Overview of Data on Race/Ethnicity of COVID-19 Booster Shot Recipients
As of October 21, 2021, the Centers for Disease Control and Prevention (CDC) recommended that people who received the Pfizer-BioNtech or Moderna COVID-19 vaccine receive a booster shot if they are age 65 years and older, have underlying medical conditions that put them at higher risk for severe illness, or are in high-risk occupational and institutional settings. For people who got the Johnson and Johnson COVID-19 vaccine, the CDC recommends they get a booster if they are age 18 and older and were vaccinated two or more months ago. Data from CDC indicate that as of November 2, 19.8 million fully vaccinated people have received booster shots of the COVID-19 vaccine. However, data currently are limited to understand whether there are racial disparities in booster shot uptake. Increasing the availability of data to understand who is receiving booster doses is important for identifying and addressing potential disparities in COVID-19 booster shot uptake. This data note reviews data currently available at the federal and state level on race/ethnicity of booster shot recipients.
Federal COVID-19 Booster Dose Vaccination Data
The CDC is not reporting race/ethnicity of booster dose recipients at this time, although may begin reporting these data in the future. As of November 2, 2021 CDC reports the total number of booster shots administered and share of fully vaccinated people who have received a booster dose for the total population, adults 18 years of age and older, adults 50 years of age and older, and adults 65 years of age and older. These data show that as of November 2, 2021, about 10% of fully vaccinated people had received a booster dose, including over 25% of fully vaccinated people age 65 and older.
Separately, the Health Resources and Services Administration (HRSA) reports data on booster shot recipients for individuals who received them at a community health center. These data are based on the bi-weekly Health Center COVID-19 Survey and include race/ethnicity of booster dose recipients at the federal and state level. Community health centers are a primary source of care for low-income populations and people of color and have been a key federal partner in facilitating equitable access to vaccines.
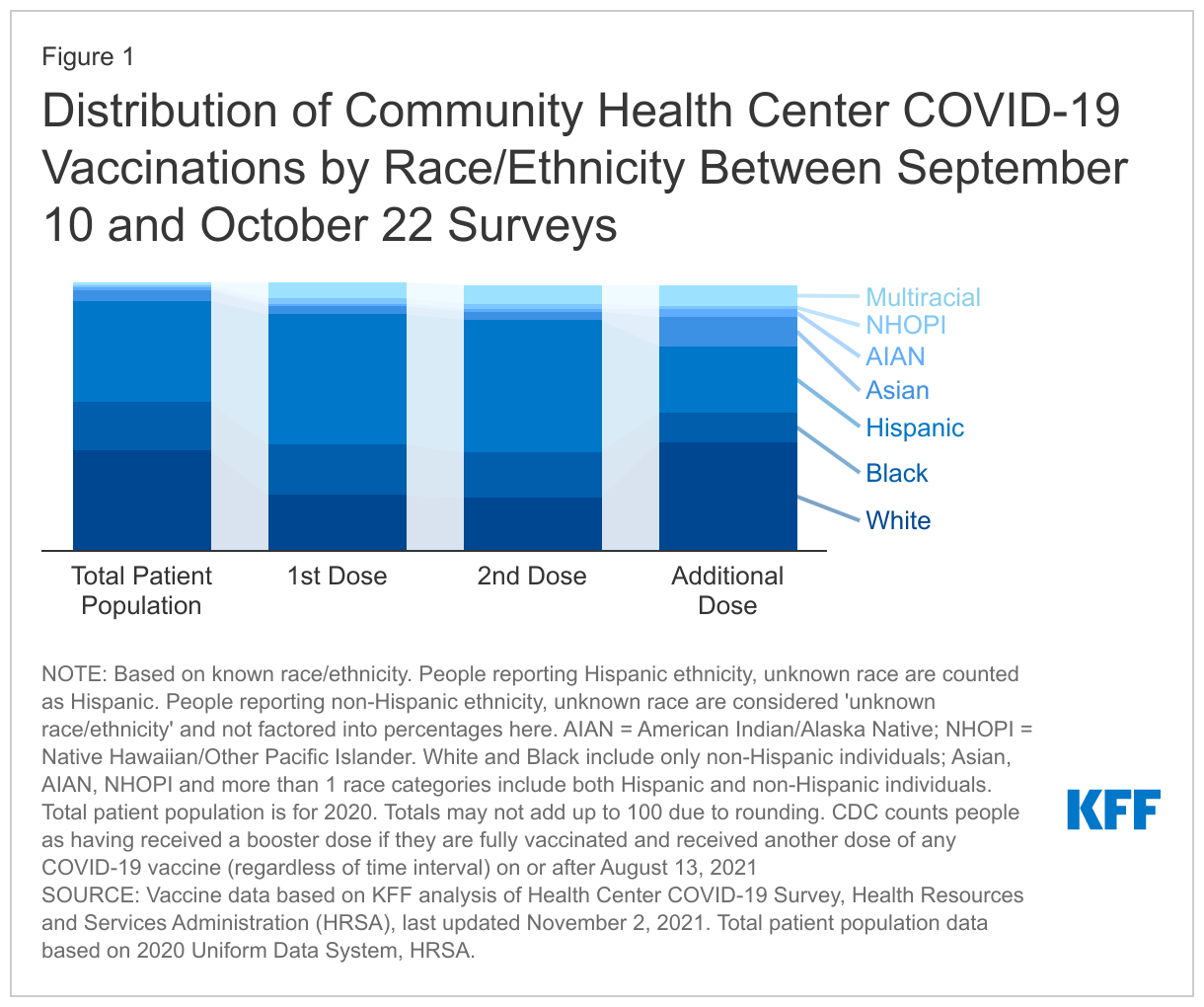
Community health centers are providing first and second doses of the vaccine to people of color at rates higher than their share of the overall patient population, but the share of booster dose recipients who are people of color is similar to the share of the total patient population. In 2020, 62% of community health center patients were people of color. In contrast, between the September 10 and October 22 surveys, 80% of first and second dose vaccine recipients with known race/ethnicity were people of color. Only 59% of booster dose recipients at community health centers surveyed during the same period were people of color. White, Asian, American Indian and Alaska Native (AIAN) and multiracial people received similar or larger shares of booster doses compared to their representation in the overall patient population between the September 10 and October 22 surveys, while Hispanic, Black, and Native Hawaiian and Other Pacific Islander (NHOPI) people received smaller shares of booster shots. A larger share of booster doses also had unknown or missing race/ethnicity data (18%) compared to initial (14%) and second (13%) doses.
State COVID-19 Booster Dose Vaccination Data
As of October 28, 2021, 27 states and Washington, DC were publicly reporting the total number of individuals who received booster or additional doses of the COVID-19 vaccine, but only 7 of these states (Colorado, Delaware, Michigan, Mississippi, New Jersey, Ohio, and Oregon) reported the race and ethnicity of booster dose recipients. As with state reporting of data for first and second doses, states vary in how they report booster dose data by race and ethnicity and in the completeness of their data. Delaware and New Jersey do not report data for AIAN or NHOPI people; Michigan combines Asian and Pacific Islander people into a single category, and the states vary in whether they report Hispanic ethnicity separately from race.
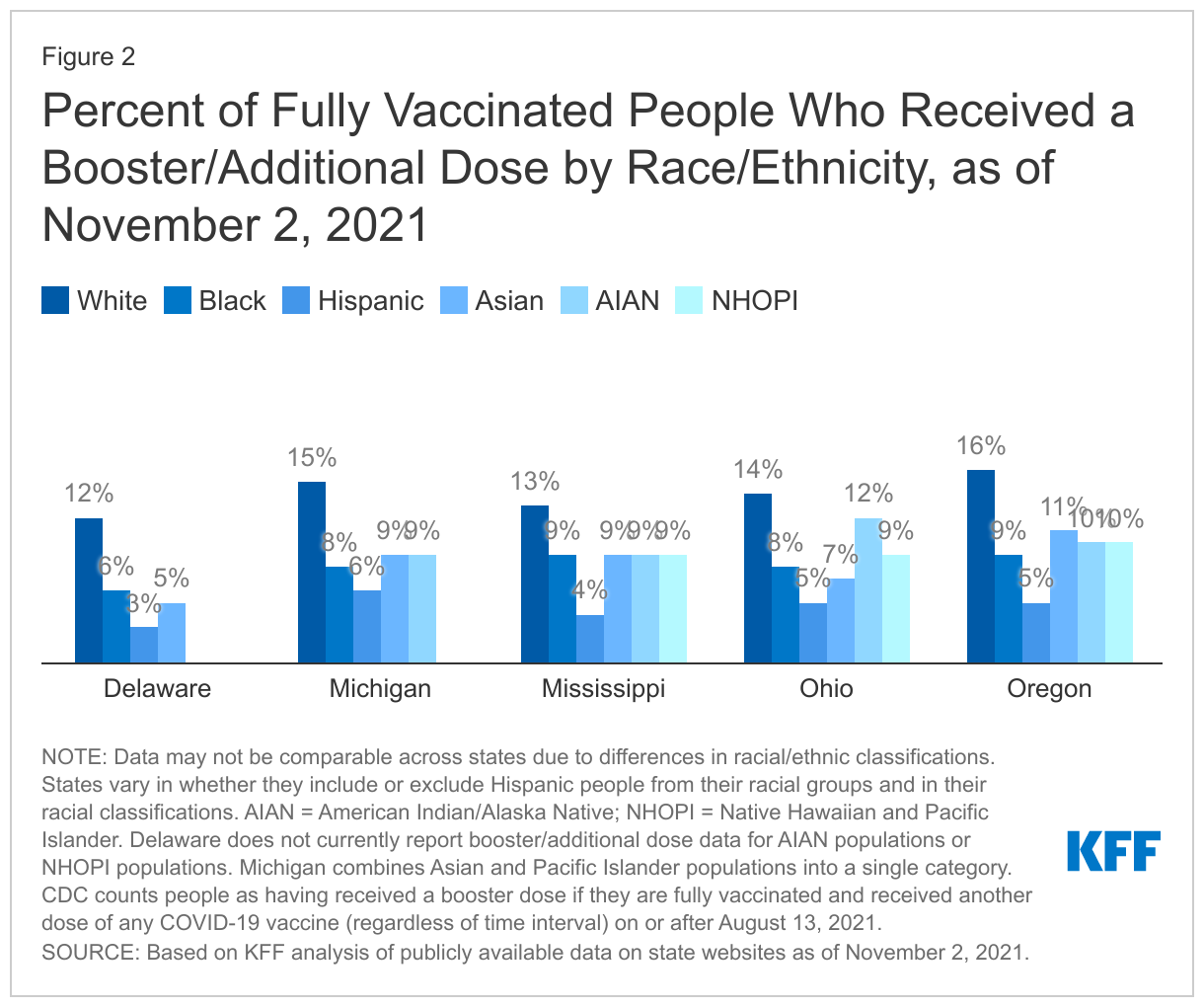
The limited data on booster shots by race/ethnicity available to date show that fully vaccinated White people are more likely to have received a booster dose compared to other groups as of November 2, 2021. Across the five states where we were able to calculate the share of fully vaccinated people who have received a booster dose by race/ethnicity, the share of fully vaccinated White people who had received a dose was higher compared to other racial/ethnic groups. These differences were largest compared to Hispanic people in all five of the states.
Discussion
In sum, to date, there is limited data on race/ethnicity of COVID-19 booster shot recipients. The limited data available to date suggest that fully vaccinated White people are more likely to have received a booster shot compared to other racial/ethnic groups. White people account for a larger share of booster shot recipients at community health centers compared to first and second dose recipients. Moreover, in the few states reporting data, a higher share of fully vaccinated White people received a booster dose compared to other racial/ethnic groups.
These patterns, in part, may reflect differences in the age distribution of racial/ethnic groups. CDC has recommended that people age 65 and older receive booster shots if they received a Pfizer or Moderna COVID-19 vaccine, and White people are more likely than people of color to be age 65 or older (21% vs. 10%).1 However, CDC guidance also notes that adults between ages 18-64 who have underlying health conditions and those who are at increased risk for COVID-19 exposure and transmission because of occupational or institutional setting may obtain a booster. Previous analysis has shown that people of color are more likely to have underlying health conditions that put them at increased risk for serious illness if infected with COVID-19 and to work in frontline essential jobs that increase risk of potential exposure to the virus. Further, it remains difficult to interpret the booster shot data because data are not available on who is eligible for a booster shot by race/ethnicity. For example, booster shot recommendations vary by type of vaccine received, with all adults who received the Johnson and Johnson vaccine recommended to get a booster shot two months or more after their initial dose. However, racial/ethnic data are not available for vaccine recipients by vaccine type. Going forward, comprehensive, consistent, and complete racial and ethnic data will be key for identifying potential disparities in uptake of the booster shots and directing efforts to address those disparities.
- KFF analysis of 2019 American Community Survey data. ↩︎