Pulling it Together: Reflections on This Year’s Four Percent Premium Increase
Our 2012 Employer Health Benefits Survey found a 4% increase in premiums this year, continuing the recent trend of moderation in health costs and spending reported in several studies. Double digit increases in premiums were once a common occurrence, but we have not seen any since a 10% increase in 2004 and 13% growth in 2003. Rates of increase in total health spending have been holding at 4-6% per year recently, and per capita spending — which is most analogous to premiums — has been rising about a percentage point below that. These are strikingly low numbers to those of us who have been studying health costs for a long time. A 4% increase in health premiums is good news, although good news is seldom “news.” But will it last?
No one has yet been able to disentangle the causes of the slowdown persuasively. Health care use and the economy have always been closely tied, and my sense is that the recession and slow recovery are responsible for much of the recent health spending and premium trends. Increases in recent years in cost sharing through high deductible plans have probably played a supporting role. In tough times, when wages are flat, people avoid using the health care system if they can. We also know that higher out-of-pocket costs deter utilization, so it’s reasonable to assume that the growth of high-deductible plans and other forms of cost sharing has had an impact on health care use, magnifying the effect of the economy.
There is no perfect database that will enable us to spot a new wave of utilization building back up just over the horizon. Insurers can often spot trends in their claims and the publicly held companies sometimes give clues as to what’s going on in their quarterly earnings statements. Recent reports suggest that utilization may be starting to pick up modestly, at least for outpatient services.
Using data from our employer survey, Exhibit 1 shows cumulative premium increases for the years before and after the recession, suggesting (but not proving) the influence of economy on premium trends.
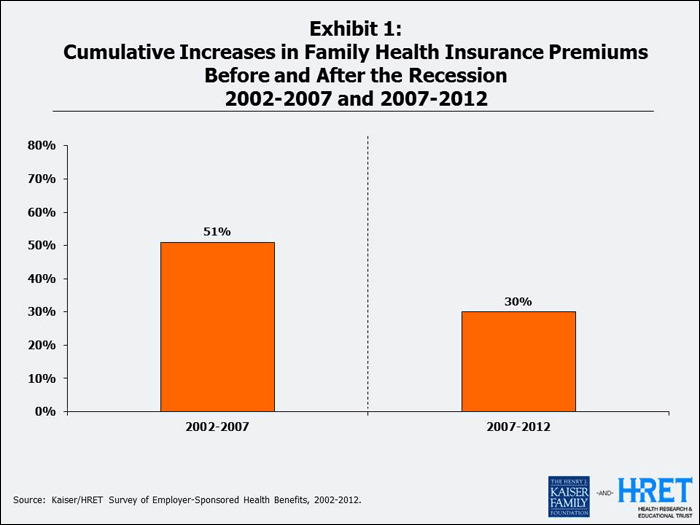
Some observers think the cumulative effects of delivery and payment reform efforts across the country may also be playing a role in holding down costs. Employers, insurers, and providers have been organizing a range of efforts to reduce costs and improve quality. These efforts are promising, but they also tend to be locally based and small scale. Some focus on one employee group, or disease group, or on the efforts of one insurance plan in a state. The largest effort to encourage payment and delivery reform, the Medicare payment and delivery experiments funded under the Affordable Care Act, are only just beginning. Our colleagues at the Commonwealth Fund recently estimated that there are today about 2.4 million Medicare beneficiaries being served by providers participating in Accountable Care Organizations, far too few to impact costs nationally. The Congressional Budget Office has thus far been unwilling to score savings for delivery reform, at least as it has been embodied in legislative form. Whatever the promise of these efforts to reduce costs, experience to date is mostly small scale. Previous efforts produced mixed results according to the most rigorous evaluations we have, and we don’t have much new evidence yet.
Then there are chronic disease management programs. And wellness programs. And tighter managed care. It is possible that it is not any one thing but somehow the combined effect of all of these things that is holding back cost increases. Like other theories, the “all of the above” theory is not provable, at least not yet. Many claims are being made about current efforts to hold down costs – some in the interest of understanding what is happening in a complex health care system, others not entirely disinterested. The truth is that what we don’t know about the causes of the slowdown and the efficacy of current efforts exceeds what we do know by a wide margin. Our colleague, the health economist Gail Wilensky, said essentially the same thing in The New York Times not too long ago: “If there’s something else going on, we don’t know what it is yet. The most honest thing to say is that, one, the reduction in use is greater than the recession predicts; two, we don’t understand why yet; and, three, you’d be foolhardy to say that we can understand it.” My sense, from watching these trends for many years, is that explanations that focus on the recession and the economy, and secondarily on the recent growth in cost sharing and high deductible plans, are the most plausible. In the small group market where fewer firms are self-insured, it is also possible that recent medical loss ratio and rate review regulations are having some effect.
With the economy only slowly recovering and wage stagnation depressing utilization, there is no reason to expect a return to double digit increases in health insurance premiums anytime soon, if at all. Other new variables could also change the cost picture moving forward, including the implementation of the Affordable Care Act and reductions in Medicare or Medicaid spending that might arise out of budget talks. At the same time, there has been no obvious change in the fundamental underlying drivers of medical costs or in the delivery of, or payment for, medical services that should lead us to think that the recent historically low increases in health costs represents a “new normal.” There is no bigger or more challenging problem in health care than controlling costs, and the recent good news about premium increases is no reason to assume the problem is solved or to back off of new efforts to address it.
