How Will the Uninsured in Pennsylvania Fare Under the Affordable Care Act?
The 2010 Affordable Care Act (ACA) has the potential to extend coverage to many of the 47 million nonelderly uninsured people nationwide, including the 1.4 million uninsured Pennsylvanians. The ACA establishes coverage provisions across the income spectrum, with the expansion of Medicaid eligibility for adults serving as the vehicle for covering low-income individuals and premium tax credits to help people purchase insurance directly through new Health Insurance Marketplaces serving as the vehicle for covering people with moderate incomes. With the June 2012 Supreme Court ruling, the Medicaid expansion became optional for states, and as of August 2014, Pennsylvania was planning to implement the expansion in 2015.1 As a result, almost all nonelderly uninsured, most of whom are adults, will become eligible for coverage under the ACA coverage expansions. As the coverage expansions are implemented and coverage changes are assessed, it is important to understand the potential impact of the law in the state.
How Will the ACA Expand Health Insurance Coverage in Pennsylvania?
Historically, Medicaid had gaps in coverage for adults because eligibility was restricted to specific categories of low-income individuals, such as children, their parents, pregnant women, the elderly, or individuals with disabilities. In most states, adults without dependent children were ineligible for Medicaid, regardless of their income, and income limits for parents were very low—often below half the poverty level.2 The ACA aimed to fill in these gaps by extending Medicaid to nearly all nonelderly adults with incomes at or below 138% of poverty (about $32,900 for a family of four in 2014).
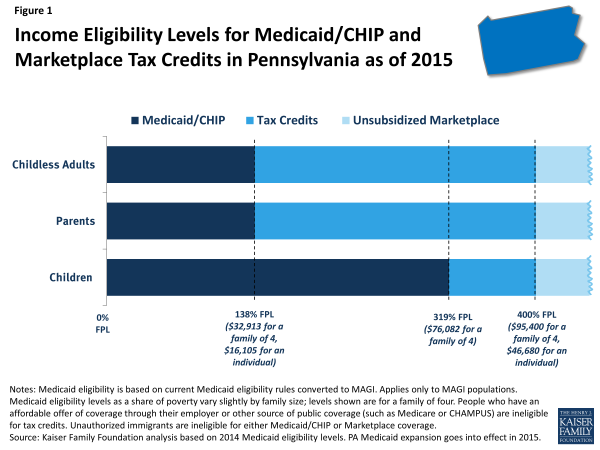 Beginning in 2015, Medicaid eligibility in Pennsylvania will cover almost all nonelderly adults up to 138% of poverty, as shown by the dark blue shading in Figure 1. All states previously expanded eligibility for children to higher levels than adults through Medicaid and the Children’s Health Insurance Program (CHIP). In Pennsylvania, children with family incomes up to 319% of poverty (about $76,100 for a family of four) are already eligible for Medicaid or CHIP prior to the implementation of the Medicaid coverage expansions under the ACA. As was also the case before the ACA was implemented, undocumented immigrants will remain ineligible to enroll in Medicaid, and recent lawfully residing immigrants are subject to certain Medicaid eligibility restrictions.3
Beginning in 2015, Medicaid eligibility in Pennsylvania will cover almost all nonelderly adults up to 138% of poverty, as shown by the dark blue shading in Figure 1. All states previously expanded eligibility for children to higher levels than adults through Medicaid and the Children’s Health Insurance Program (CHIP). In Pennsylvania, children with family incomes up to 319% of poverty (about $76,100 for a family of four) are already eligible for Medicaid or CHIP prior to the implementation of the Medicaid coverage expansions under the ACA. As was also the case before the ACA was implemented, undocumented immigrants will remain ineligible to enroll in Medicaid, and recent lawfully residing immigrants are subject to certain Medicaid eligibility restrictions.3
Under the ACA, people with incomes between 100% and 400% of poverty may be eligible for premium tax credits when they purchase coverage in a Marketplace, as indicated by the bright blue shading in Figure 1. The amount of the tax credit is based on income and the cost of insurance, and tax credits are only available to people who are not eligible for other coverage, such as Medicaid/CHIP, Medicare, or employer coverage, and who are citizens or lawfully-present immigrants. Citizens and lawfully-present immigrants with incomes above 400% of poverty can purchase unsubsidized coverage through the Marketplace.
How Many Uninsured Pennsylvanians Will Be Eligible for Financial Assistance Under the ACA in 2015?
With Pennsylvania deciding to implement the Medicaid expansion in 2015, nearly three-quarters (72%) of nonelderly people in the state who were uninsured prior to the ACA coverage expansions will become eligible for financial assistance for coverage available through either Medicaid or the Marketplace (Figure 2).
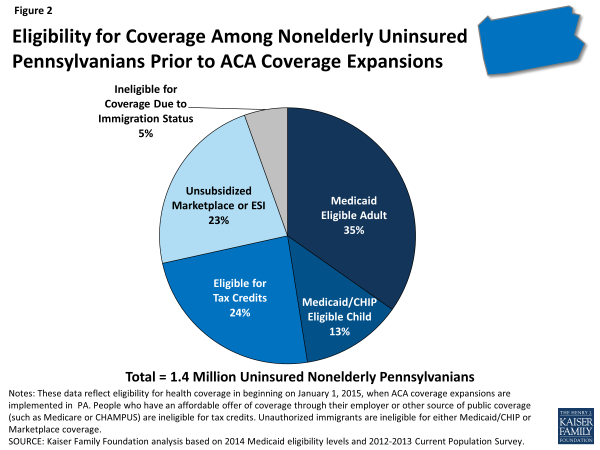 Given the income distribution of the uninsured in the state, the main pathway for coverage will be Medicaid once the Medicaid expansion is implemented in the state, with nearly half (48%) of uninsured Pennsylvanians eligible for either Medicaid or CHIP as of January 1, 2015. While some of these people (such as eligible children) are eligible for health coverage under pathways that were in place before the ACA coverage expansions, most adults are newly-eligible through the Medicaid expansion. Nearly one in four (24%) of all uninsured people in Pennsylvania will be eligible for premium tax credits to help them purchase coverage in the Marketplace in 2015.
Given the income distribution of the uninsured in the state, the main pathway for coverage will be Medicaid once the Medicaid expansion is implemented in the state, with nearly half (48%) of uninsured Pennsylvanians eligible for either Medicaid or CHIP as of January 1, 2015. While some of these people (such as eligible children) are eligible for health coverage under pathways that were in place before the ACA coverage expansions, most adults are newly-eligible through the Medicaid expansion. Nearly one in four (24%) of all uninsured people in Pennsylvania will be eligible for premium tax credits to help them purchase coverage in the Marketplace in 2015.
Other uninsured Pennsylvanians may gain coverage under the ACA but will not receive direct financial assistance. These people include the 23 percent with incomes too high to be eligible for premium tax subsidies or who have an affordable offer of coverage through their employer. Some of these people will still be able to purchase unsubsidized coverage in the Marketplace, which may be more affordable or more comprehensive than coverage they could obtain on their own through the individual market in 2015. Lastly, approximately 5 percent of uninsured people in Pennsylvania who are undocumented immigrants will be ineligible for financial assistance under the ACA and barred from purchasing coverage through the Marketplaces. This group is likely to remain uninsured, though they will still have a need for health care services.
***
The ACA will help many Pennsylvanians who were uninsured prior to the ACA coverage expansions gain health coverage by providing coverage options across the income spectrum for low and moderate-income people. While almost all of the uninsured in Pennsylvania will become eligible for some type of coverage under the ACA in 2015, the impact of the ACA will depend on take-up of coverage among the eligible uninsured, and outreach and enrollment efforts will be an important factor in decreasing the uninsured rate. The ACA includes a requirement that most individuals obtain health coverage, but some people (such as the lowest income or those without an affordable option) are exempt and others may still remain uninsured. Continued attention to who gains coverage as the ACA is fully implemented and who is excluded from its reach—as well as whether and how their health needs are being met—can help inform decisions about the future of health coverage in Pennsylvania.
Endnotes
Pennsylvania received approval of a Section 1115 waiver for the Medicaid expansion. Coverage under the expansion will go into effect on January 1, 2015.
Some states had expanded coverage to parents at higher income levels or provided coverage to adults without children. See http://www.kff.org/medicaid/fact-sheet/medicaid-eligibility-for-adults-as-of-january-1-2014/ for more detail on pre- and post-ACA Medicaid eligibility for adults.
For more detail on Medicaid coverage for immigrants, see: http://www.kff.org/disparities-policy/fact-sheet/key-facts-on-health-coverage-for-low/.
