Unwinding of the PHE: Maintaining Medicaid for People with Limited English Proficiency
Introduction
Guidance from the Department of Health and Human services identifies individuals with limited English proficiency (LEP) as those who do not speak English as their primary language and who have a limited ability to read, write, speak, or understand English. Individuals with LEP disproportionately experience gaps in health insurance coverage and poor health outcomes, related to difficulties in comprehending and communicating health care information. Individuals with LEP make up a disproportionate share of the Medicaid population and are more likely than English proficient enrollees to experience administrative barriers to completing Medicaid renewal processes, which may result in them losing coverage despite remaining eligible. Because people of color are significantly more likely to have LEP than White people, these barriers can also exacerbate racial and ethnic health disparities.
Provisions in the Families First Coronavirus Response Act (FFCRA) require states to maintain continuous Medicaid enrollment for enrollees until the end of the month when the COVID-19 public health emergency (PHE) ends. The current PHE was extended in January 2022. The Biden Administration has said that it will give states a 60 day notice before the PHE expires. Since that notice was not issued in February, it is expected that the PHE will be extended again through mid-July which would mean that the continuous enrollment provisions could expire at the beginning of August 2022 (if legislation does not pass to set an earlier end date), unless the PHE is extended again.
When the continuous enrollment requirements end and states resume redeterminations and disenrollments, individuals with LEP may be at increased risk of losing Medicaid coverage or experiencing a gap in coverage due to barriers completing these processes, even if they remain eligible for coverage. In addition to the continuous enrollment provisions, many states have leveraged Medicaid emergency authorities to expand eligibility or streamline enrollment processes during the pandemic. However, it remains to be seen whether states will maintain these processes after the public health emergency ends.
This brief examines issues to consider for maintaining coverage for eligible people with LEP when the PHE ends, including:
- Who are Medicaid enrollees with LEP?
- What barriers might people with LEP face to maintaining coverage when the PHE ends?
- How can states mitigate coverage gaps and losses for eligible people with LEP?
Who are Medicaid enrollees with LEP?
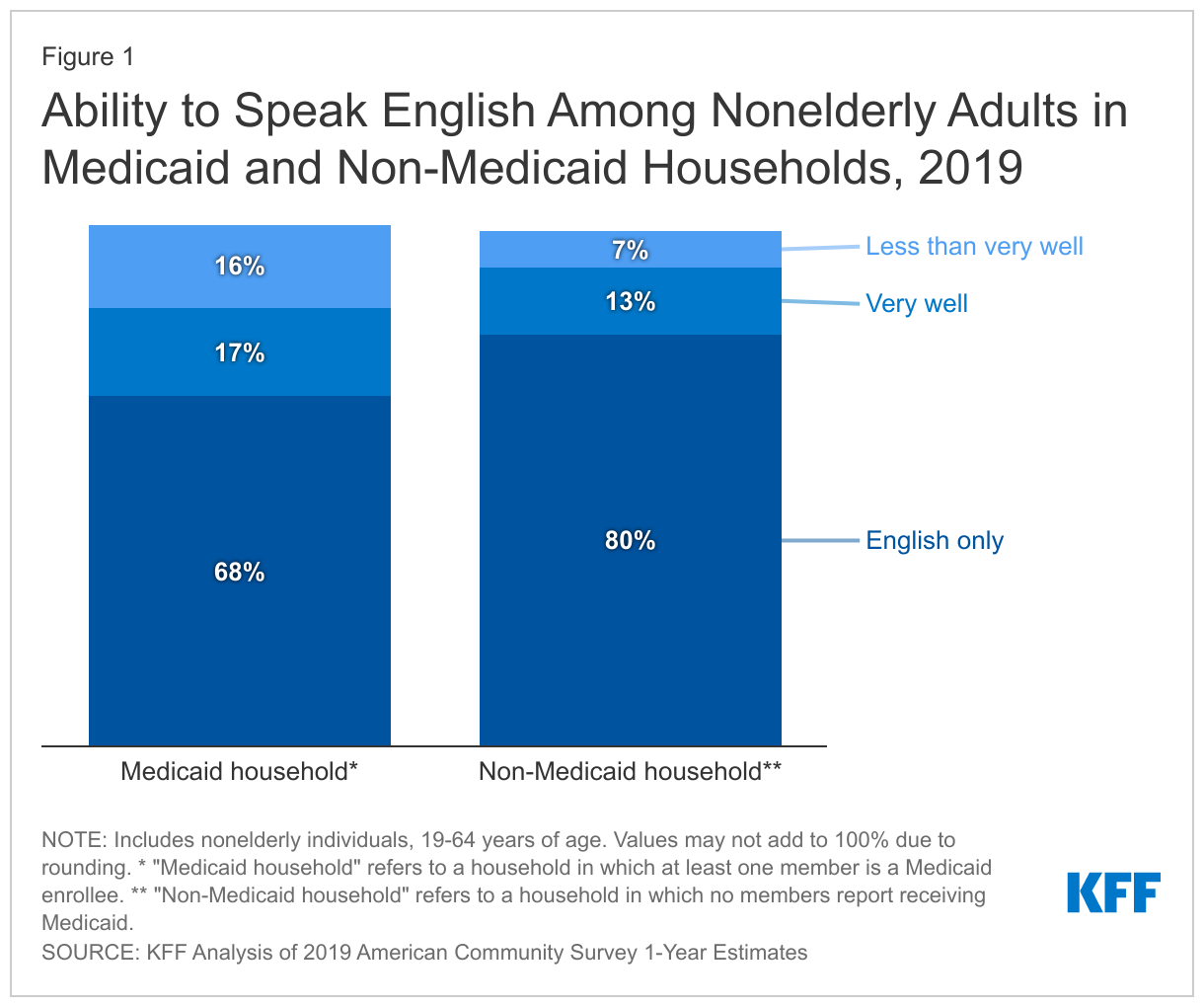
Medicaid households include a disproportionate share of nonelderly adults with LEP. Overall, 16% of nonelderly adults living in households with at least one Medicaid enrollee have LEP, meaning they reported speaking English less than very well, compared to 7% of nonelderly adults in households in which no member is enrolled in Medicaid (Figure 1). Moreover, nearly a quarter (23%) of children enrolled in Medicaid have a parent that speaks English less than very well.
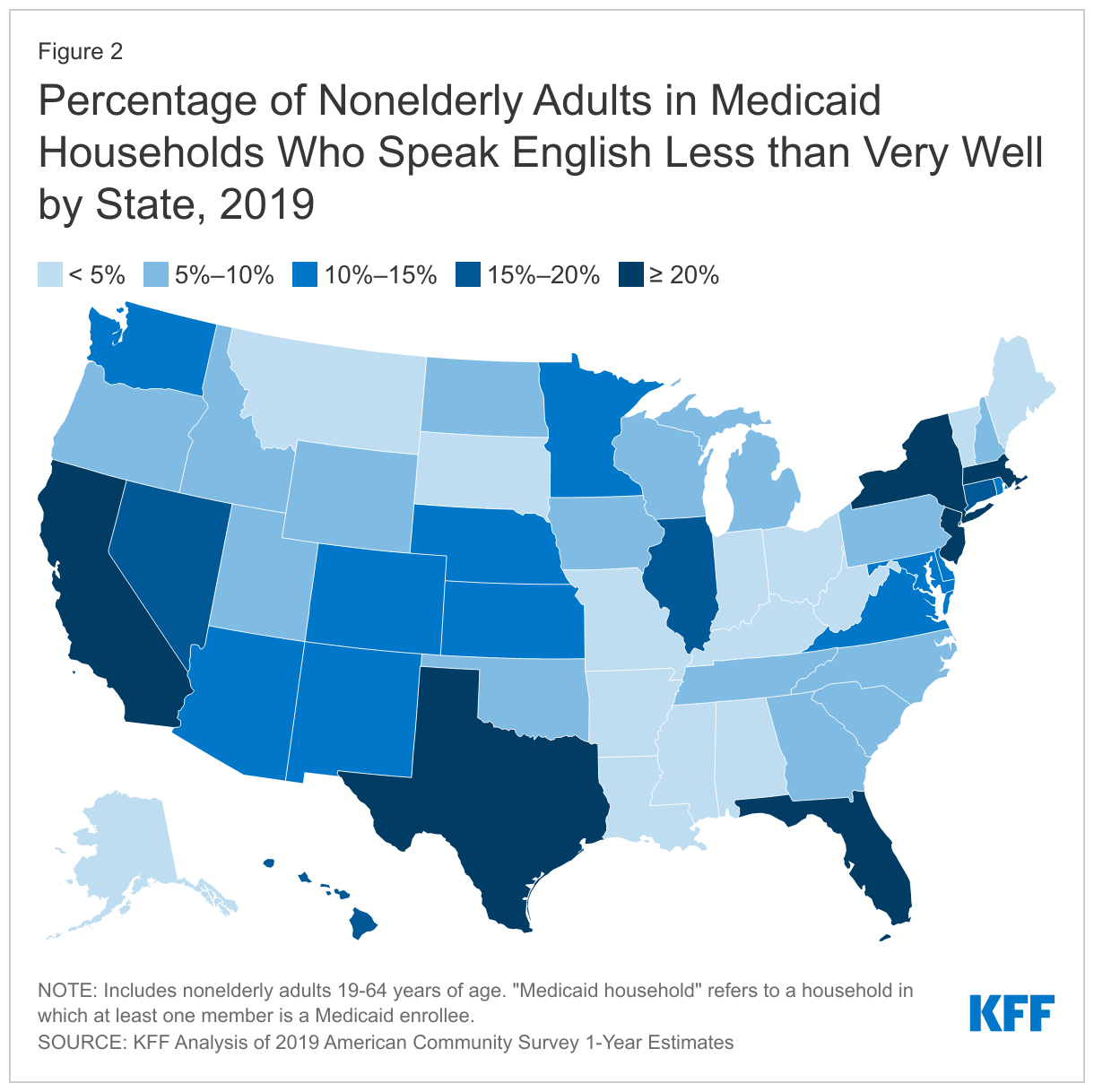
The share of nonelderly adults in a household with Medicaid who speak English less than very well is higher in some states. For example, the share of nonelderly adults in Medicaid households with LEP ranges from a low of less than 1% in West Virginia to a high of 29% in California (Figure 2). Other states with relatively high shares of nonelderly adults in Medicaid households with LEP include New Jersey (25%), New York (24%), Texas (25%), Massachusetts (21%) and Florida (21%).
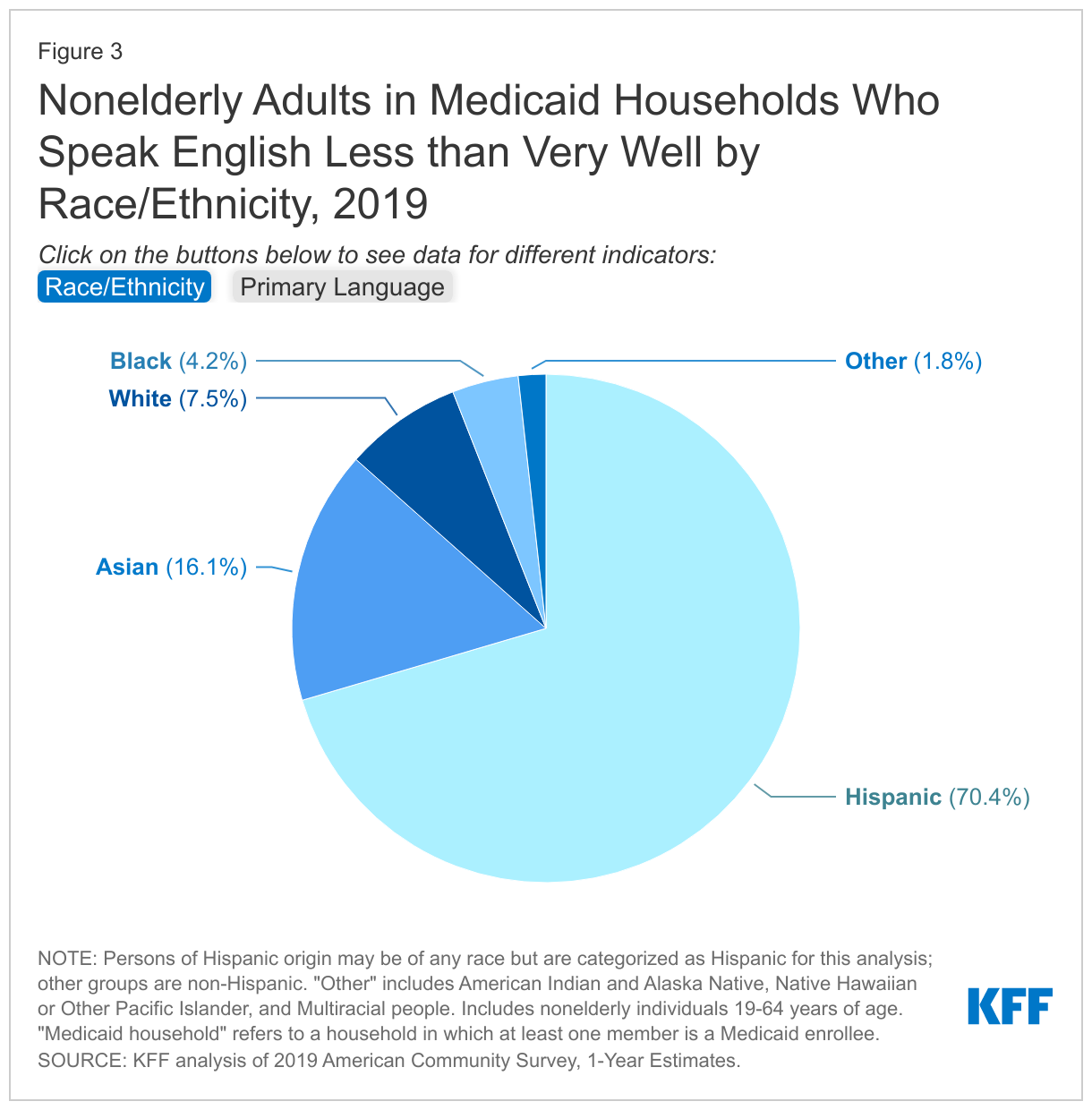
Most nonelderly adults in Medicaid households who have LEP are Hispanic and speak Spanish as their primary language (Figure 3). However, 16% are Asian, 7% are White and 4% are Black. While Spanish is the most common language spoken among nonelderly adults in Medicaid households who have LEP, Chinese and Vietnamese are each spoken by 3% of these adults, and there are a diverse set of languages spoken overall by this group. The other top ten languages spoken among these adults, include Arabic, Haitian, Tagalog, Korean, Portuguese, Russian and French. Moreover, the concentration of primary languages among this group will vary across areas.
What barriers might enrollees with LEP face to maintaining Medicaid coverage when the PHE ends?
All Medicaid enrollees may face administrative barriers to completing renewal and eligibility redetermination processes, but enrollees with LEP face increased risk of encountering difficulties due to language barriers. Complex enrollment and renewal processes have historically been barriers to obtaining and maintaining Medicaid coverage. Under current rules, states must first seek to renew eligibility automatically or on an ex parte basis, by checking all available data sources to confirm if eligibility can be renewed without contacting or requesting information from the family. However, due to differences in IT capabilities, states vary widely in how many renewals they are processing automatically. When a state is unable to confirm eligibility through available data sources, it must send requests for information and, in some cases, documentation to enrollees. All Medicaid enrollees may face potential challenges related to understanding redetermination processes, providing information and documentation when requested, and meeting required timeframes that can result in coverage losses among people who remain eligible. Enrollees with LEP are at particular risk for experiencing difficulties, as they may face added challenges understanding and completing tasks or forms due to language barriers, particularly if they are not provided materials translated into their language. For example, one study of Medicaid enrollees with LEP in Illinois found LEP respondents were over five times as likely to lose their Medicaid benefits compared to English proficient respondents at redetermination. The majority of LEP respondents reported having difficulty comprehending Medicaid renewal documentation and felt that completing the benefits renewal form was difficult or very difficult. Nearly half of LEP respondents also reported limited awareness of the redetermination process.
How can states mitigate Medicaid coverage gaps and losses for eligible people with LEP?
States can take a range of actions to mitigate coverage gaps and losses for eligible people when they resume eligibility determinations and renewals at the end of the PHE. The Centers for Medicare and Medicaid Services (CMS) outlined a range of policy and operational strategies for states to consider to maintain continuous coverage for eligible individuals when normal eligibility determination operations resume and specific strategies for Medicaid enrollees with LEP, including:
Streamlining renewal processes to minimize actions required by enrollees. Because enrollees with LEP may face increased difficulty understanding and completing forms or instructions, minimizing the actions people need to take to maintain coverage may be particularly helpful. States can minimize required actions by increasing the shares of Medicaid/CHIP renewals conducted automatically and simplifying processes for other renewals. CMS has identified steps states can take to increase the shares of renewals completed automatically, including expanding the types of data sources used for renewal and creating a data source hierarchy to prioritize the most recent and reliable data sources. For those renewals that cannot be completed automatically, CMS notes that states can support continuity of coverage by providing multiple modes for people to submit information (e.g., phone, mail, online, and in-person) and prepopulating forms, as required under federal rules, and by taking up other options, such as extending deadlines for response.
Facilitating access to clear and linguistically accessible communications, including notices and requests for additional information as well as throughs website and call centers. Under Title VI of the Civil Rights Act and Section 1557 of the Affordable Care Act, state Medicaid agencies are required to provide meaningful access to people with LEP. Guidance from the Department of Health and Human Services clarifies that state Medicaid agencies must take reasonable steps to ensure meaningful access to their programs by people with LEP by balancing four factors, including “1) The number or proportion of LEP persons eligible to be served or likely to be encountered by the program or grantee; (2) the frequency with which LEP individuals come in contact with the program; (3) the nature and importance of the program, activity, or service provided by the program to people's lives; and (4) the resources available to the grantee/recipient and costs.”
Sharing and implementing best practices used by states in meeting language access requirements. Earlier work has identified promising practices among states to facilitate access for people with LEP, including designating staff to coordinate language services activities; involving the community to assist with planning and implementing services; creating written language access plans that identify language needs and outline strategies to meet those needs; introducing availability of language services at individuals’ first point of contact through posters or signs; utilizing bilingual staff and well as contracting out for interpreters and translators, including telephone language lines; and translating documents or providing taglines on documents to inform individuals about interpreter availability when resources are not available for full translation. For example, Colorado requires all Medicaid client correspondence to be accurately translated into the second most commonly spoken language in the state and include a tagline, translated into the top 15 languages spoken in Colorado by individuals with LEP, informing enrollees how to seek further assistance in understanding the content of correspondence. Beyond these strategies to facilitate communication with enrollees, states can also design policies to minimize coverage gaps for people with LEP. For example, Tennessee allows good cause extensions for individuals who do not complete the Medicaid eligibility determination paperwork in a timely manner if they require and are not provided assistance with English translation.
Adopting CMS suggested strategies for communicating effectively with people who have LEP to maintain coverage of eligible individuals when the PHE ends. These strategies include:
- Review their language access plans to provide written translation and oral interpretation of information and advice to individuals with LEP on how they can access free language services;
- Translate notices, forms, and other communications into multiple languages by qualified translators and review these materials for cultural competence;
- Review and enhance access to and availability of qualified oral interpreters who speak frequently spoken languages in person and through qualified telephonic interpreters, and
- Update websites with taglines in non-English languages to advise people with LEP on how they can access language services free of charge.
The Department of Justice (DOJ), also recently released recommended strategies from a federal interagency working group for improving access to public websites and digital services for people with LEP. These include making vital digital information accessible to people with LEP by translating content, prominently displaying multilingual content on websites and translating dropdown menus and search bars, ensuring translated content links to other content that is translated or communicating that the link leads to English content, and ensuring website and digital services inform people of how to access language assistance services.
Engaging with trusted community partners to conduct outreach and provide assistance. A combination of broad and targeted outreach strategies will be important for helping enrollees understand renewal requirements and maintain coverage. Working closely with community partners to conduct outreach and provide assistance will be particularly important for effectively reaching enrollees with LEP. CMS suggests states work with community-based organizations, application assisters, and providers to remind enrollees to provide updated contact information and about renewal or eligibility redetermination requirements. CMS also advises states to conduct outreach through multiple modalities, including using text messaging to send reminders to enrollees about requested information or required actions. In August 2021, CMS announced $80 million in funding for 60 Navigator programs in 30 states with Federally-Facilitated Marketplaces for the 2022 plan year, significantly higher than the annual funding awarded in 2018-2020. Navigator programs must provide information that is culturally and linguistically appropriate. Navigators can assist individuals with renewing Medicaid coverage and help those who are no longer eligible for Medicaid transition to coverage through the marketplaces, which may be particularly important for people with LEP.