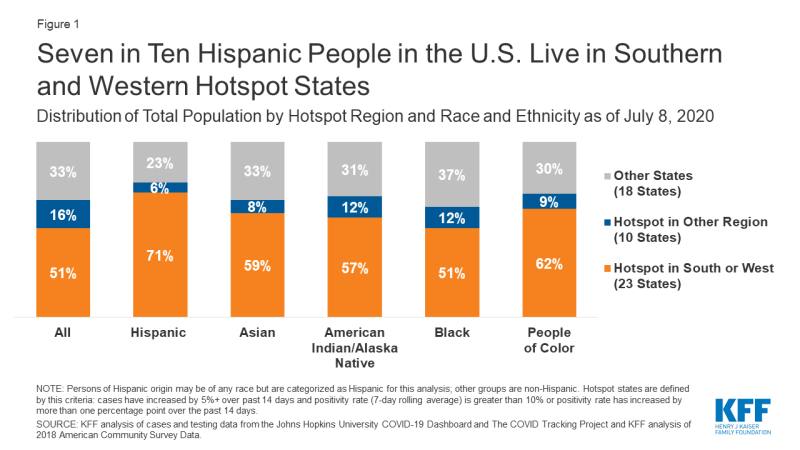
Growing COVID-19 Hotspots in the U.S. South and West will Likely Widen Disparities for People of Color
Samantha Artiga, Jennifer Tolbert, Jennifer Kates, Josh Michaud, and Kendal Orgera
Published:
The number of COVID-19 cases in the U.S. is expanding rapidly, particularly in many states in the South and West. While the locations of outbreaks continue to move across the country, surging in some states and falling in others, much of the recent case growth has been occurring in the South and West. As of July 8th, we identified 33 states as hotspots (experiencing recent increases in cases and an increasing positivity rate or positivity rate over 10%), 23 of which were in the South and West. The shifting surge in outbreaks to the South and West will likely exacerbate the disparate effects of COVID-19 for people of color, who already are facing a higher burden of cases, hospitalizations, and deaths as well as a larger economic toll compared to their White counterparts. Hispanic people may be particularly hard hit as outbreaks rise in these areas.
Just over half (51%) of people in the U.S. reside in these 23 Southern and Western hotspot states, but these states are home to seven in ten of all Hispanic individuals (71%) (Figure 1). Moreover, roughly six in ten Asian (59%) and American Indian and Alaska Native (AIAN) (57%) people live in these states, as do over half (51%) of Black people. Overall, nearly two-thirds of people of color (62%) reside in these states, compared to less than half of White people (43%).
In addition, people of color account for a larger share of the population compared to their share of the total U.S. population in a number of these states. For example, in 9 of the 23 Southern and Western hotspot states, Black people make up a larger share of the population compared to their share of the total U.S. population (12%). These states include Georgia (31%), Louisiana (32%), and Mississippi (38%), where more than three in ten residents are Black. AIAN people also make up a larger share of the population in 9 of these 23 states, including Montana (6%), New Mexico (9%), and Alaska (16%), compared to their share of the total U.S. population (<1%). Similarly, while 18% of the total U.S. population is Hispanic, they make up a higher share of the population in 7 of these 23 states, including roughly a third or more of the population in Arizona (32%), California (39%), Texas (40%), and New Mexico (49%). Asian people also account for a higher share of the population in Nevada (8%), Washington (9%), California (15%), and Hawaii (38%) compared to the U.S. overall (6%).
Moreover, within many of these states, COVID-19 has already disproportionately affected people of color. Based on data reported as of July 6, Black people accounted for a higher share of COVID-19 related deaths compared to their share of the population in 13 of these states that were reporting deaths by race/ethnicity. Similarly, Hispanic people made up a larger share of cases compared to their share of the population in 13 states, including in Tennessee and Arkansas, where their share of cases is over three times higher than their share of the population. There are also striking disparities for AIAN and Asian people in some of these states. For example, in Arizona, AIAN people made up 7% of cases and 16% of deaths compared to just 4% of the population and, in Nevada, Asian people made up 14% of deaths compared to 8% of the population.
The large number of people of color living in COVID-19 hotspots coupled with the already disproportionate impact for people of color will likely lead to further growth in disparities as the outbreak shifts to the South and West. Potential growing impacts for the large shares of Hispanic and Asian people living in these areas heighten the importance of providing information and services in linguistically and culturally appropriate ways and addressing potential fears that could make those who have an immigrant family member hesitant to access services. Prior to the pandemic, growing research showed that many immigrant families were increasingly fearful of accessing services, including health care services, due to recent immigration policy changes. Rising cases will likely compound the major challenges AIAN people already are facing due to the pandemic and widen disproportionate impacts for Black individuals, as these groups are at increased risk of experiencing serious illness if they contract the virus due to high rates of underlying health conditions. People of color also are at increased risk of exposure to the virus, face increased barriers to testing and treatment, and are more vulnerable to financial challenges due to the pandemic due to social and economic circumstances.
As discussed in previous work, the disparate impacts of COVID-19 mirror and compound existing racial and ethnic disparities in health and health care that are driven by broader underlying structural and systemic barriers, including racism and discrimination. For example, people of color are more likely to be uninsured, report poorer access to health care, and face increased economic and social challenges compared to their White counterparts. Further, 8 of these 23 hotspot states have not yet implemented the ACA Medicaid expansion to low-income adults, leaving a gap in coverage for poor adults in these states.
Together the findings point to the importance of prioritizing health equity as part of response and relief efforts and directing resources to communities who are at the highest risk and experiencing disproportionate effects. Such efforts include collecting data to monitor the impact across communities; working with trusted community members and leaders and providing information in linguistically and culturally appropriate ways to effectively reach individuals; making testing and care readily accessible within communities to facilitate access to services, including for those who are uninsured; and providing adequate resources and support to help prevent spread of the virus. At the same time, broader efforts to address systemic and structural barriers both within and outside the health care system remain pivotal to addressing the underlying health inequities that have been highlighted and exacerbated by the COVID-19 pandemic.