Analysis: For Patients with Large Employer Coverage, About 1 in 6 Hospital Stays Includes an Out-of-Network Bill
Emergency Room, Mental Health and Substance Abuse Admissions Most Likely to Generate Out of-Network Claims
A new Kaiser Family Foundation analysis of medical bills from large employer plans finds that a significant share of inpatient hospital admissions includes bills from providers not in the health plan’s networks, generally leaving patients subject to higher cost-sharing and potential additional bills from providers.
Almost 18 percent of inpatient admissions result in non-network claims for patients with large employer coverage. Even when enrollees choose in-network facilities, 15 percent of admissions include a bill from an out-of-network provider, such as from a surgeon or an anesthesiologist. These bills potentially expose enrollees to high out-of-pocket costs if these providers charge enrollees more than their plans pay for services. This is typically referred to as “balance billing,” and can result in a “surprise” medical bill if a patient did not anticipate receiving care from an out-of-network provider. Health insurance plans also typically require higher patient cost-sharing for out-of-network claims.
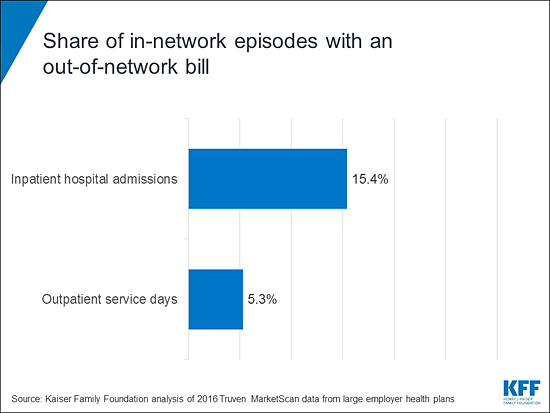
The analysis looks at inpatient admissions and outpatient services to examine how often they result in claims from providers that are not participating in an enrollee’s provider network.
For both inpatient admissions and outpatient services, use of an emergency room is associated with higher rates of out-of-network bills. Treatments for mental health and substance abuse also have a much higher chance of including a claim from an out-of-network provider, potentially reflecting difficulty in finding a participating provider.
The issue brief is available on the Peterson-Kaiser Health System Tracker, a partnership between the Peterson Center on Healthcare and the Kaiser Family Foundation that monitors the U.S. health system’s performance on key quality and cost measures.