A Look at the Intersection of SNAP and Medicaid as States Implement Medicaid Work Requirements
On July 4, President Trump signed the 2025 reconciliation law that makes significant changes to the Medicaid program, including new requirements for states to implement work requirements. Starting January 1, 2027, states must condition Medicaid eligibility on meeting work requirements for individuals enrolled through the Affordable Care Act (ACA) Medicaid expansion pathway and through certain state waivers. To ease the burden on individuals, the law directs states to use available information “where possible” to verify compliance with Medicaid work activities or exemption status, without requiring additional documentation from individuals.
The Supplemental Nutrition Assistance Program (SNAP), the federal aid program addressing food insecurity among low-income households, is an important source of data that can be used to identify individuals who are in compliance with or exempt from the Medicaid work requirements. Both Medicaid and SNAP target low-income households, and many individuals receive benefits through both programs; overall, most people who receive SNAP benefits are covered by Medicaid. As a result, some states have integrated eligibility systems or otherwise share data between the two programs. In addition, SNAP has long-standing work requirements for certain “able-bodied” adults without dependents, so coordination among agencies can streamline the collection of information to verify compliance with requirements in both programs. The reconciliation law introduced changes for the population subject to work requirements in SNAP that align them more closely with the new Medicaid work requirements, but differences remain between the programs.
New Medicaid work requirements and changes to SNAP work requirements are expected to impact enrollment in both programs. The Congressional Budget Office (CBO) estimates that Medicaid work requirements will increase the number of uninsured by 5.3 million over the next ten years, and that changes in who will need to meet work requirements will reduce participation in SNAP by roughly 2.4 million people in an average month over the 2025-2034 period. The changes to SNAP work requirements to align with Medicaid mean there could be overlap in the populations projected to lose SNAP and Medicaid benefits. This brief describes the intersection between Medicaid and SNAP and discusses how information from SNAP may be leveraged by states when implementing the new Medicaid work requirements.
What are Medicaid and SNAP Work Requirements?
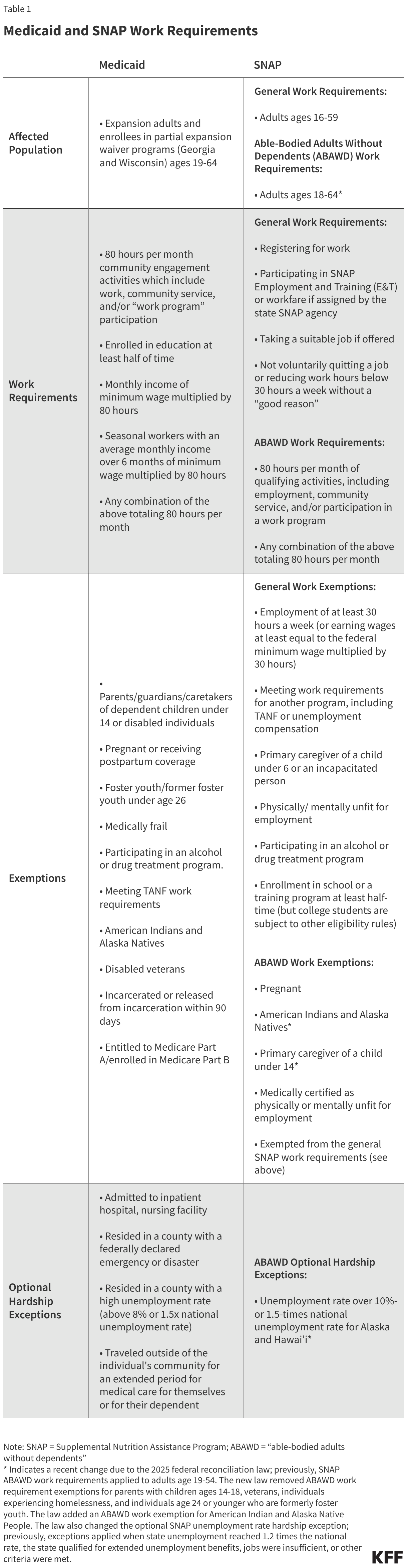
Beginning January 1, 2027, states must require expansion adults and enrollees in partial expansion waiver programs (Georgia and Wisconsin) to complete 80 hours of work or community service activities per month or meet exemption criteria to enroll in Medicaid and maintain coverage. At a minimum, states will be required to verify individuals’ work or exemption status when individuals apply for coverage and at eligibility renewal. The law specifies mandatory exemptions, including being in a household receiving SNAP and not exempt from SNAP work requirements. Other exemptions include parents and caretakers with children ages 13 and under, individuals who are “medically frail,” and individuals who are pregnant or postpartum, among others (Table 1). When a state is unable to verify compliance with the requirements or that an individual meets exemption criteria through data matching, it must issue a “notice of noncompliance” and deny the application or disenroll the individual from Medicaid coverage if the individual is unable to show compliance within 30 days.
SNAP has its own work requirements and exemptions, but these do not fully align with the new Medicaid work requirements and exemptions. While most adults on SNAP must meet general work requirements, individuals who are considered “able-bodied adults without dependents” (ABAWDs) must work or participate in a work program for at least 80 hours per month or participate for an assigned number of hours in workfare to receive SNAP benefits for more than three months in a 36-month period (Table 1). The reconciliation law made changes that went into effect at the end of 2025 affecting the ABAWD population subject to this 80 hour per month work requirement, including newly subjecting adults ages 55 to 64 and parents with children ages 14 and older to these requirements, as well as removing previous exemptions for veterans, people experiencing homelessness, and young adults who aged out of foster care and who are under age 24. The law also added a new exemption for American Indian and Alaska Native People and changed the criteria for optional hardship exceptions for areas facing high unemployment. These changes make the SNAP requirements more consistent with Medicaid work requirements, although differences remain. For example, unlike SNAP, Medicaid work requirements include exemptions for individuals recently released from incarceration, as well as optional short-term hardship exceptions states can adopt for individuals with inpatient or nursing facility admissions, residents of counties with a disaster declaration, and those who have traveled outside their community for medical care (Table 1).
What do we know about the intersection between Medicaid and SNAP?
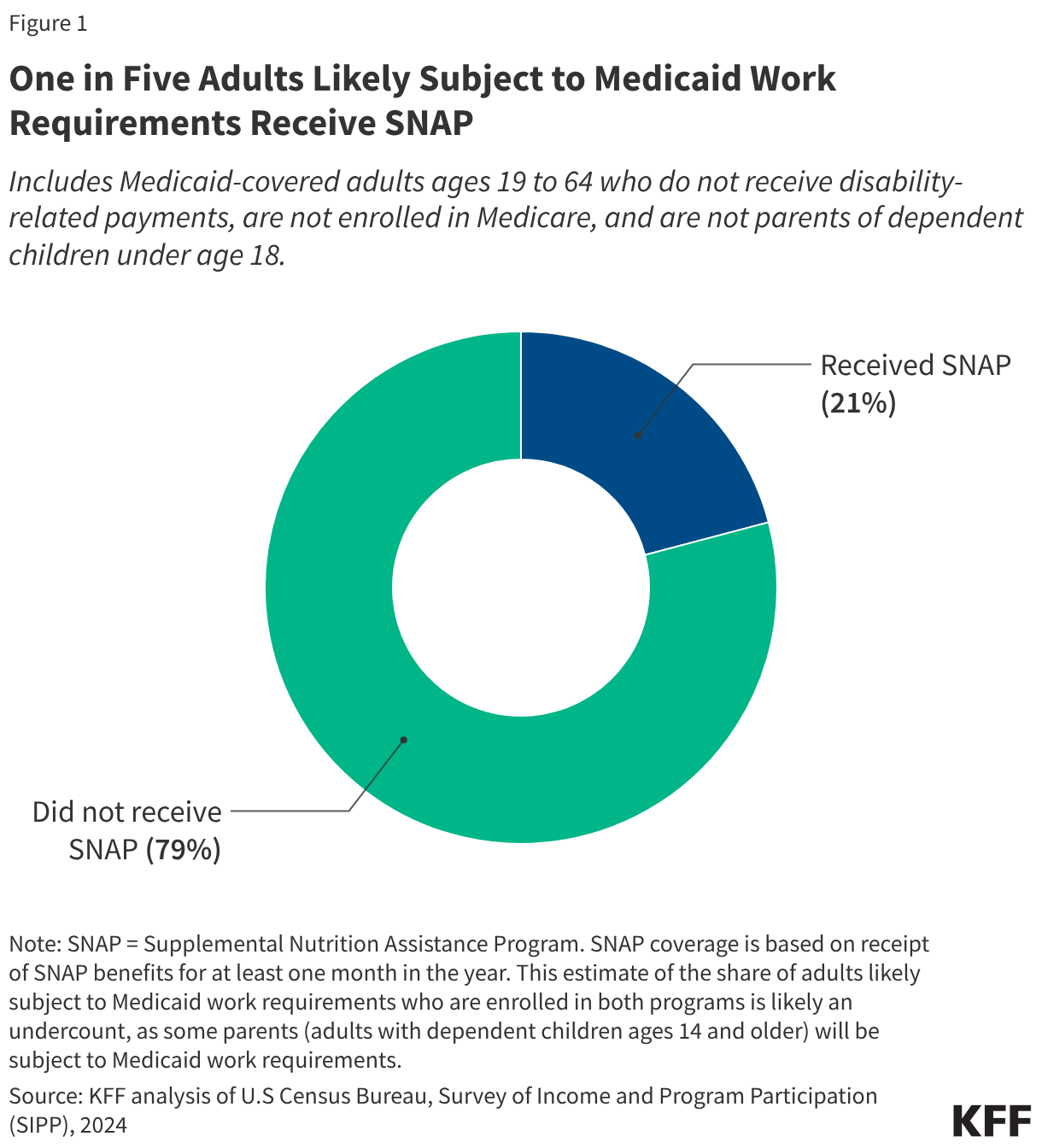
About one in five Medicaid-covered adults who will likely be subject to the new work requirements also receive SNAP benefits (Figure 1). Similar eligibility requirements, particularly in Medicaid expansion states, account for this overlap in enrollment. In the 41 states (including DC) that have expanded their Medicaid programs, the income eligibility limit for adults is 138% of the federal poverty level (FPL), which is $22,024 for an individual in 2026 or $1,835 per month. The income eligibility limit for SNAP is 130% FPL gross monthly income ($1,696 for an individual in 2026) and 100% FPL net monthly income reflecting certain deductions ($1,305 for an individual in 2026); though definitions of income and household composition rules differ somewhat between SNAP and Medicaid. This estimate of the share of adults likely subject to Medicaid work requirements who are enrolled in both programs is likely an undercount as it excludes Medicaid adults with dependent children ages 14 and older. While nearly all SNAP participants are also enrolled in Medicaid, because SNAP participation is much lower than total Medicaid enrollment, the share of Medicaid enrollees who also receive SNAP is lower. This analysis focuses on adults who would likely qualify for an exemption from Medicaid work requirements due to being in a household receiving SNAP and not exempt from SNAP work requirements. When looking at the broader population of all Medicaid adults ages 19-64, the share receiving SNAP benefits rises to one in three individuals.
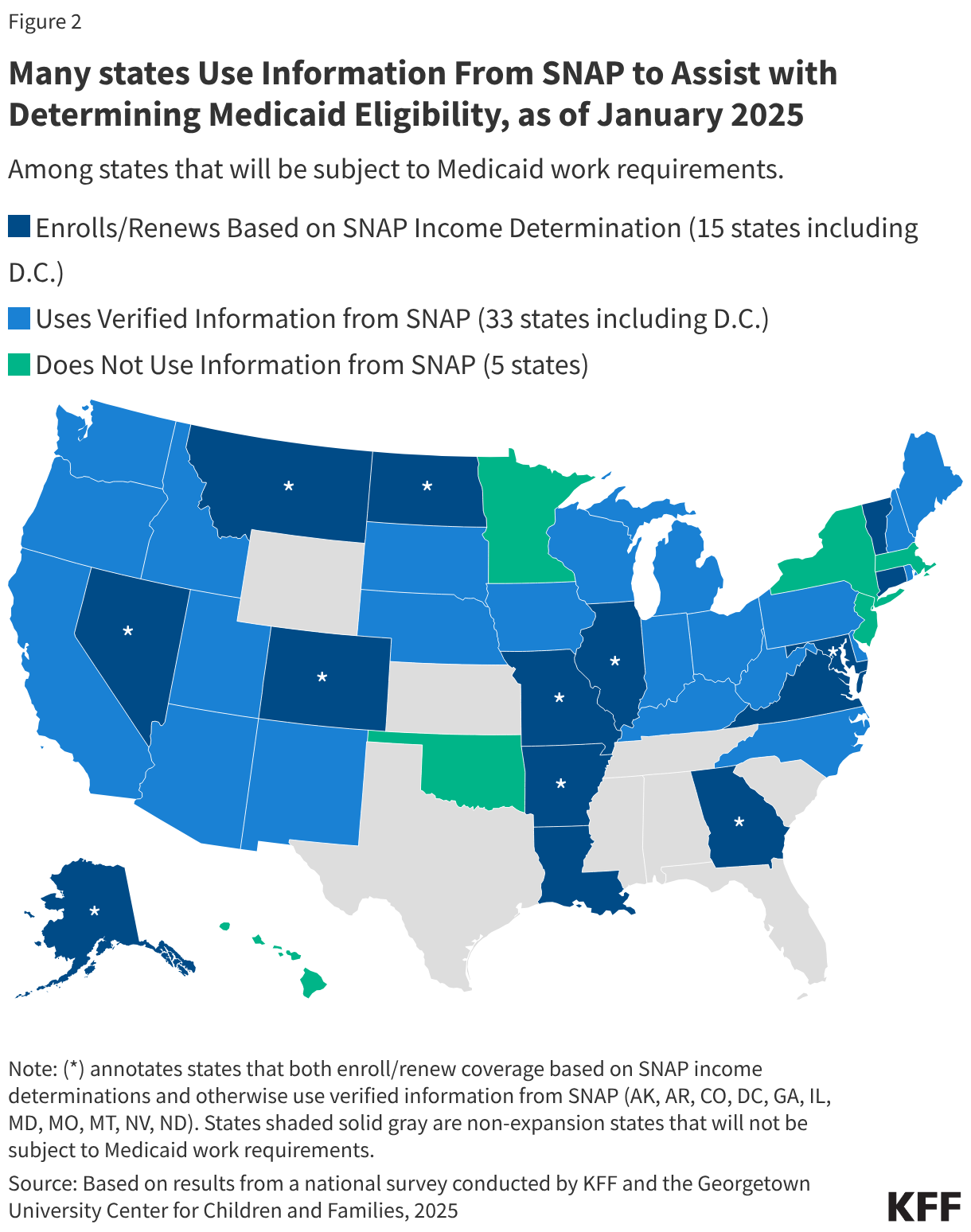
In part because of the overlap in eligibility between the two programs, many states use information from SNAP to assist with determining Medicaid eligibility. Most Medicaid programs are already facilitating coordination of enrollment processes and systems between Medicaid and SNAP. For example, 29 states affected by the new Medicaid work requirements allow individuals to apply for Medicaid and SNAP through a single online application and 24 states affected by the new Medicaid work requirements make eligibility determinations for Medicaid and SNAP through a single shared system. In addition, among states that will be subject to Medicaid work requirements, 15 enroll or renew individuals in Medicaid using SNAP income determinations, and 33 states use information from SNAP to identify and act on potential changes in eligibility between renewals, including 10 states and DC that do both, as of January 2025 (Figure 2).
How can states use data from SNAP to implement Medicaid work requirements?
States can use information from SNAP to identify individuals who may be exempt from Medicaid work requirements and those who are meeting the requirements. States are required to use available data from reliable sources to “data match” the work or exemption status of individuals to lessen the administrative burden on both enrollees and Medicaid staff. Although CMS has not released formal guidance, it is anticipated that states will be required to access SNAP and TANF data for the purpose of determining compliance with work requirements. Successful automation to verify compliance with Medicaid work activities or exemption status can lower the risk of eligible people not being able to enroll in Medicaid or losing their coverage due to not submitting proof of work hours or exemption status. States can use information already collected by SNAP to identify individuals in a household receiving SNAP who are not exempt from SNAP work requirements, and who are, therefore, exempt from the Medicaid requirements. SNAP data can also be used to identify individuals who qualify for exemptions because they are medically frail, are participating in a drug or alcohol addiction program, or are American Indians or Alaska Natives. States can also use income information from SNAP to verify compliance with Medicaid work requirements. While some of this information on work and exemption status is likely available for current Medicaid enrollees, SNAP can be a source of data for applicants for whom Medicaid agencies do not have this information.
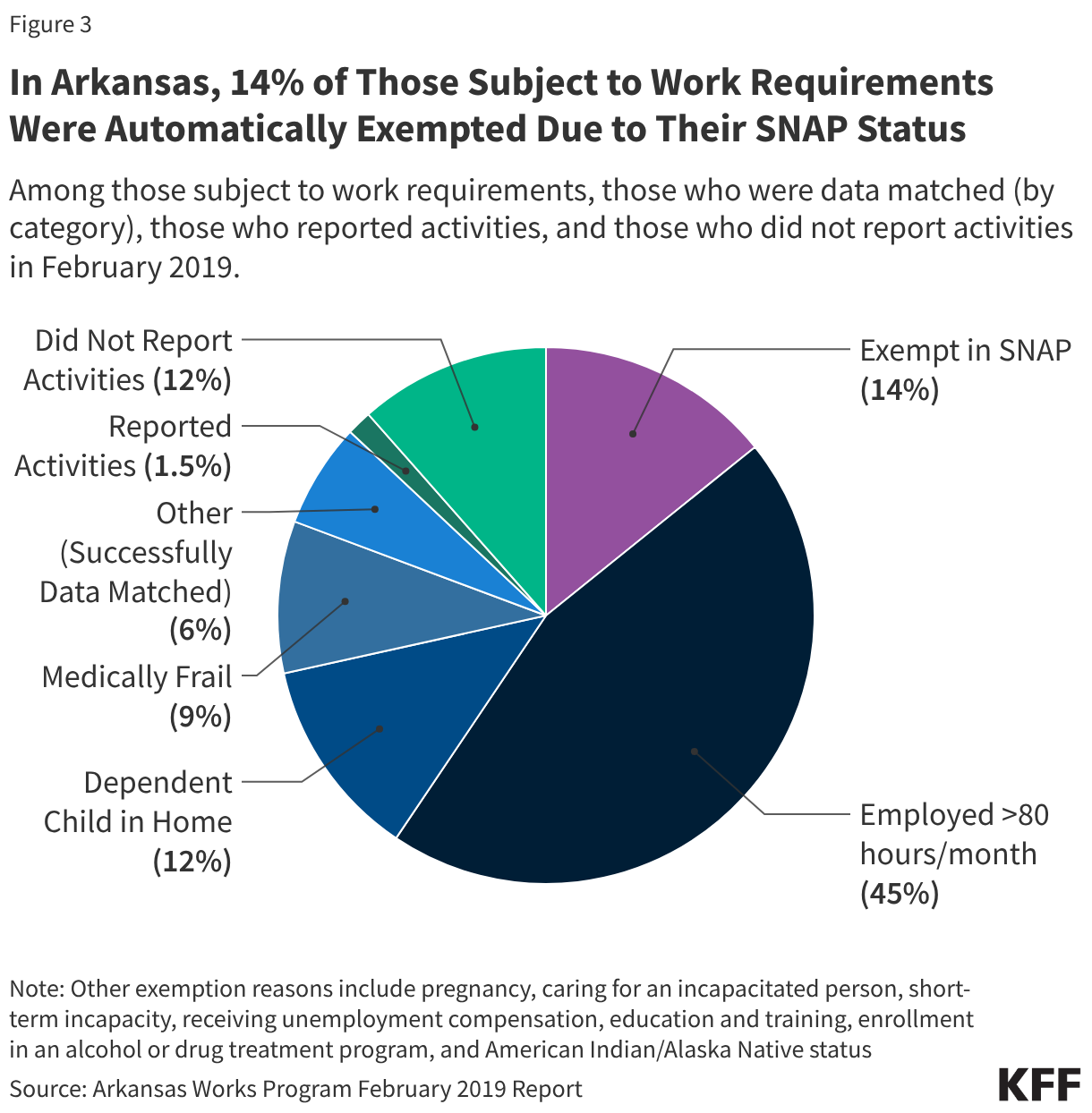
When Arkansas implemented work requirements in 2018, the state used SNAP data to verify exemptions and compliance with work hours. Of the 116,000 individuals subject to work requirements in February 2019, Arkansas was able to determine that 87% of enrollees were meeting or exempt from the work requirements through data matching (Figure 3). Most individuals whose status was verified using available data fell into four categories: those who were already working at least 80 hours per month (45%), those meeting or exempt from SNAP employment and training requirements (14%), those with a dependent child in the household (12%), and those identified as medically frail (9%). Most enrollees who were not data matched ultimately did not report any work activities in that month. Arkansas did not have integrated eligibility systems, but implemented a daily file exchange between its SNAP and Medicaid systems to update exemption and compliance information across programs without manual intervention. Although Arkansas’ work requirements differ from the new federal requirements in key ways, the experience shows how states can use SNAP data when implementing the new Medicaid work requirements.
Data sharing between Medicaid and SNAP will be easier in states that have integrated eligibility systems; however, these states may also face unique issues in addition to the challenges all states will likely face when making necessary system changes for both programs. Of the many systems changes needed, states have previously reported prioritizing enhancing capabilities to collect and match data from multiple agencies and external sources to reduce the burden on applicants and enrollees for documenting their work or exemption status. However, states may face different challenges based on their current Medicaid eligibility system integration with SNAP. States that do not currently link to SNAP will need to establish an interface to share data between agencies. Some states may face difficulty establishing this linkage and may require more time to put it into place. States with integrated Medicaid and SNAP eligibility systems needed to prioritize completing work requirement changes for SNAP that went into effect at the end of 2025, which may have delayed the initiation of work on the Medicaid changes. Any delays in preparing for Medicaid work requirements could potentially increase costs. In addition, as states implement complex SNAP and Medicaid eligibility and enrollment policy changes, they will also need to prepare for changes to the payment error rate measurement (PERM) program at the same time, requiring states to make decisions on how to apply scarce state resources and mitigate budgetary consequences. Beginning in 2028, the reconciliation law requires states to pay a portion of SNAP benefit costs, depending on the state’s payment error rate, and starting October 1, 2029, HHS will be required reduce federal Medicaid financial participation to states that exceed a three percent PERM eligibility error rate threshold.