Snapshots: Comparing Projected Growth in Health Care Expenditures and the Economy
The rising cost of health care is much in the news. Health costs continue to grow faster than national income and, despite research indicating that we the get good value for the increased spending, some policy makers and health analysts question whether governments and private employers can continue to finance the level of care that they do today. This paper illustrates the magnitude of savings that would be needed in order to bring health care cost growth closer to the rate of national income growth, and suggests that none of the usual policy options raised in health policy or political circles is likely to significantly close the gap between the growth of health spending and income.1
The Centers for Medicare and Medicaid Services (CMS) recently released projected health care expenditures for the 2005 through 2015 period.2 Total health expenditures are estimated to be $2.16 trillion in 2006, and are projected to rise to over $4 trillion in 2015. Per person health spending is $7,110 this year and is projected to increase to $12,320 by the end of the period.
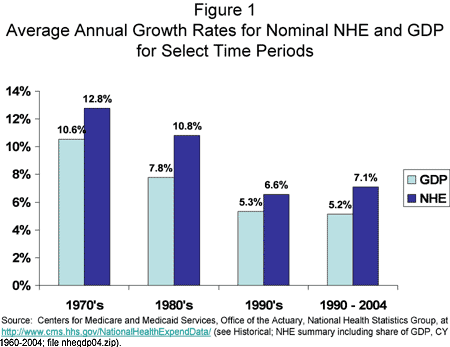
Health spending continues to increase much faster than the overall economy (i.e., gross domestic product, or GDP). Since 1970, health care spending has grown at an average annual rate of 9.9%, or about 2.5 percentage points faster than GDP.3 In recent decades, the growth rates for health spending and GDP have slowed, but health spending growth remains consistently above GDP growth (Figure 1). As a share of the economy, health care has risen from 7.2% of GDP in 1965 to over 16% of GDP today, and it is projected to be 20% of GDP just 10 years from now.4
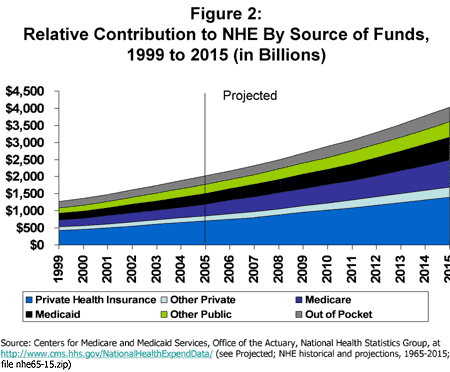
Although not a new phenomena, the rapid rate of growth in health spending relative to national income is raising concerns among policy makers and others as to whether our health care system is financially sustainable. On the public benefit side, spending growth, combined with the aging of the population, has raised concerns about the longer-term affordability of the Medicare and Medicaid programs.5 For private health insurance, rapid premium increases have focused attention on the affordability of coverage for employers and workers as well as on the impact that paying for health care has on the international competitiveness of U.S. businesses. As Figure 2 shows, health cost growth is an issue for both private and public third-party payers – with each sector facing similar growth patterns into the future.6
This renewed attention to expenditure growth, along with reports such as the Institutes of Medicine’s “To Err is Human: Building a Safer Health Care System” that demonstrate the amount of waste and inappropriate care with the U.S. health care system, have spurred a considerable number of cost containment and quality improvement efforts. For payers, efforts have focused on improving medical information technology, disease management, better identification and management of high cost and chronically ill patients, the introduction of wellness programs and incentives, initiatives to reward providers for appropriate and high quality care ( sometimes referred to as “pay for performance”), reducing payment rates to providers, and instituting higher cost-sharing. Most recently, consumer directed approaches use increased out-of-pocket responsibility, combined with tax incentives and more information on health care alternatives, to encourage consumers to be more cost conscious and better informed when making health care decisions. On the supply side, health care institutions and professionals are investing in medical technology (such as electronic medical records), developing systems to reduce medical errors, and participating in programs that reward efficiency and quality. Many states additionally have enacted laws to reduce medical malpractice judgments in order to reduce premium burdens on providers and lower overall costs.
Although many of these efforts may lead to efficiency and quality gains, none would appear to be of a scale to have any meaningful impact on the overall cost picture. CMS estimates that health spending between 2006 and 2015 will grow at an average annual growth rate of almost 7.2% (2.3 percentage points faster than average annual GDP growth), with total health spending in that period of about $30.3 trillion. If we began next year trying to hold health care cost growth to the current project growth rate for GDP (i.e., slowing growth in health costs to an average of 4.9% annually starting in 2007) we would need to lower health spending by over $3 trillion over the 2007 to 2015 that period (the area between the red and green lines in Figure 3.)7 These savings would represent about 10.8% of projected total health spending over the period, or an average annual reduction of about $340 billion relative to the projected level of spending.
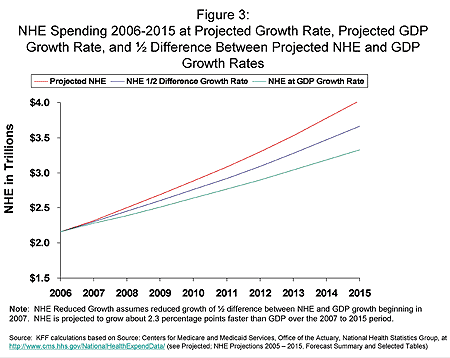
Splitting the difference between projected NHE growth and GDP growth – which would mean lowering health spending growth on average to about 6 percent per year — would lower spending by almost $1.6 trillion between 2007 and 2015, (the area between the red and blue lines in Figure 3).8 This almost $1.6 trillion represents about 5.6% of projected spending over the 2007 to 2015 period, or an average reduction of about $175 billion each year relative to the projected level of spending over the period. Reducing projected costs by this amount would lower projected expenditures per person by about $1,100 in 2015 (Figure 4).
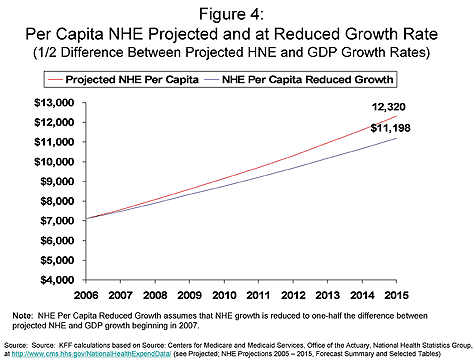
Systemically lowering health cost growth is a complex task. Some actions can lower what we currently spend, but they may not affect how fast spending grows from the new, lower level that is achieved. Cutting provider payments or reducing administrative costs, such as moving from paper to electronic claims, fall into this category. Programs designed to reduce inappropriate treatments and resource use, such as pay for performance initiatives, and changes in cost sharing, such as higher deductibles and coinsurance levels, also would largely fall into this category.9 These actions, while potentially valuable, are directed primarily at the amount that we are currently spending as opposed to why that amount grows so rapidly each year. For example, we know that there is substantial waste in our health care system (which potentially could be reduced through policies such greater use of evidence-based medicine), but there is no real evidence that the level of waste is growing substantially each year.
Many economists and health policy analysts argue that the development and adoption of new medical technology (e.g., drugs, devises, treatments and techniques) is responsible for a substantial portion of the growth in health expenditures.10 Health care is the type of good that we want more of as the nation prospers and becomes wealthier and health care suppliers, providers and institutions have been successful in providing an increasing variety of new products and services to meet the societal demand.11 This steady advance of medical capacity means that we have a growing stock of medical interventions that can potentially address a growing list of health care issues and conditions. To address the impact of medical technology on spending, policies would need to constrain the introduction and adoption of new medical products and services to a much greater extent than we do today. An example would be a policy that provides payment through insurance (public and private) only for new medical interventions that demonstrate benefits that exceed their costs. Limiting the supply of new imaging devices is a far more limited example of such a policy.
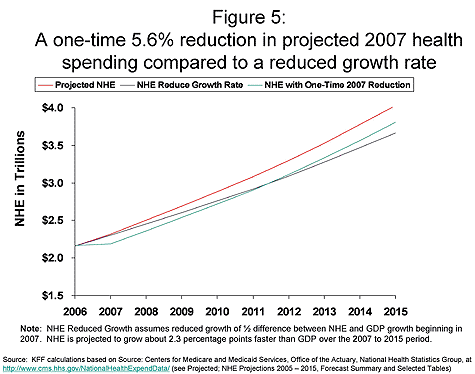
Policymakers considering policies to address cost growth need to keep in mind the long term impacts of the types of policies that they are considering. Figure 5 demonstrates the trajectory of two types of policies – one that produces a one-time cost reduction but does not affect the rate of growth, and the other that systematically constrains growth – both of which achieve a similar aggregate reduction over the time period. The green line shows the impact on projected NHE of a policy that would reduce overall spending by 5.6%12 in 2007, with future growth at the same rate as projected NHE. The blue line shows the impact of a policy that reduces the annual growth rate by one-half of the difference between the projected NHE and GDP growth rates, or to about 6% annually. In both cases, projected NHE would be reduced by the same total amount over the 2007 to 2015 period (almost $1.6 trillion). The first policy – the one-time 5.6% reduction – produces more savings in the first part of the period, but by 2015 both annual costs and the trajectory for future costs are higher than under the reduced growth rate scenario.
There is no consensus about how much of the economy can or should be dedicated to health care, but policy makers and commentators continue to suggest that cannot afford to continue on our current course for a long period into the future. How we would change the projected trajectory, however, is far from clear. Many of the policies aimed at improving efficiency and reducing unnecessary care, such as disease management, wellness, and pay for performance programs are already underway and their impacts are anticipated in the baseline. Even if these policies do better than anticipated, they are not designed to produce the magnitude of savings needed to change the path of NHE. Consumer directed health care approaches, if accompanied by significant increases in out-of-pocket liability, have the potential to make a dent in cost growth, at least in the short term, but there is little reason to believe that these approaches would systematically affect the introduction of new medical technologies in ways that would slow growth over the longer term unless cost sharing was set a levels that put the price of many new goods and services out of the reach of a meaningful part of the population. Policies that would significantly constrain medical technology growth have not been part of the political or public discussion over health care cost growth; implementing systemic limits on what we would pay for (or allow to be provided to patients) would require a coordinated public intervention in health spending decisions or an unprecedented level of cooperation among public and private plans, neither of which seem likely in the current deregulatory environment.
Policy makers and others concerned about the financial sustainability of our health care system will need to understand and come to terms with the level of policy intervention that would be needed to meaningfully reduce the portion of our national income devoted to health care. Finding even small amounts of savings in either public or private programs has been very difficult for policymakers; interventions that would reduce spending by hundreds of billions or even a trillion dollars over the foreseeable future would require a fundamental rethinking of how we pay for health care.
Notes:
1. This paper talks about the dollar amounts of health spending that would occur under current projections and if health care costs were to grow more closely to the growth rate for the economy as a whole. The purpose is to show dollar magnitude of the difference and the challenge facing the nation if policy makers want to reduce appreciably the amount of national income that is spent on health care. However, because health care is such a large component of the gross domestic product (GDP), any efforts to significantly slow health care expenditure growth would also affect GDP growth. We have not tried to deal with that interaction here.
2. C. Borger et al., “Health spending projections through 2015: changes on the horizon,” Health Affairs Web Exclusive, March/April 2006; 25(2): 61-73.
3. Centers for Medicare and Medicaid Services, Office of the Actuary, National Health Statistics Group, at http://www.cms.hhs.gov/NationalHealthExpendData/ (see Historical; NHE summary including share of GDP, CY 1960-2004; file nhegdp04.zip).
4. Borger et al., op cit; CMS National Health Statistics Group, NHE summary including share of GDP, op cit.
5. Although it gets less attention, federal and state governments also subsidize a substantial share of private health spending through tax exclusions for private health insurance. See L. Berman, et al., “Tax incentives for health insurance,” Discussion Paper No. 12, Washington D.C.: Urban-Brookings Tax Policy Center, May 2003, http://www.urban.org/UploadedPDF/310791_TPC_DP12.pdf. Analysis by the Lewin Group suggests that federal tax exclusions for health insurance were almost $190 billion in 2004. J. Sheils and R. Haught, “The cost of tax-exempt health benefits in 2004,” Health Affairs Web Exclusive, February 25, 2004.
6. See Centers for Medicare and Medicaid Services, Office of the Actuary, National Health Statistics Group, at http://www.cms.hhs.gov/NationalHealthExpendData/ (see Projected; NHE historical and projections, 1965-2015; file nhe65-15.zip).
7. We assume that the reduced growth rate begins in 2007.
8. We assume that the reduced growth rate begins in 2007.
9. For instance, see: Newhouse, JP. “Medical care costs: how much welfare loss?” Journal of Economic Perspectives, 1992; Vol 6 (3): 3-21; and Swartz, WB. “The inevitable failure of cost containment strategies: why they can provide only temporary relief,” Journal of the American Medical Association, January 9, 1987; Vol 257 (2): 220-24. Large changes in cost sharing could have more of a systemic impact on costs to the extent that they encourage or discourage the development or diffusion of new medical technologies (drugs, devices, treatments) over time.
10. Newhouse, JP. “Medical care costs: how much welfare loss?” Journal of Economic Perspectives, 1992; Vol 6 (3): 3-21; Zweifel, P. “Technological change in health care: why are opinions so divided?” Managerial and Decision Economics, 1984; 5(3): 177-82;Cutler, DM. “Technology, health costs, and the NIH” (Paper presented at the National Institutes of Health Economic Roundtable on Biomedical Research, Bethesda, Maryland, November 1995); and Freeland, MS, Heffler, SK, Smith, SD. “The impact of technological change on health care cost increases: A brief synthesis of the literature,” Office of the Actuary, Health Care Financing Administration, June 1998.
11. The relationship of health care expenditure growth to national income growth is observed throughout the world. See Newhouse, JP. “Medical care expenditure: a cross-national survey,” Journal of Human Resources, 1977; Vol 12: 115-25; “Projecting OECD health and long-term care expenditures: what are the main drivers?” Economics Department Working Paper No. 477, Organisation for Economic Co-operation and Development, 2006. Available at www.oecd.org/eco.
12. A 5.6% reduction in projected NHE in 2007 would be equal to about $109 billion.