment’ for Covid-19,” The New York Times (April 2020), https://www.nytimes.com/2021/04/23/us/coronavirus-puerto-rico.html ↩︎
- United States Virgin Islands, COVID-19 – Path to a New Normal (United States Virgin Islands, March 2021), https://www.vi.gov/covid/phases/ ↩︎
- National Governors Association, Coronavirus State Actions (Washington D.C.: National Governors Association, July 2020), https://www.nga.org/coronavirus-state-actions-all/ ↩︎
- Reopening efforts were analyzed on May 12th, 2021. At that time, USVI had not made any changes from its previous “Safer at Home” phase. ↩︎
- Simon Romero, “A Place in the U.S. With No Covid-19? Look at American Samoa,” The New York Times (May 2020), https://www.nytimes.com/2020/05/06/us/coronavirus-american-samoa.html ↩︎
- Associated Press, “American Samoa Repatriation Program Detects 5 Virus Cases,” U.S. News (January 2021), https://www.usnews.com/news/best-states/hawaii/articles/2021-01-28/american-samoa-repatriation-program-detects-5-virus-cases ↩︎
- Rates were compared using “Total Doses Delivered Rate per 100,000” and data were analyzed on March 26th, 2021 and May 4th, 2021. See: Center for Disease Control, COVID Data Tracker (Centers for Disease Control, March 2021), https://covid.cdc.gov/covid-data-tracker/#vaccinations ↩︎
- Steve Limtiaco, “CNMI outpaces United States in COVID-19 vaccine rollout,” Pacific Daily News (January 2021), https://www.guampdn.com/story/news/2021/01/06/cnmi-covid-19-vaccine-rollout-best-us-cdc/6574087002/ ↩︎
- RNZ (Radio New Zealand), “Close to 24,00 Covid-19 vaccines rolled out in American Samoa,” RNZ (March 2021), https://www.rnz.co.nz/international/pacific-news/437798/close-to-24-000-covid-19-vaccines-rolled-out-in-american-samoa ↩︎
- Manatt Health, The American Rescue Plan: An Overview of Medicaid Provisions and State/Local Relief (Manatt Health, March 2020), https://www.shvs.org/wp-content/uploads/2021/03/FINAL-ARP-Medicaid-and-State_Local-Relief-Deck.pdf ↩︎
- Ibid. ↩︎