Section 1115 Waiver Watch: Continuous Eligibility Waivers
Note: For the latest information on states with approved and pending waivers to extend multi-year continuous eligibility for children, view our Section 1115 tracker “Key Themes Maps.“
The pandemic continuous enrollment provision and other research show that continuous eligibility reduces Medicaid disenrollment and “churn” rates and helps to ensure stable coverage. Guaranteeing 12-month continuous coverage for children has long been an option in Medicaid and CHIP without a waiver, but not for adults. The Consolidated Appropriations Act required all states to implement 12-month continuous eligibility for children beginning on January 1, 2024. As many Medicaid enrollees are currently experiencing disruptions in coverage as a result of the Medicaid unwinding, a number of states are pursuing strategies to help promote continuity of coverage, including through unwinding waivers and Section 1115 demonstration waivers. This Waiver Watch summarizes approved and pending Section 1115 waivers with continuous eligibility provisions for children and adults in Medicaid.
What is continuous eligibility?
States are required to provide 12-month continuous eligibility for children in Medicaid and CHIP. Continuous eligibility generally allows individuals to remain enrolled for a specific period even if there are fluctuations in income. States have long had the option to provide 12 months of continuous eligibility to children (under age 19) without a waiver, and many states (23 as of January 2023) had taken up that option for all children in Medicaid and CHIP (additional states had adopted 12-month continuous eligibility for only some children or only children in CHIP). However, the Consolidated Appropriations Act required all states to implement 12-month continuous eligibility for all children in Medicaid and CHIP beginning on January 1, 2024. Additional guidance issued on October 27, 2023 prohibits states from terminating coverage of children enrolled in CHIP for failure to pay premiums. Under the previous 12-month continuous eligibility option, states were permitted to disenroll children in CHIP during the continuous eligibility period if a family did not pay their premiums; this exception to continuous eligibility was not available in Medicaid. On February 1, 2024, the state of Florida filed a lawsuit against HHS challenging the implementation of the law, asserting states should be allowed to terminate CHIP coverage (during the 12-month period) when premium payments are not made.
Under current law, states cannot provide continuous eligibility for adults without a Section 1115 waiver submitted to the federal government. States cannot require a renewal process for Medicaid coverage for adults who are eligible based on income more than once every 12 months. While states may conduct renewals for individuals who qualify for Medicaid based on age or disability more than once every 12 months, most states conduct annual renewals for these groups. However, because states cannot guarantee continuous eligibility for adults absent a waiver, adults may lose coverage if there are “changes in circumstance,” including changes in family income, during the year. Enrollees are required to report changes in circumstances, and some states conduct periodic electronic data matches between renewal periods to identify changes in circumstance.
Continuous eligibility has been shown to reduce Medicaid disenrollment and “churn” rates. Churn occurs when individuals temporarily lose Medicaid coverage and then re-enroll within a short period of time suggesting they are experiencing short-term changes in income or difficulty completing the renewal process. When individuals churn on and off coverage, the gaps in coverage may limit access to care or lead to delays in getting needed care, which can be especially problematic for young children who receive frequent screenings and check-ups. Research has found continuous eligibility for Medicaid is associated with improved child health. While continuous eligibility increases coverage costs due to longer average eligibility periods, there are also administrative costs associated with disenrolling individuals and then subsequently processing new applications.
How are states using 1115 waivers to provide extended continuous eligibility for children?
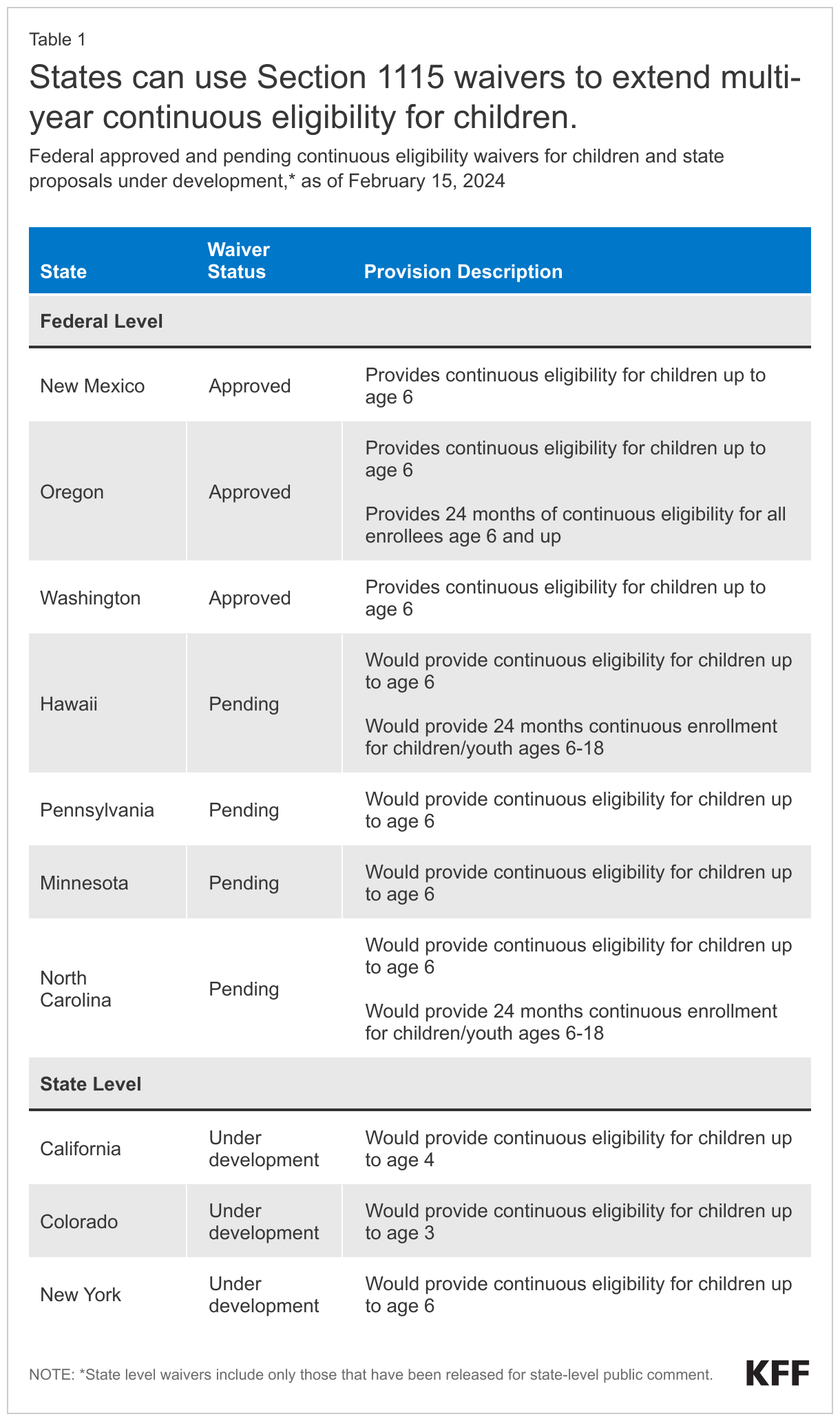
As of February 15, 2024, three states have approved Section 1115 demonstration waivers to provide multi-year continuous eligibility to children (Table 1). Section 1115 waivers allow states to obtain federal approval to operate Medicaid programs in ways that differ from federal standards and requirements. In September 2022, CMS approved Oregon’s waiver to implement continuous eligibility for children from birth to age six as well as 24 months of continuous eligibility for nearly all enrollees ages six and older. Since then, CMS has approved multi-year continuous eligibility requests for children in Washington and New Mexico. Hawaii, Minnesota, North Carolina, and Pennsylvania have requests pending with CMS.
A number of states are developing waivers to provide multi-year continuous eligibility to children. Several states have waiver proposals under development that have recently been released for state-level public comment (California, Colorado, and New York) that include multi-year continuous eligibility for children (Table 1). Other tracking shows state activity, including legislation directing the state Medicaid agency to seek approval for multi-year continuous eligibility for children, in Illinois, Ohio and the District of Columbia. In December 2023, growing concern over loss of Medicaid coverage for children prompted federal officials to issue additional guidance with strategies to protect coverage; one strategy CMS highlighted in its guidance is providing multi-year continuous eligibility for children through Section 1115 demonstration authority.
What options do states have to provide continuous eligibility for adults?
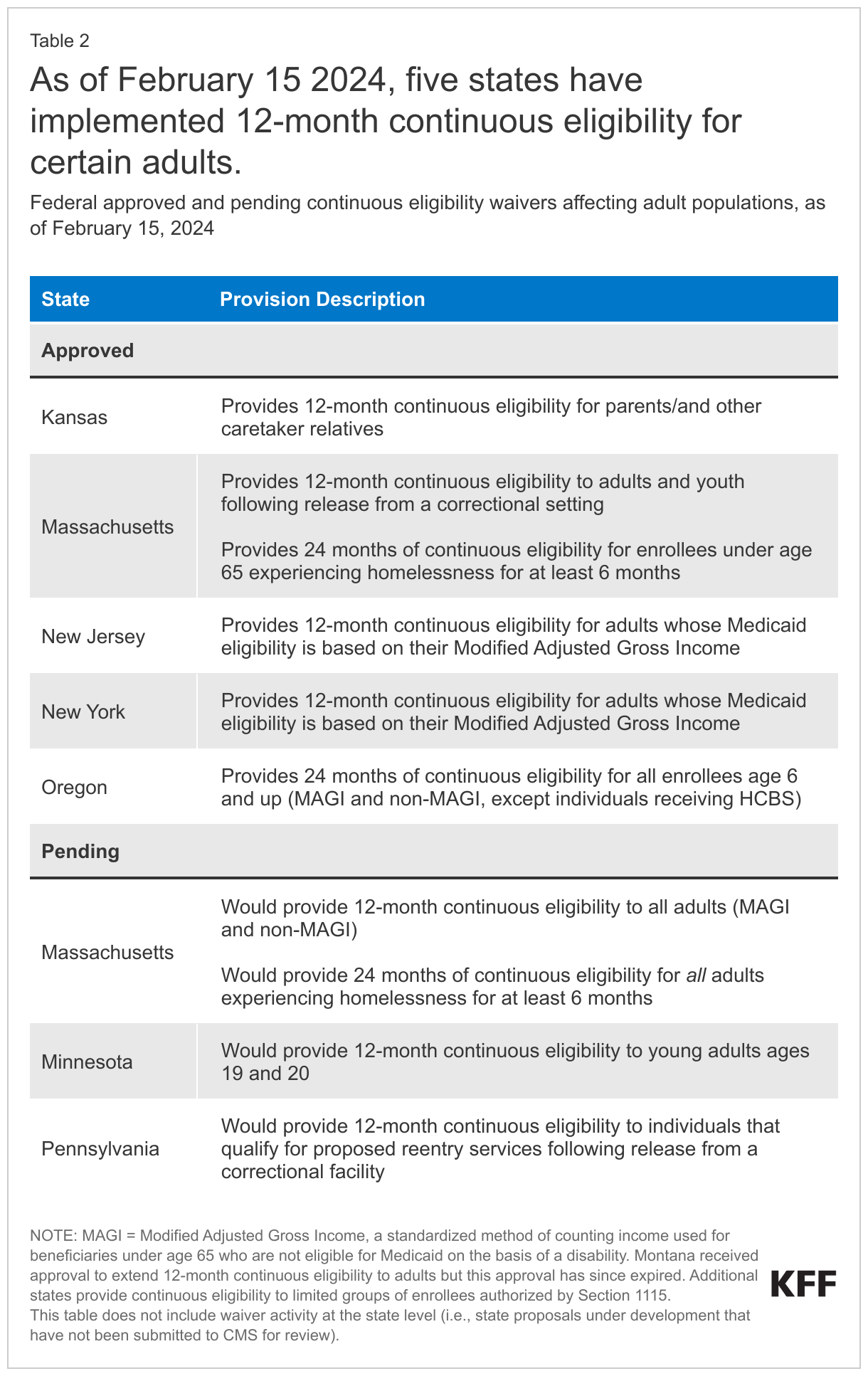
As of February 15, 2024, five states have approved Section 1115 waivers to provide varying lengths of continuous eligibility to certain adults (Table 2). Oregon provides 24 months of continuous eligibility to nearly all enrollees over age six. New York and New Jersey provide 12-month continuous eligibility to all income-eligible Medicaid adults. Kansas provides 12-month continuous eligibility to parents and caretaker relatives. Massachusetts provides 12-month continuous eligibility for individuals following release from a correctional institution and 24-month continuous eligibility for individuals under age 65 experiencing homelessness for at least 6 months; however, the state is seeking CMS approval to expand 12-month continuous eligibility to all adults (including those eligible based on income, age, or disability status) and 24 months of continuous eligibility to all adults experiencing homelessness. Minnesota is seeking to provide 12-month continuous eligibility to young adults ages 19 and 20, and Pennsylvania is seeking to provide 12-month continuous eligibility to individuals that qualify for proposed reentry services following release from a correctional facility.
Looking Ahead
Experience during the pandemic demonstrated that continuous enrollment can ensure stable coverage and reduce churn. While increased enrollment may result in increased overall costs, the policy can also improve health outcomes and potentially lead to some longer-term savings due to less fragmented care. While the unwinding of the pandemic-era continuous enrollment provision is leading to high rates of procedural disenrollments and is expected to increase the number of people who are uninsured longer term, mandatory 12-month continuous eligibility for children as well as new continuous eligibility policies that some states are pursuing through 1115 waivers can help to provide more stable coverage once the unwinding period ends.