Medicaid and the Elderly
Long-Term Care Spending
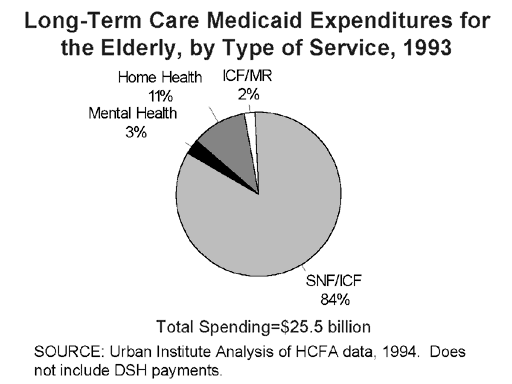
In 1993, Medicaid spent $25.5 billion for long-term care services for elderly beneficiaries (Figure 5). This represents 58 percent of the $44 billion Medicaid spent on long-term care services for all population groups. The majority of spending was for care delivered in nursing facilities (84 percent) and ICFs-MR (2 percent). The remaining 14 percent of Medicaid long-term care spending went towards community-based care, including 3 percent for mental health services and 11 percent for home health and personal care services.
Medicaid plays a fundamental role for institutionalized people and provided nursing home payments on behalf of 1.4 million elderly people in 1993. Often in nursing homes due to severe physical or cognitive limitations, nursing home residents tend to be over 80, female, white, and without a spouse in the community. Most have few choices available to them, and the need for continuous care and monitoring makes remaining in the community unaffordable and impractical.
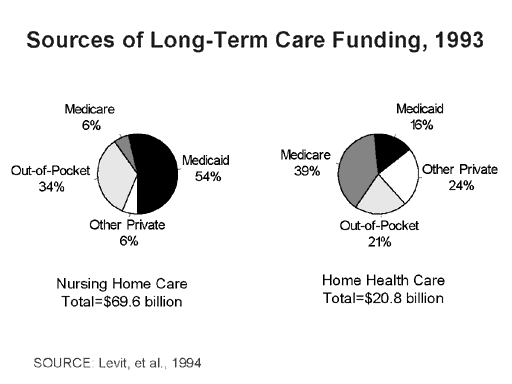
Medicaid is essentially the only public financing program for long-term care services and accounts for 52 percent of overall nursing home payments and the vast majority of all public spending for these services. In 1993, a total of $90 billion was spent on long-term care in the U.S. for people of all ages, with $70 billion spent on nursing home care and $21 billion on care in the community (Figure 6). Medicaid pays for 16 percent of home health and community-based long-term care. Private payments, primarily out-of-pocket spending by the elderly and their families, account for a major share of long-term care financing.
Less than 5 percent of elderly people have private long-term care insurance. The relatively low penetration of private long-term care policies among the elderly is attributable to two factors. First, premiums can be extremely costly for people who are already 65 and older living on fixed incomes, typically ranging from $650 to $4,200 per year depending on the age when purchased. Second, many elderly people are prohibited from purchasing private long-term care insurance because of a pre-existing condition or disability.
Medicare was not designed to be a long-term care program and provides only minimal long-term care services. In general, Medicare’s home health and nursing home benefits are limited to skilled, rehabilitation-oriented care, with the number of days in a Skilled Nursing Facility (SNF) limited explicitly to a maximum of 100 days. Medicare covers 9 percent of total nursing home expenditures and accounts for over one-third of total home health expenditures. Custodial or personal care services are generally not covered by Medicare, leaving Medicaid as the principal public program to provide these services.
Applying Beneficiaries’ Financial Resources to the Cost of Nursing Home Care
Nursing home care is expensive, with annual costs ranging from $30,000 to $50,000 or higher in some areas of the country. Regardless of whom it affects, nursing home care is a catastrophic expense that is likely to impoverish most middle- and lower-income persons. Medicaid is a means-tested program and, unlike insurance, provides assistance only when financial resources are exhausted. An elderly person must deplete almost all of their assets and apply all of their income, except for a small personal allowance, toward the cost of nursing home care before Medicaid will pay for services. Under the spousal impoverishment provision in the Medicare Catastrophic Coverage Act (MCCA) of 1988, a spouse of a nursing home resident is allowed to keep more income and assets than was previously permitted. Protected assets for spouses range across states from $14,964 up to a maximum of $74,820 and the minimum protected income is 150 percent of the poverty level.
Because the means-tested program is almost always the sole alternative to spending personal funds for nursing home care, some higher-income persons receive assistance by transferring their resources to establish eligibility. Although this situation has attracted attention, the magnitude of this phenomenon has never been well documented. The Omnibus Budget Reconciliation Act of 1993 (OBRA 93) tightened eligibility rules to ensure that nonpoor elderly persons apply their resources toward the cost of care before Medicaid pays for long-term care services. It requires states to delay Medicaid eligibility for institutionalized persons who dispose of assets for less than fair market value during the three years prior to institutionalization; counts trusts as available to cover the cost of care within five years of institutionalization; and mandates estate recovery to cover Medicaid’s long-term care costs. States also have the option to use these rules to delay eligibility for disabled persons in the community before Medicaid will provide assistance for home- and community-based services. These efforts have made it more difficult for elderly people to receive coverage for Medicaid long-term care services. In the absence of adequate private financing alternatives, setting appropriate limits on Medicaid’s ability to help individuals and families with long-term care will continue to be a source of tension in program policy and spending.
Medicaid Payments to Nursing Homes
Medicaid payments for nursing home care are a large component of Medicaid spending, accounting for 20 percent of total expenditures. Nursing home payment levels will become increasingly important as state Medicaid programs search for ways to constrain spending. The Boren Amendment, enacted under the Omnibus Budget Reconciliation Act of 1980 (OBRA 80), permitted states to move from cost-based reimbursement for nursing homes to set payment rates that are “reasonable and adequate” to meet the costs of “efficiently and economically” operated facilities, but did not specify methods or rates. State Certificate of Need (CON) programs, which enabled states to limit the number of nursing home beds, coupled with increased state flexibility in setting payment rates, helped states control the rate of nursing home spending during the 1980s. Recently, providers have used the Boren Amendment provisions to sue state Medicaid agencies, arguing that Medicaid payment rates are inadequate to meet the cost of operating nursing facilities and to accommodate the changes being implemented as part of nursing home reform.
Nursing Home Quality Reform
The Omnibus Budget Reconciliation Act of 1987 (OBRA 87) established protections for nursing home residents in response to Congressional concern about the quality of nursing home care and findings described in a 1986 Institute of Medicine report detailing an unsatisfactory level of care provided by nursing homes. Effective in October 1990, these reforms established requirements for providing care to Medicare and Medicaid beneficiaries related to scope of services, staffing levels and qualifications, residents’ rights, and the physical environment. Nursing facilities must comply with these requirements in order to receive reimbursement from Medicare and Medicaid.
Medicaid Coverage of Community-Based Long-Term Care
Medicaid has played an increasingly important role in covering community-based services for the elderly population with disabilities. Medicaid pays for skilled home health care in all states and 28 states and the District of Columbia have elected to cover the optional benefit of personal care in the home. Through home- and community-based waivers, states have been able to design programs to provide services, such as personal care, homemaker services, and adult day care to specific populations. Many states have implemented innovative programs to deliver coordinated community services to foster independence and provide an alternative to nursing home care, but most programs are small in scope and serve only a small number of frail elderly people. In 1993, Medicaid spent $2.8 billion on these innovative programs under home- and community-based waivers, through which 300,000 people were served.
Finding ways to stimulate the development of home- and community-based alternatives will continue to be a pressing challenge in Medicaid. Although the share devoted to home- and community-based services has been steadily increasing, Medicaid spending on long-term care continues to be directed primarily toward nursing home care. Of total Medicaid long-term care spending in 1993, $6.7 billion (15 percent) went toward community-based care (including skilled home health care, personal care, and home- and community-based waiver services), with most states spending between 5 and 25 percent (Figure 7).
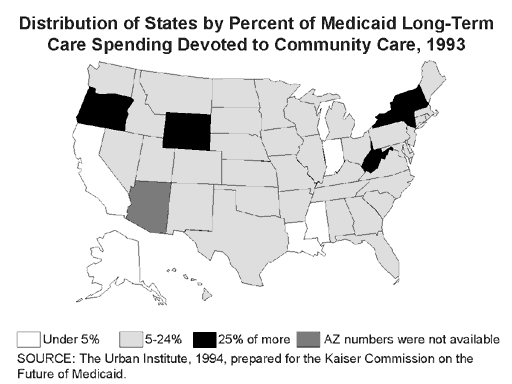
Six states — New Hampshire, New York, Oregon, Vermont, West Virginia, and Wyoming