Pulling it Together: Small $ for HIV Prevention
It’s no secret that the response to the HIV epidemic domestically has not kept pace with the response to the global epidemic. And in an earlier column called America Has Gone Quiet on HIV/AIDS I wrote about the growing complacency towards the domestic epidemic revealed in our recent survey of the American people.
Last Friday, we released a new study with the National Alliance of State and Territorial AIDS Directors that documents the level of spending, state-by-state, for HIV prevention, looking at both federal and state funds combined that are administered by state and local health departments – where the rubber meets the road and HIV prevention is actually delivered in the U.S. The results were striking in two respects.
First, the overall level of spending for HIV prevention in the U.S. has been essentially flat since fiscal year (FY) 2004, the last year for which we have state-by-state data, except for one-time federal funding of $35 million for HIV testing in FY 2007. This is despite the fact that the CDC determined in August of 2008 that the number of new HIV infections in the U.S. is 40% higher than we thought it was – at about 56,000 per year.
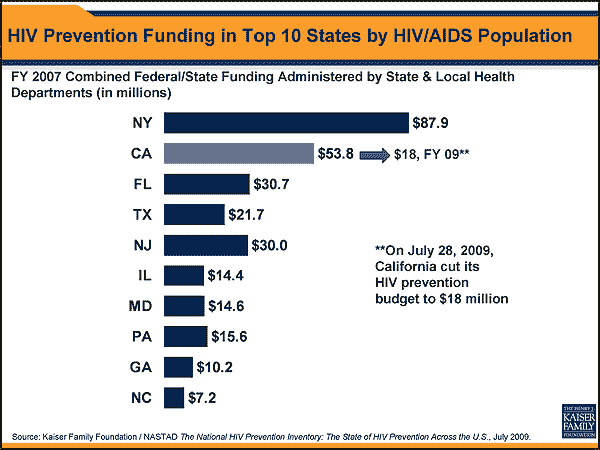
Second, and more striking, the absolute amount of money we spend on HIV prevention is quite small nationally and on a state-by-state basis. Nationally we spend less than $600 million in combined state and federal dollars for states to deliver HIV prevention services. But as the chart shows, the absolute amount of spending in the ten states with the largest numbers of people living with HIV/AIDS is modest, ranging from about $7 million in North Carolina to a high of $88 million in New York. These are the latest comprehensive state-by-state data, but they are from FY 2007 and many states have faced serious budget shortfalls since then and have cutback or may soon cutback programs. The most glaring example is California which just this week cut its HIV prevention spending drastically – by more than 80% in state funds – in the middle of its widely reported budget debacle, bringing total HIV prevention spending in California from about $50 million to $18 million, a tiny number in a state larger than most nations.
There are a few simple points to be made here. First, while more needs to be done to target and fine tune prevention interventions (we have to improve prevention not just spend on it), scale and intensity are always important; these amounts are not big enough in most states for a prevention strategy to operate at scale or to reach high risk groups with sustained interventions of the intensity needed. Second, while treatment is inherently more expensive than prevention – and it is not appropriate to directly compare spending on treatment with spending on prevention – it is obvious that the treatment agenda has driven out prevention in recent years. Partly this is because it required funding to ramp up treatment services and partly this is because prevention became ensnarled in broader controversies about social issues.
Virtually every issue we work on in health makes a claim for more money and usually a valid one. In the real world of budget priorities there are many legitimate needs that have to compete for scarce dollars and not all needs can be met, especially in today’s economy and the budget environment at the federal and state levels. But even in a world of competing needs, the small size of the investment we are making in HIV prevention revealed in this report stands out.
