2017 Employer Health Benefits Survey
Section 8: High-Deductible Health Plans with Savings Option
To help cover out-of-pocket expenses not covered by a health plan, some firms offer high deductible plans that are paired with an account that allows enrollees to use tax-preferred savings to pay plan cost sharing and other out-of-pocket medical expenses. The two most common are health reimbursement arrangements (HRAs) and health savings accounts (HSAs). HRAs and HSAs are financial accounts that workers or their family members can use to pay for health care services. These savings arrangements are often (or, in the case of HSAs, always) paired with health plans with high deductibles. The survey treats high-deductible plans paired with a savings option as a distinct plan type – High-Deductible Health Plan with Savings Option (HDHP/SO) – even if the plan would otherwise be considered a PPO, HMO, POS plan, or conventional health plan. Specifically for the survey, HDHP/SOs are defined as (1) health plans with a deductible of at least $1,000 for single coverage and $2,000 for family coverage27 offered with an HRA (referred to as HDHP/HRAs); or (2) high-deductible health plans that meet the federal legal requirements to permit an enrollee to establish and contribute to an HSA (referred to as HSA-qualified HDHPs).28
PERCENTAGE OF FIRMS OFFERING HDHP/HRAS AND HSA-QUALIFIED HDHPS
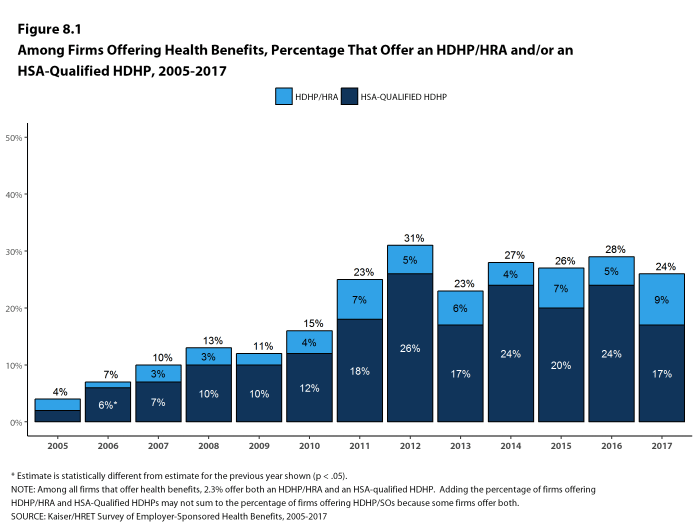
- Twenty-four percent of firms offering health benefits offer an HDHP/HRA, an HSA-qualified HDHP, or both. Among firms offering health benefits, 9% offer an HDHP/HRA and 17% offer an HSA-qualified HDHP [Figure 8.1]. The percentage of firms offering an HDHP/SO is similar to last year.
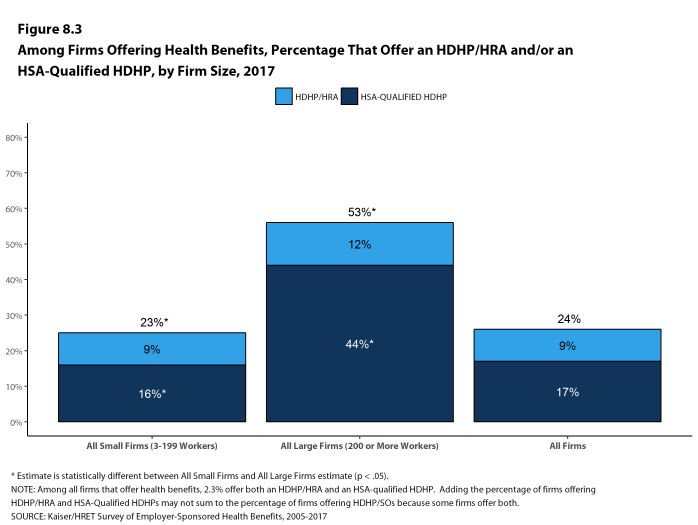
- Large firms (200 or more workers) are more likely than small firms (3-199 workers) to offer an HDHP/SO (53% vs. 23%). [Figure 8.3].
Figure 8.1: Among Firms Offering Health Benefits, Percentage That Offer an HDHP/HRA And/Or an HSA-Qualified HDHP, 2005-2017
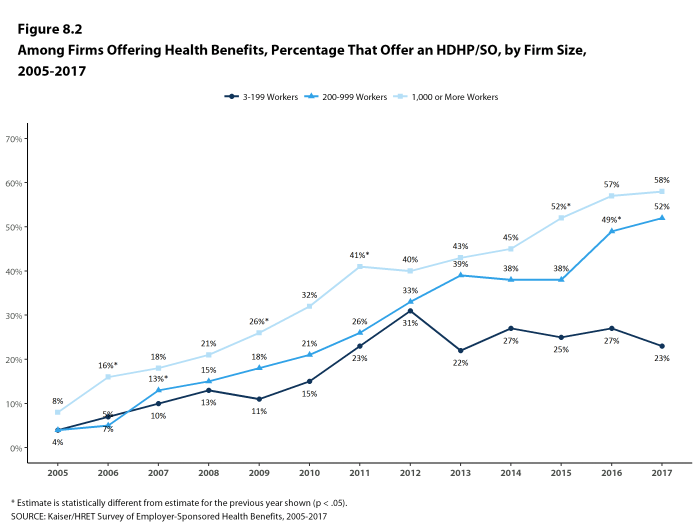
Figure 8.2: Among Firms Offering Health Benefits, Percentage That Offer an HDHP/SO, by Firm Size, 2005-2017
ENROLLMENT IN FIRMS OFFERING HDHP/HRAS AND HSA-QUALIFIED HDHPS
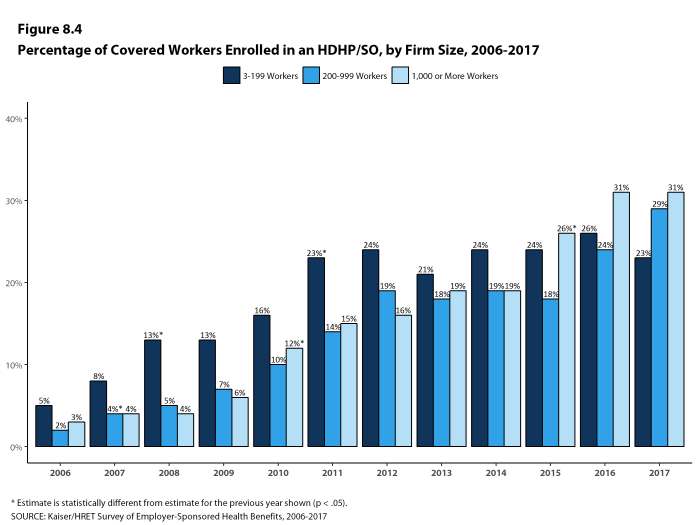
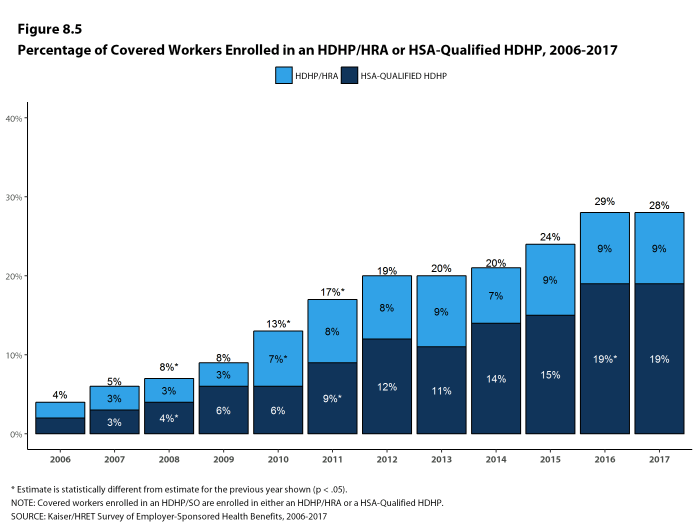
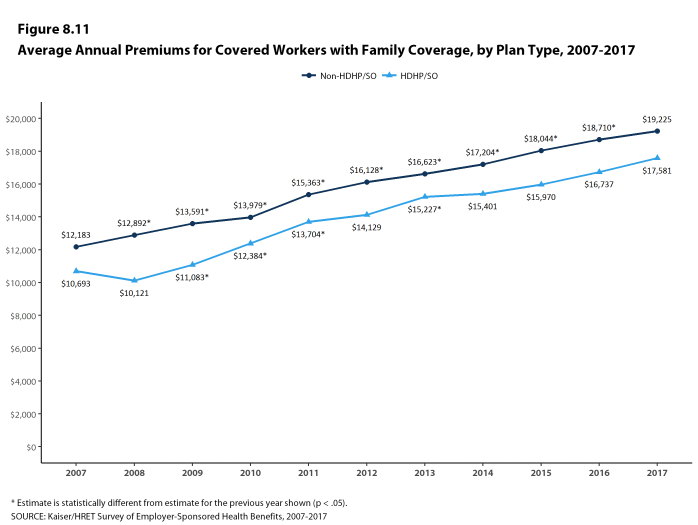
- Enrollment in HDHP/SO plans has increased over the last five years, from 19% of covered workers in 2012 to 28% in 2017.
- Nine percent of covered workers are enrolled in HDHP/HRAs and 19% of covered workers are enrolled in HSA-qualified HDHPs in 2017. These percentages are the same as the percentages last year [Figure 8.5].
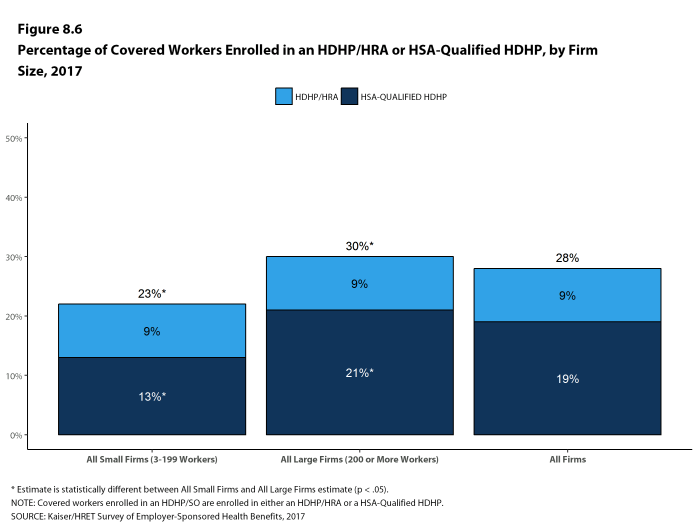
- A higher percentage of covered workers in large firms is enrolled in HDHP/SOs than in small firms (30% vs. 23%) [Figure 8.6].
PLAN DEDUCTIBLES
- As expected, workers enrolled in HDHP/SOs have higher deductibles than workers enrolled in HMOs, PPOs, or POS plans.
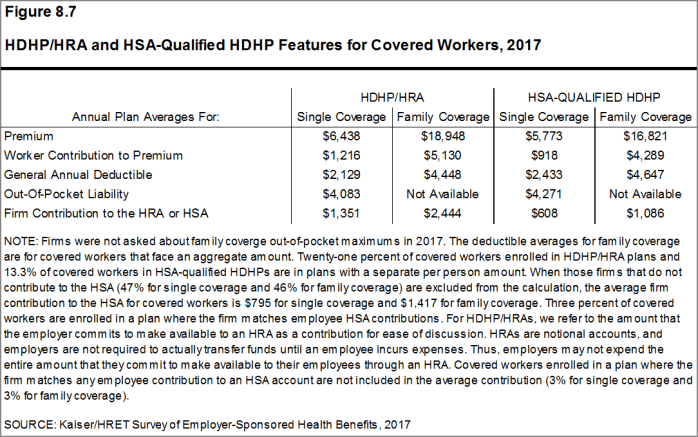
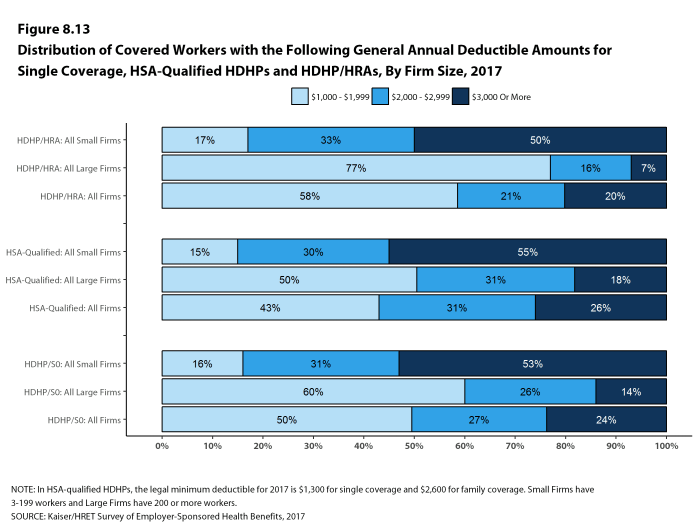
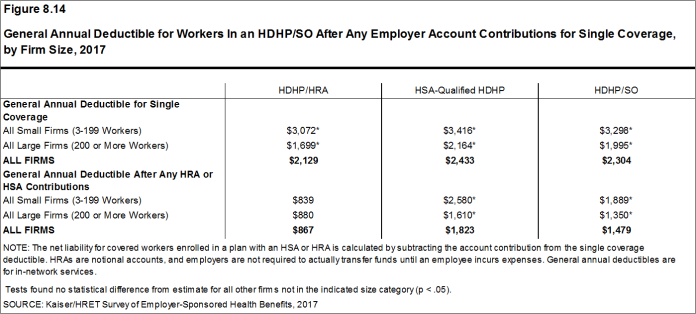
- The average general annual deductible for single coverage is $2,129 for HDHP/HRAs and $2,433 for HSA-qualified HDHPs [Figure 8.14]. These averages are similar to the amounts reported in recent years. There is wide variation around these averages: 19% of covered workers enrolled in an HDHP/SO are in a plan with a deductible of $1,000 to $1,499 while 24% are in a plan with a deductible of $3,000 or more [Figure 8.13].
- The survey asks firms whether the family deductible amount is (1) an aggregate amount (i.e., the out-of-pocket expenses of all family members are counted until the deductible is satisfied), or (2) a per-person amount that applies to each family member (typically with a limit on the number of family members that would be required to meet the deductible amount) (see Section 7 for more information).
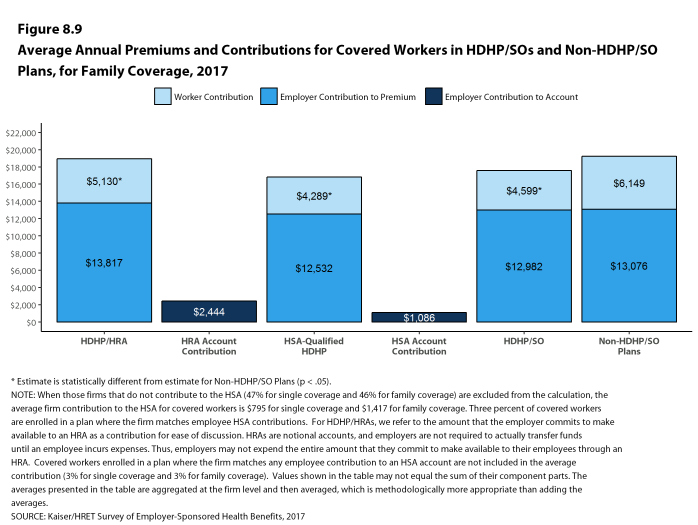
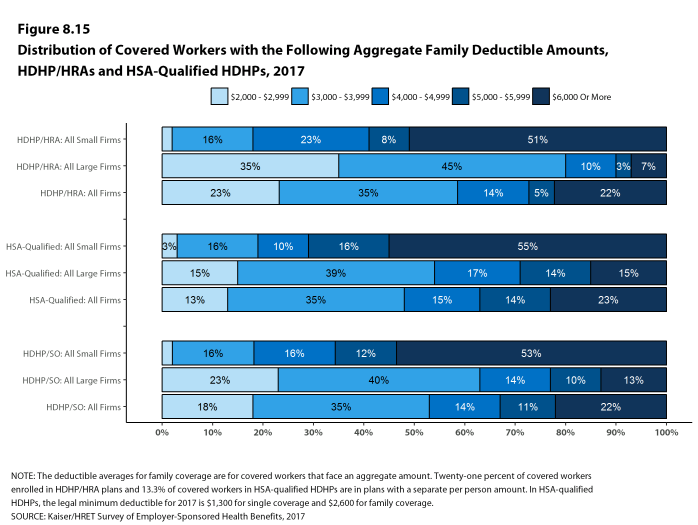
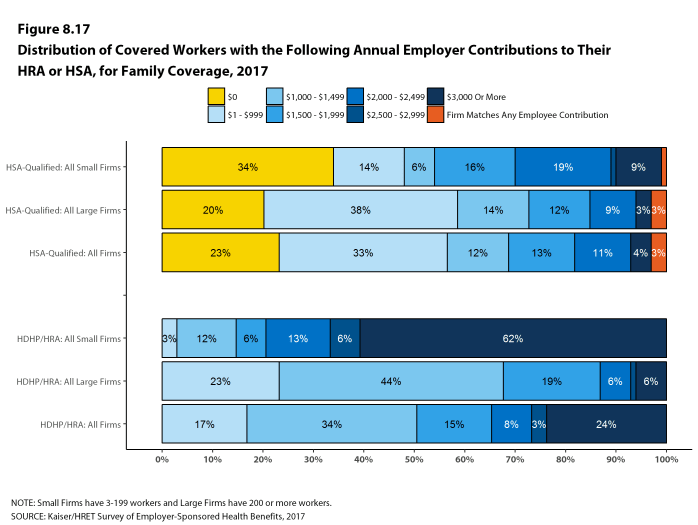
- The average aggregate deductibles for workers with family coverage are $4,448 for HDHP/HRAs and $4,647 for HSA-qualified HDHPs [Figure 8.7]. As with single coverage, there is wide variation around these averages for family coverage: 18% of covered workers enrolled in HDHP/SOs with an aggregate family deductible have a deductible of $2,000 to $2,999 while 22% have a deductible of $6,000 dollars or more [Figure 8.15].
Figure 8.13: Distribution of Covered Workers With the Following General Annual Deductible Amounts for Single Coverage, HSA-Qualified HDHPs and HDHP/HRAs, by Firm Size, 2017
Figure 8.14: General Annual Deductible for Workers In an HDHP/SO After Any Employer Account Contributions for Single Coverage, by Firm Size, 2017
OUT-OF-POCKET MAXIMUM AMOUNTS
- HSA-qualified HDHPs are legally required to have an annual out-of-pocket maximum of no more than $6,550 for single coverage and $13,100 for family coverage in 2017. Non-grandfathered HDHP/HRA plans starting in 2017 are required to have out-of-pocket maximums of no more than $7,150 for single coverage and $14,300 for family coverage. Virtually all HDHP/HRA plans have an out of pocket maximum for single coverage in 2017.
- The average annual out-of-pocket maximum for single coverage is $4,083 for HDHP/HRAs and $4,271 for HSA-qualified HDHPs [Figure 8.7].
COST-SHARING FOR OFFICE-VISITS
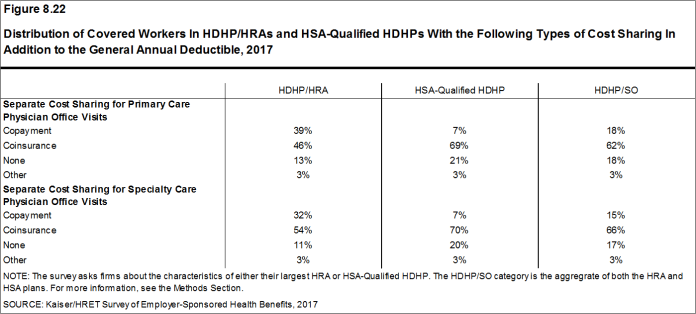
- The cost-sharing pattern for primary care office visits differs for workers enrolled in HDHP/SOs. Thirty-nine percent of covered workers in HDHP/HRAs have a copayment for primary care physician office visits compared to 7% enrolled in an HSA-qualified HDHP [Figure 8.22]. Workers in other plan types are much more likely to face copayments than coinsurance for physician office visits (see Section 7 for more information).
Figure 8.22: Distribution of Covered Workers In HDHP/HRAs and HSA-Qualified HDHPs With the Following Types of Cost Sharing In Addition to the General Annual Deductible, 2017
- Health Reimbursement Arrangements (HRAs)
- are medical care reimbursement plans established by employers that can be used by employees to pay for health care. HRAs are funded solely by employers. Employers may commit to make a specified amount of money available in the HRA for premiums and medical expenses incurred by employees or their dependents. HRAs are accounting devices, and employers are not required to expend funds until an employee incurs expenses that would be covered by the HRA. Unspent funds in the HRA usually can be carried over to the next year (sometimes with a limit). Employees cannot take their HRA balances with them if they leave their job, although an employer can choose to make the remaining balance available to former employees to pay for health care. HRAs often are offered along with a high-deductible health plan (HDHP). In such cases, the employee pays for health care first from his or her HRA and then out-of-pocket until the health plan deductible is met. Sometimes certain preventive services or other services such as prescription drugs are paid for by the plan before the employee meets the deductible.
- Health Savings Accounts (HSAs)
- are savings accounts created by individuals to pay for health care. An individual may establish an HSA if he or she is covered by a “qualified health plan” –a plan with a high deductible (i.e., a deductible of at least $1,300 for single coverage and $2,600 for family coverage in 2017) that also meets other requirements. Employers can encourage their employees to create HSAs by offering an HDHP that meets the federal requirements. Employers in some cases also may assist their employees by identifying HSA options, facilitating applications, or negotiating favorable fees from HSA vendors. Both employers and employees can contribute to an HSA, up to the statutory cap of $3,400 for single coverage and $6,750 for family coverage in 2017. Employee contributions to the HSA are made on a pre-income tax basis, and some employers arrange for their employees to fund their HSAs through payroll deductions. Employers are not required to contribute to HSAs established by their employees but if they elect to do so, their contributions are not taxable to the employee. Interest and other earnings on amounts in an HSA are not taxable. Withdrawals from the HSA by the account owner to pay for qualified health care expenses are not taxed. The savings account is owned by the individual who creates the account, so employees retain their HSA balances if they leave their job.30
- There is no legal requirement for the minimum deductible in a plan offered with an HRA. The survey defines a high-deductible HRA plan as a plan with a deductible of at least $1,000 for single coverage and $2,000 for family coverage. Federal law requires a deductible of at least $1,300 for single coverage and $2,600 for family coverage for HSA-qualified HDHPs in 2017. See the Text Box for more information on HDHP/HRAs and HSA-qualified HDHPs.↩
- The definitions of HDHP/SOs do not include other consumer-driven plan options, such as arrangements that combine an HRA with a lower-deductible health plan or arrangements in which an insurer (rather than the employer as in the case of HRAs or the enrollee as in the case of HSAs) establishes an account for each enrollee. Other arrangements may be included in future surveys as the market evolves.↩
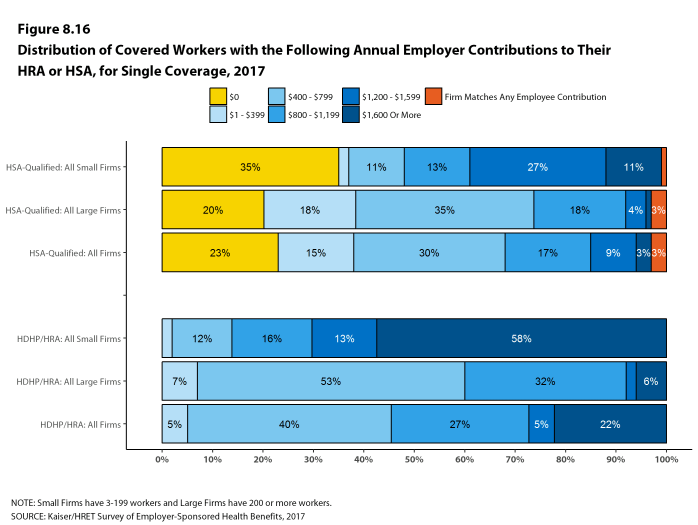
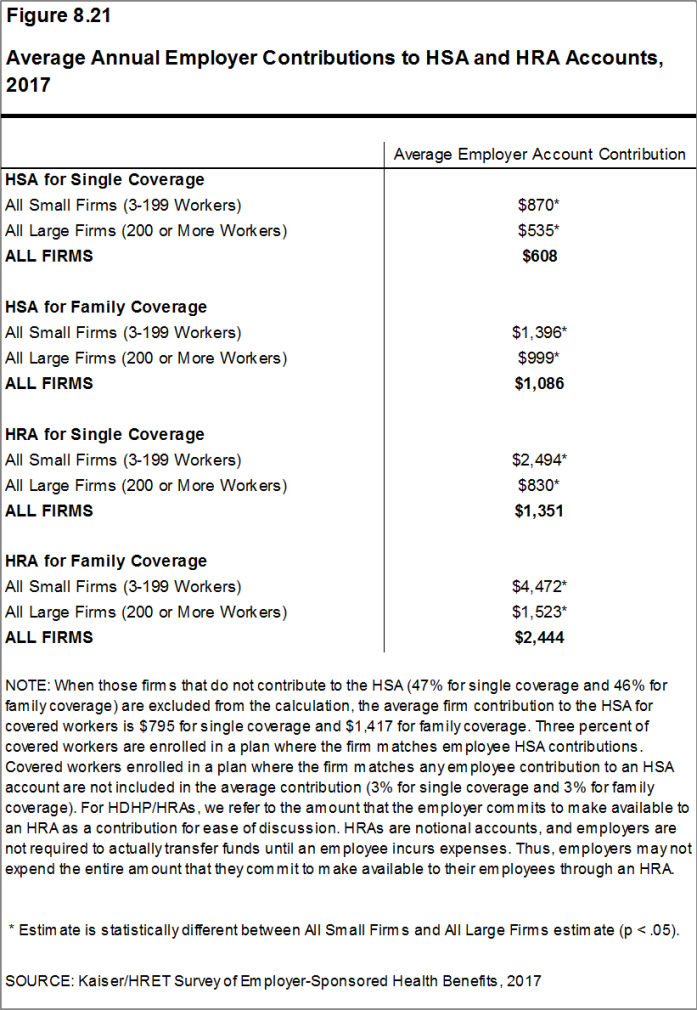
- The survey asks “Up to what dollar amount does your firm promise to contribute each year to an employee’s HRA or health reimbursement arrangement for single coverage?” We refer to the amount that the employer commits to make available to an HRA as a contribution for ease of discussion. As discussed, HRAs are notional accounts, and employers are not required to actually transfer funds until an employee incurs expenses. Thus, employers may not expend the entire amount that they commit to make available to their employees through an HRA. Some employers may make their HRA contribution contingent on other factors, such as completing wellness programs.↩
- See U.S. Department of the Treasury, Health Savings Accounts, available at http://www.irs.gov/pub/irs-drop/rp-14-30.pdf↩